Unveiling the Anti-Inflammatory Diet: How Whole Plant Foods Combat Chronic Inflammation and Reduce Mortality Risk

Chronic inflammation, a persistent low-grade immune response, has emerged as a critical underlying factor in the development and progression of numerous age-related diseases and premature mortality. Understanding and effectively mitigating this silent threat is paramount for healthy aging, and growing scientific evidence points towards dietary interventions as a powerful, accessible tool. Indeed, as a pivotal study highlighted, "Intervention studies to enhance healthy ageing need appropriate outcome measures, such as blood-borne biomarkers, which are easily obtainable, cost-effective, and widely accepted." These biomarkers, notably C-reactive protein (CRP) and Interleukin-6 (IL-6), offer quantifiable insights into an individual’s inflammatory status and, crucially, their long-term health prospects.
The Silent Threat: Understanding Inflammatory Biomarkers and Mortality Risk
C-reactive protein (CRP) is one of the most extensively studied inflammatory biomarkers, routinely measured in blood tests. Elevated levels of CRP are not merely indicators of an active inflammatory process but are also strongly correlated with an increased risk of premature death. Research indicates that individuals with higher circulating levels of CRP may face a staggering 42% increased risk of dying prematurely. This acute phase reactant, produced by the liver in response to inflammation, serves as a general marker of systemic inflammation, often associated with cardiovascular disease, metabolic syndrome, and certain cancers.
Beyond CRP, Interleukin-6 (IL-6) stands out as another potent inflammatory cytokine with significant prognostic value. IL-6 is a pro-inflammatory mediator involved in various immune responses and is implicated in chronic inflammatory conditions, autoimmune diseases, and even depression. Studies have shown that individuals exhibiting the highest levels of IL-6 face an even greater risk, potentially increasing their premature death risk by as much as 49%. These statistics underscore the urgent need for strategies to effectively lower these inflammatory markers within the general population.
The pervasive nature of chronic inflammation in modern society is often linked to lifestyle factors, with diet playing a central role. While certain foods are known to exacerbate inflammatory pathways, a growing body of research is illuminating the profound anti-inflammatory potential of specific dietary components and patterns.
Diet’s Dual Role: Fueling or Fighting Inflammation

Previous discussions and extensive research have identified foods that actively contribute to systemic inflammation. These typically include highly processed meats, refined sugars, and diets rich in saturated and trans fats, which can disrupt the gut microbiome, promote oxidative stress, and trigger immune responses. Conversely, certain foods have demonstrated remarkable abilities to attenuate this inflammatory cascade, offering a pathway to better health and longevity. The critical question then becomes: what specific foods possess these anti-inflammatory properties, and how can they be integrated into daily diets?
Berries: Nature’s Potent Anti-Inflammatory Agents
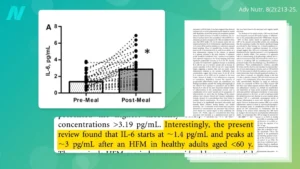
The power of whole, unprocessed foods in combating inflammation is vividly illustrated by studies on berries. Consider an experiment where participants consumed a high-fat, high-glycemic-load meal composed of common pro-inflammatory culprits: white potatoes, white bread, ham, cheese, and butter. Such a meal is typically expected to induce a significant inflammatory response. However, the addition of a mere single cup of blueberries to this otherwise inflammatory meal led to a statistically significant drop in IL-6 levels. This compelling finding suggests that the potent compounds within blueberries can counteract the inflammatory impact of an otherwise unhealthy meal, offering a buffer against immediate post-meal inflammatory surges.
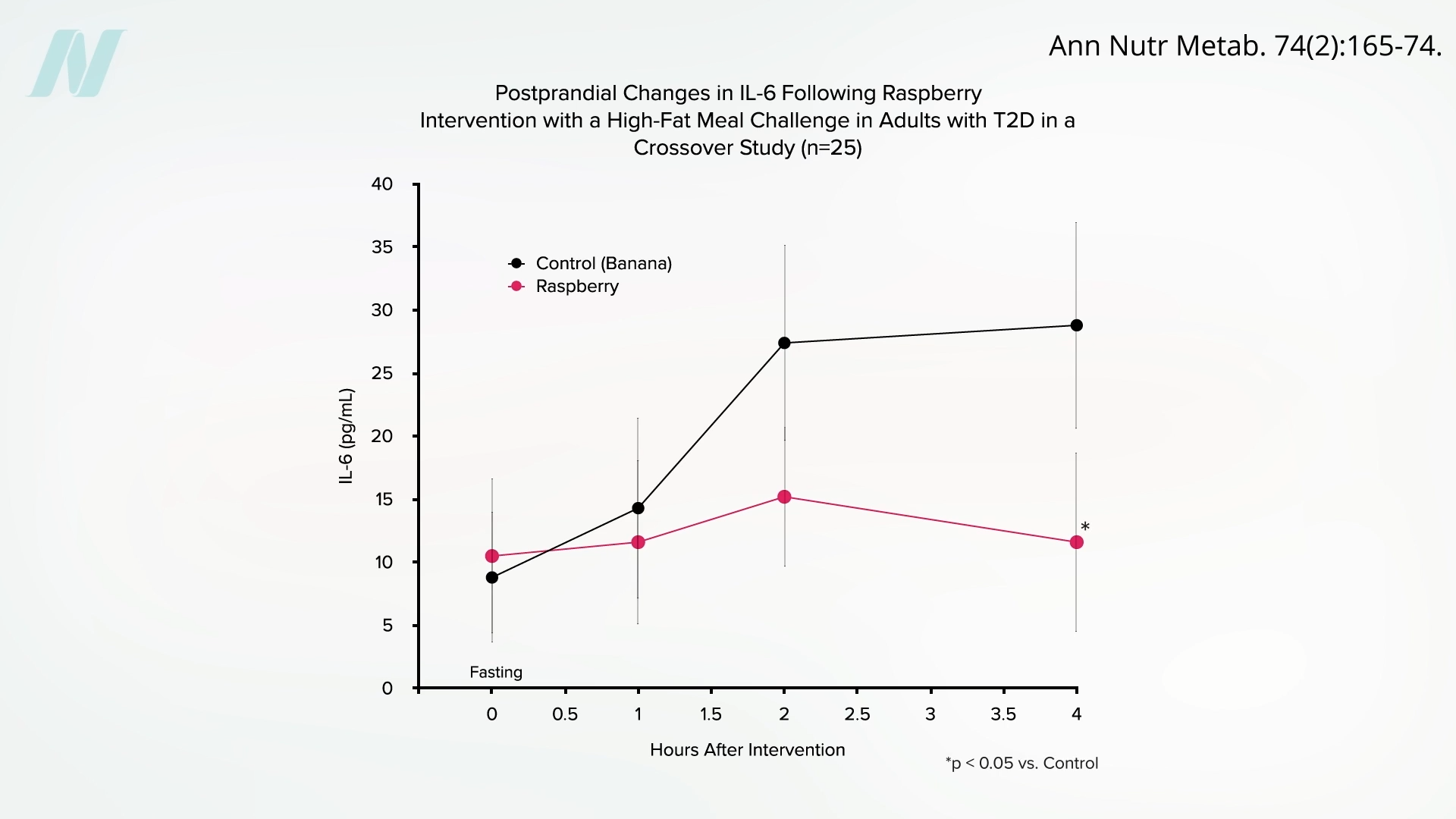
Further research extended these findings to other berries. In another study, participants were fed a meal notoriously high in inflammatory triggers, including eggs, butter, white potatoes, white flour biscuits, and sausage. One group consumed this meal alongside a smoothie containing two cups of frozen raspberries blended with water. A control group received an equivalent amount of calories and carbohydrates in the form of bananas. The results were stark: the pro-inflammatory meal alone, or with bananas, led to a tripling of IL-6 levels within four hours. In stark contrast, those who consumed the raspberries were able to "hold the line," preventing the dramatic spike in IL-6. This highlights raspberries’ ability to significantly mitigate the inflammatory response induced by a high-fat, high-carbohydrate, animal-product-rich meal.
The differential effect between raspberries and bananas begs the question of the underlying mechanisms. While bananas offer valuable nutrients, they lack the specific anti-inflammatory compounds abundant in berries. The primary candidates for berries’ anti-inflammatory prowess are their rich antioxidant content, particularly anthocyanins. These potent pigments are responsible for the vibrant red, blue, and purple hues of berries and have been the subject of numerous randomized controlled trials. These trials have consistently demonstrated the efficacy of anthocyanins in reducing inflammatory markers. It is crucial to note that while antioxidants are key, antioxidant supplements (such as vitamins C or E, beta-carotene, or selenium) have largely failed to replicate the benefits observed with whole foods, underscoring the synergistic effect of compounds within whole foods that cannot be isolated and bottled. Beyond berries, fruits like pomegranates, also packed with anthocyanin pigments, have been shown in multiple studies to reduce inflammation over time.
The Potent Role of Spices in Dietary Inflammation Control
Beyond fruits, the culinary world offers another powerful arsenal against inflammation: spices. Incorporating spices into meals presents a practical and effective approach to cool down systemic inflammation. However, the form in which these spices are consumed appears to be critical. For instance, a study exploring the effects of grape and turmeric extracts on the inflammatory response to a milkshake found no significant impact. This result contrasts sharply with research on whole turmeric.
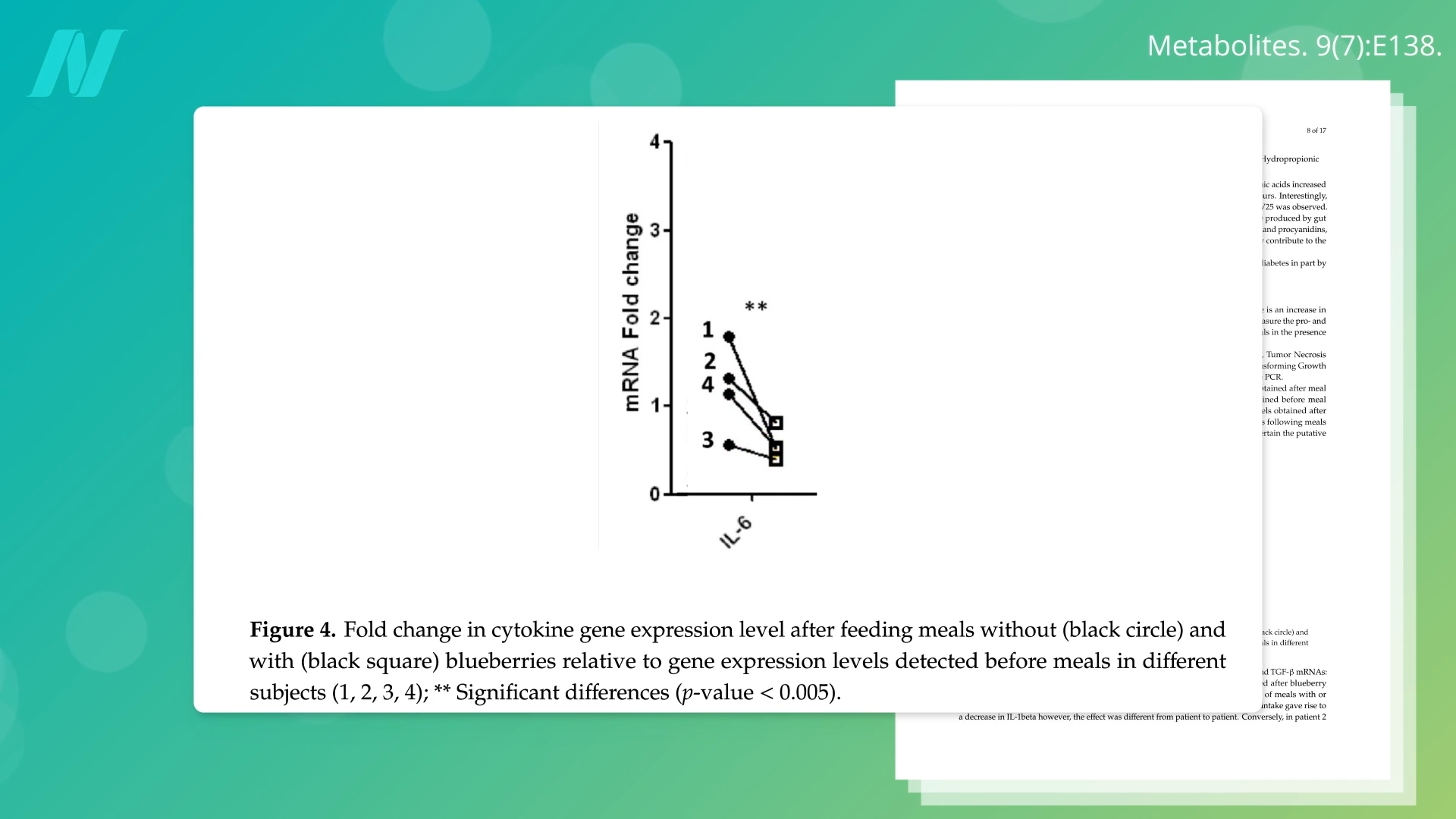
When individuals were given just one teaspoon a day of actual turmeric – the whole spice, not purified curcumin supplements – a significant drop in IL-6 levels was observed. This distinction between whole spices and isolated extracts is vital. Turmeric’s primary active compound, curcumin, is celebrated for its anti-inflammatory properties, but it appears that the full spectrum of compounds in the whole spice works synergistically to exert its maximal effect.
Other common kitchen spices also demonstrate remarkable anti-inflammatory capabilities. Garlic powder, even at a modest dose of about half a teaspoon a day, has been shown to reduce IL-6 levels. The active compounds in garlic, such as allicin, contribute to its well-documented health benefits, including its anti-inflammatory actions. Similarly, ginger powder (ground ginger) produced comparable results, with doses ranging from half a teaspoon to one and a half teaspoons daily effectively lowering inflammatory markers. Gingerols, the main active compounds in ginger, are known for their potent antioxidant and anti-inflammatory effects. These findings suggest that simply integrating these everyday spices into cooking can provide a consistent, low-cost strategy to manage chronic inflammation.
Embracing a Plant-Based Paradigm: Beyond Individual Foods
While specific foods and spices offer targeted benefits, the most profound and sustained impact on inflammation often comes from adopting a holistic dietary pattern. One immediate way to mitigate the inflammation caused by highly processed, animal-product-heavy meals, such as a "Sausage and Egg McMuffin," is, quite simply, to avoid them altogether. But what about the broader impact of a plant-based diet?
Early studies investigating the effects of generally plant-centered diets, such as the Mediterranean diet, on inflammatory markers sometimes yielded less dramatic results than expected, with the drop in IL-6 not always reaching statistical significance. This led researchers to ponder, "What exactly was the diet they actually ate?" The challenge lies in the variability of "plant-centered" or "Mediterranean" diets, which, while healthier than typical Western diets, may still include substantial amounts of animal products or less healthy plant-derived foods. These diets might not go "far enough" to elicit a truly significant anti-inflammatory effect.
To gain clearer insights, researchers turned to more rigorously defined dietary interventions, such as Dr. Turner-McGrievy’s landmark "New DIETs study." This study randomized participants into several distinct dietary groups: a control group continuing their fully omnivorous diets, and intervention groups adopting a vegan diet (no animal products), a vegetarian diet (dairy and eggs permitted), a pesco-vegetarian diet (fish permitted, no other meat), or a semi-vegetarian diet (limited red meat).
The dietary patterns were distinct:
- Omnivorous: A typical diet including all types of animal products.
- Semi-Vegetarian: Primarily plant-based but with limited intake of red meat and occasional poultry. For instance, dinner might include some turkey sausage.
- Pesco-Vegetarian: Excludes all meat except fish. A dinner might consist of shrimp with plant-based components.
- Vegetarian: Excludes all meat, poultry, and fish, but includes dairy and eggs. A vegetarian dinner could feature red beans and brown rice with chopped tomatoes and roasted peppers, supplemented with cheese.
- Vegan: Excludes all animal products. A vegan dinner would be entirely plant-based, such as red beans and brown rice with chopped tomatoes and roasted peppers.
The study aimed to measure changes in the Dietary Inflammatory Index (DII) scores over two months. The DII is a comprehensive measure that assesses the overall inflammatory potential of a diet, factoring in various food components and nutrients. Negative DII scores indicate an overall anti-inflammatory diet, with lower scores signifying a stronger anti-inflammatory effect. Conversely, positive scores denote a pro-inflammatory dietary pattern. Predictably, the participants, starting from regular omnivorous diets, began with positive, pro-inflammatory DII scores, reflecting the prevalent dietary habits in nations grappling with inflammation-related diseases.
The results were compelling. When participants switched to strictly plant-based nutrition – specifically the vegan, vegetarian, and pesco-vegetarian groups – their dietary patterns underwent a significant transformation, flipping to become decidedly anti-inflammatory, as evidenced by negative DII scores. This demonstrates that even cutting out only red meat (pesco-vegetarian) was sufficient to shift the dietary inflammatory profile. However, those who switched mostly to poultry or only limited their overall meat intake (semi-vegetarian and omnivorous groups) did not achieve this shift; their diets remained inflammatory. This underscores a crucial insight: for maximal anti-inflammatory benefits, a substantial reduction or complete elimination of animal products appears necessary.
Nuances of "Plant-Based": Quality Matters
It is critical to emphasize that merely adopting a "plant-based" label is not a guarantee of anti-inflammatory benefits. The quality of plant foods consumed is paramount. If a diet primarily consists of less healthy plant-derived foods such as fruit juices, white bread, white potatoes (especially when processed or fried), sugary sodas, and cakes, individuals can paradoxically end up even more inflamed. These highly refined plant foods often lack fiber and beneficial micronutrients while being high in sugar and unhealthy fats, triggering inflammatory responses similar to animal products.
However, when individuals commit to a truly clean diet centered on whole plant foods – encompassing fruits, vegetables, legumes, whole grains, nuts, and seeds in their minimally processed forms – the health benefits are profound and far-reaching. Such a diet has been shown to yield significant reductions in lipoprotein(a) (Lp(a)), a notoriously difficult-to-modify risk factor for cardiovascular disease that was once thought unresponsive to dietary changes. Additionally, robust drops in LDL cholesterol (the "bad" cholesterol) and even the most dangerous forms of LDL cholesterol are observed. Crucially, across the board, there are dramatic reductions in inflammatory markers: a remarkable 30% drop in C-reactive protein and a 20% drop in IL-6.
These findings strongly suggest that the limited success of some previous studies with "plant-centered" diets may have stemmed from their insufficient adherence to truly whole plant-based principles, with animal products still being substantially consumed or processed plant foods dominating. Therefore, the scientific consensus increasingly points towards the "total elimination of animal products and processed foods" as a more prudent and effective dietary strategy to combat chronic inflammation.
Broader Implications and Public Health Perspective

The implications of these dietary findings are profound, extending beyond individual health choices to public health policy and preventive medicine. As chronic inflammatory diseases continue to burden healthcare systems globally, understanding and promoting effective dietary interventions becomes a critical public health imperative. Shifting dietary guidelines to emphasize whole plant foods and minimize processed foods and animal products could lead to significant reductions in the prevalence of heart disease, type 2 diabetes, certain cancers, and autoimmune conditions.
However, implementing such a widespread dietary shift presents challenges. Public education is crucial to clarify the distinction between "plant-based" and "whole food, plant-based" to ensure that individuals make informed, health-promoting choices. Accessibility to affordable whole plant foods, along with culinary education, will also be vital in enabling populations to adopt and sustain these beneficial dietary patterns.
Ultimately, the body of evidence unequivocally demonstrates that diet is not merely a source of sustenance but a powerful modulator of our internal inflammatory environment. By consciously choosing anti-inflammatory foods like berries, incorporating potent spices, and embracing a comprehensive whole food, plant-based dietary pattern, individuals can significantly reduce their risk of chronic inflammation, lower critical mortality biomarkers, and pave the way for a healthier, longer life. The control over our inflammatory fate largely lies on our plates.