Prioritizing Safety: The Ethical Imperative of Trauma-Informed Resilience Building in Mental Healthcare
In the aftermath of profound adversity, the impulse to foster growth and resilience often drives therapeutic interventions. However, a growing consensus among mental health professionals highlights a critical distinction: forcing growth without first establishing psychological safety can inadvertently lead to retraumatization, delaying genuine healing and undermining the very resilience it seeks to build. This nuanced approach, known as trauma-informed resilience-building, advocates for a deliberate, phased methodology that respects the client’s nervous system capacity and lived experience, ensuring interventions are both effective and ethical.
The concept of resilience, traditionally understood as the ability to bounce back from adversity, has evolved significantly within the framework of trauma care. Modern understanding, informed by neurobiology and extensive clinical practice, recognizes that true resilience cannot be rushed or imposed. Instead, it emerges organically from a foundation of stability and safety. When individuals face trauma, grief, or betrayal, the lines between immediate stabilization, long-term resilience-building, and eventual post-traumatic growth (PTG) can easily blur. Experts, including licensed trauma therapist Dr. Laura Copley, underscore that this blurring can render even well-intentioned interventions harmful, leading to subtle forms of pressure, invalidation, toxic positivity, and premature growth.
Understanding Trauma-Informed Resilience in Practice
Trauma-informed resilience-building is fundamentally about developing adaptive capacity without bypassing essential steps related to safety, appropriate pacing, or the individual’s unique lived experience. It moves beyond a simplistic "pull yourself up by your bootstraps" mentality, recognizing the profound physiological and psychological impact of trauma. Instead, therapists are tasked with supporting the nervous system in ways that facilitate gradual forward movement, ensuring that the client’s internal resources are not overwhelmed.
This approach stands in stark contrast to practices that might prematurely push for cognitive reframing or meaning-making before a client feels secure. For instance, a common misstep involves urging clients to "make sense" of their trauma when their primary need is to feel safe enough to simply be present with their emotions and bodily sensations. The core principle is that the brain cannot effectively engage in higher-order processing, such as learning or integration, when it is in a state of hyperarousal (fight/flight) or hypoarousal (freeze/shutdown). In these survival-oriented states, the system prioritizes protection over growth, making any resilience-building efforts largely ineffective.

The Neurobiological Imperative: Stabilization First
The bedrock of trauma-informed resilience is stabilization. Before any meaningful resilience can be built, a client must achieve a baseline sense of safety. From a neurobiological perspective, regulation of the autonomic nervous system is the prerequisite for attention, learning, and integration. Pioneering work by researchers like Stephen Porges (Polyvagal Theory) and Daniel Siegel (Interpersonal Neurobiology) illustrates how a dysregulated nervous system, constantly oscillating between states of overwhelm and shutdown, cannot engage in the complex work of healing and growth. In such a state, the brain and body are organized around survival, not expansion.
This understanding informs the crucial sequence of therapeutic interventions. When a person is experiencing intense emotional dysregulation, flashbacks, dissociation, or persistent hypervigilance, their system is not ready for skills-based resilience work. Instead, the focus must shift from seeking insight into the trauma to establishing predictability and immediate safety.
Key Indicators a Client May Not Be Ready for Resilience-Building:
- Fluctuations in Arousal: Rapid shifts between hyperarousal (anxiety, panic, irritability) and hypoarousal (numbness, dissociation, fatigue).
- Difficulty Staying Present: Inability to focus on the current moment, persistent rumination, or feeling disconnected from their body.
- Overwhelm with Complexity: Struggling with multi-step instructions, feeling flooded by emotions, or experiencing cognitive fog.
- Lack of Basic Safety: Experiencing ongoing threats in their environment or an inability to identify internal or external resources for safety.
- Self-Harm or Suicidal Ideation: Indicating a severe lack of internal regulation and coping capacity.
In these instances, the most therapeutic action is often to slow down. Practical stabilization strategies prioritize simplicity and consistency. These can include orienting to the environment (e.g., noticing five things they can see, hear, or feel), engaging in sensory-based grounding techniques, establishing small, predictable daily habits and routines, and identifying reliable supportive individuals or resources. The aim is to help clients access brief, reliable moments of regulation they can consistently return to, thereby gently nudging the nervous system away from survival mode and towards a state conducive to healing.
Historical Context: A Shift in Trauma Treatment Paradigms

The evolution of trauma care provides crucial context for this phased approach. Early psychoanalytic models often focused on uncovering repressed memories, sometimes without sufficient attention to the client’s current capacity for integration. The rise of Cognitive Behavioral Therapy (CBT) introduced structured approaches, but some early applications could inadvertently push for cognitive restructuring before emotional regulation was established.
The late 20th and early 21st centuries saw a significant paradigm shift. Researchers like Judith Herman championed a three-stage model for complex trauma recovery (Safety and Stabilization, Remembrance and Mourning, Reconnection), emphasizing safety as the foundational first step. Concurrently, the Substance Abuse and Mental Health Services Administration (SAMHSA) articulated core principles of trauma-informed care: safety, trustworthiness and transparency, peer support, collaboration and mutuality, empowerment, voice, and choice, and cultural, historical, and gender issues. These principles underscore that healing is not just about symptom reduction but about restoring agency and trust within a supportive, non-hierarchical relationship. This historical progression highlights the increasing understanding that the how of trauma recovery is as vital as the what.
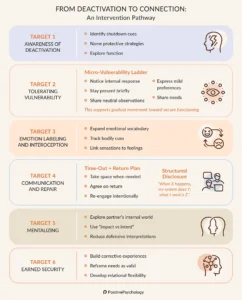
The Three-Phase Model: A Strategic Pathway to Healing
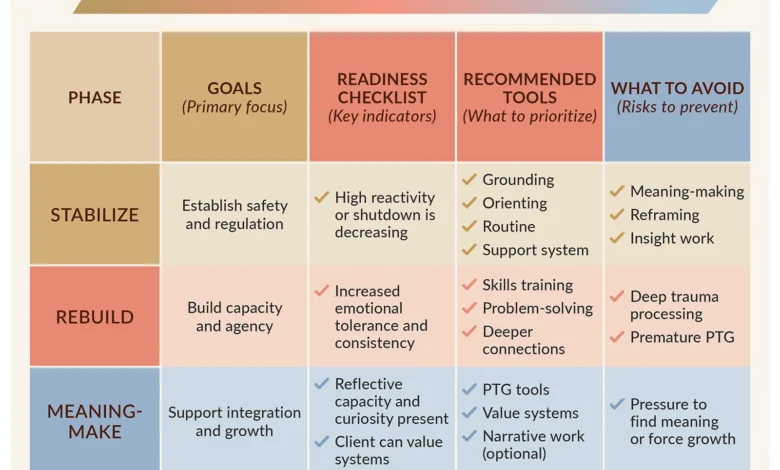
While healing is rarely linear, a strategic three-phase model offers a robust framework for clinicians: Stabilize → Rebuild → Meaning-Make. Each phase corresponds to a different level of nervous system capacity and necessitates distinct types of interventions. Moving prematurely into higher-order work, such as meaning-making, before foundational stabilization is achieved risks overwhelming the client and hindering progress.
Phase 1: Stabilization (Establishing Safety and Regulation)
- Readiness Markers: Client exhibits significant distress, dysregulation, or dissociation; unable to consistently stay present; reports feeling overwhelmed or shut down.
- Goal: Restore a baseline sense of safety, predictability, and nervous system regulation.
- Interventions: Grounding techniques (sensory, cognitive), breathwork, establishing routines, identifying external supports, psychoeducation on the nervous system, simple present-moment awareness practices, emotional containment strategies. The focus is on practical, repeatable actions that don’t require deep insight or complex cognitive processing.
Phase 2: Rebuilding Resilience Skills (Developing Capacity and Agency)

- Readiness Markers: Client demonstrates consistent emotional regulation; can return to a baseline state with greater ease; sustains attention for structured work; expresses a desire for active coping strategies.
- Goal: Expand adaptive capacity, foster a sense of agency, and develop practical skills for navigating challenges.
- Interventions: Skills-based training (e.g., distress tolerance, emotion regulation, interpersonal effectiveness from DBT), problem-solving skills, boundary setting, self-compassion practices, mindful awareness, identifying and leveraging personal strengths, gradual exposure to manageable stressors, rebuilding healthy relationships. At this stage, clients begin to reconnect with their internal resources and actively engage with their environment in manageable ways, shifting from merely surviving to actively responding.
Phase 3: Meaning-Making and Post-Traumatic Growth (Integration and Transformation)
- Readiness Markers: Client has robust emotional regulation; can reflect on experiences without becoming overwhelmed; expresses curiosity about the broader impact of their trauma; demonstrates a stable sense of self and purpose.
- Goal: Integrate the traumatic experience into their life narrative, explore personal growth, and find meaning (if desired).
- Interventions: Narrative therapy, exploration of values and purpose, identifying positive changes (e.g., increased empathy, strengthened relationships, new priorities), creative expression, altruism, spiritual exploration. This phase is characterized by a shift from merely enduring to actively integrating the experience, understanding its implications, and potentially discovering profound personal transformation.
It is crucial to emphasize that not all clients will desire or achieve post-traumatic growth, and that is entirely acceptable. A trauma-informed approach respects client autonomy, recognizing that meaning is something that may emerge naturally over time, not something that must be forced or created. The therapist’s role is to guide this phase with curiosity, offering invitations for exploration rather than expectations for growth.
Common Pitfalls and Ethical Considerations in Practice
Even with the best intentions, therapists can inadvertently cause harm by rushing the process or misaligning interventions with a client’s readiness. Reassurance, premature positive reframing, or highlighting meaning too soon can invalidate a client’s current pain or pressure them to feel something they are not ready for. It’s also important for clinicians to recognize their own discomfort with a client’s suffering and avoid the urge to "fix" or "reframe" prematurely.
Statements to Avoid vs. Trauma-Sensitive Alternatives:
- Instead of: "Everything happens for a reason."
Say: "I can only imagine how hard this is. I’m here with you." (Validates pain, offers presence) - Instead of: "Look on the bright side."
Say: "It makes sense that you feel [emotion]. We can take this at your pace." (Validates emotion, emphasizes pacing) - Instead of: "You’re so strong, you’ll get through this."
Say: "I see how hard you’re working. What do you need right now to feel a little safer?" (Acknowledges effort, focuses on immediate safety/needs) - Instead of: "What did you learn from this experience?" (Too soon for meaning-making)
Say: "When you’re ready, we can explore how this has impacted you. For now, let’s focus on what helps you feel grounded." (Offers future possibility, prioritizes current need)
These subtle shifts in language are vital for reducing pressure, reinforcing safety, and empowering clients to engage in resilience-building without bypassing their lived experience. They underscore the therapist’s commitment to attunement, validation, and pacing, which are cornerstones of trauma-informed care.

Broader Implications: Trauma-Informed Approaches Beyond Therapy
The principles of trauma-informed resilience extend far beyond the therapy room. Organizations across various sectors—education, healthcare, justice, social services, and even workplaces—are increasingly adopting trauma-informed approaches. This involves recognizing the widespread impact of trauma, understanding potential paths for recovery, and integrating this knowledge into policies, procedures, and practices.
In educational settings, this might mean training teachers to recognize signs of trauma in students and respond with empathy and regulation strategies, rather than punitive measures. In healthcare, it involves creating environments that minimize re-traumatization during medical procedures and ensuring staff are sensitive to patients’ histories. In the workplace, it can translate to fostering psychological safety, providing support for employees experiencing distress, and creating flexible policies that acknowledge the human impact of adversity. The broader societal implication is a shift towards systems that are inherently more compassionate, understanding, and conducive to collective well-being, recognizing that unaddressed trauma carries significant societal and economic costs.
Expert Perspectives and Best Practices
Dr. Laura Copley, a leading voice in complex trauma healing, consistently emphasizes that effective resilience-building is about precision and care. Her work, including her book "Loving You is Hurting Me," highlights the blend of psychoeducation, storytelling, and practical strategies needed to support individuals on their journey towards post-traumatic growth. The consensus among experts is clear: the therapist’s role is not to teach or push resilience, but to create the conditions under which it can organically emerge from within the client. This requires careful attunement to the client’s current nervous system capacity and a commitment to meeting them exactly where they are.
For practitioners, this means continuously refining their responses to better match a client’s current state. For example, if a client presents with intense anxiety and rapid speech, interventions focused on grounding and present-moment awareness are more appropriate than complex cognitive reframing. Conversely, a client exhibiting flat affect and withdrawal might benefit from gentle invitations to orient to their environment and identify small, tangible sensations to reconnect with their body. The "Quick-Start Guide: Choosing Interventions by Presentation" offers practical examples, linking client presentation (e.g., hyperarousal, hypoarousal, or dysregulation) to immediate, effective interventions (e.g., grounding, co-regulation, or predictable routines).

A Take-Home Message
The journey through trauma to resilience is deeply personal and often arduous. For therapists, the ethical imperative is to provide a safe, paced, and validating environment where clients can gradually regain their footing, rebuild their internal resources, and, if they choose, find meaning in their experiences. True resilience is not about avoiding pain or quickly moving past it; it is about developing the adaptive capacity to navigate distress with a sense of agency and self-trust. When interventions are aligned with a client’s readiness and nervous system capacity, resilience ceases to be a goal to be taught and instead becomes an inherent capacity that blossoms naturally.
Frequently Asked Questions
- Can resilience-building begin immediately after a traumatic event?
Yes, but in smaller, foundational ways. Immediate interventions focus on stabilization and safety-building, which are prerequisites for developing long-term resilience. - How can therapists avoid "toxic positivity" when discussing resilience?
Prioritize validation and pacing over reassurance or premature positive reframing. Allow clients the space to experience their emotions without judgment, moving toward meaning-making only when they express readiness. - Are resilience and recovery the same thing?
No. Resilience refers to an individual’s adaptive capacity to cope with and adapt to adversity. Recovery involves a broader healing process that may or may not include post-traumatic growth, but it often entails symptom reduction and functional improvement.








