Unmasking Menopause: How Brain Fog and Mood Swings are Often Misdiagnosed as Depression
A pervasive and often debilitating cognitive fog, coupled with profound emotional instability, is increasingly recognized as a significant yet frequently misdiagnosed symptom of menopause, leading many women down a frustrating path of seeking treatment for depression when the underlying cause is hormonal. This critical issue came into sharp focus through the personal experience of one individual who, in her late 40s and early 50s, found her once-sharp mind clouded, struggling to recall simple proper nouns or maintain focus during her workday. This experience, initially dismissed as typical age-related forgetfulness, escalated into a severe mental and emotional drain, mirroring symptoms commonly associated with clinical depression.
The Personal Ordeal of Cognitive Decline and Misdiagnosis
For nearly two years, the individual described a mental state akin to having her thoughts buried under a "pile of garbage." Simple tasks, such as remembering a restaurant’s name, became monumental struggles. A conversation about dinner plans would devolve into vague descriptions and frustrated attempts to retrieve basic information, only for the name to resurface hours later, unbidden and untimely. Beyond these frustrating lapses in recall, her professional life suffered immensely. Staring at a computer screen, she would find herself unable to initiate constructive work, describing her mental state as "hazy," much like the groggy moments after waking. While mornings offered brief windows of clarity, allowing her to cram hours of work into a fraction of the time, "worst days" brought an unshakeable haze, rendering her incapable of work, reading, or engaging in meaningful activity.
This distressing decline prompted her to seek medical advice from multiple healthcare professionals. The initial and repeated recommendations were for antidepressants, which she tried in various forms and dosages, only to feel "even worse" or "like a zombie." A sleeping pill further exacerbated her drugged sensation. Extensive tests for thyroid issues and anemia yielded no answers. Desperate, she experimented with a myriad of supplements, "mushroom coffee," and products marketed for cognitive enhancement, all to no avail. The breakthrough came almost by chance during a routine gynecological exam. A mention of vaginal dryness prompted a series of questions from her gynecologist about sleep, mood, energy levels, hot flashes, and crucially, brain fog. It was then, in a "hazy monotone," that she articulated her profound feeling of being "barely alive," leading to the revelation that her struggles were not depression, but the multifaceted symptoms of menopause.
Understanding the Menopausal Transition and its Broad Impact
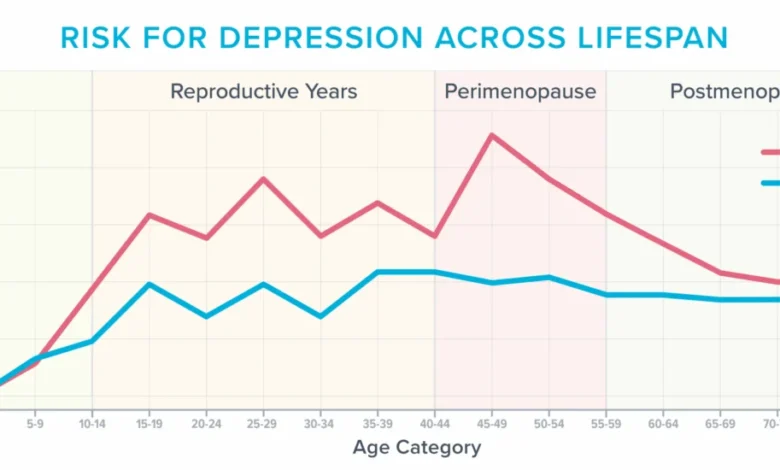
Menopause is not a disease but a natural biological stage in a woman’s life, marking the end of her reproductive years. It is officially diagnosed after 12 consecutive months without a menstrual period. The period leading up to menopause, known as perimenopause, can begin years earlier, often in a woman’s 40s. During both perimenopause and menopause, fluctuating and declining levels of hormones, particularly estrogen and progesterone, trigger a wide array of symptoms. While common symptoms like weight gain and reduced libido often receive significant attention, cognitive and emotional disturbances are equally, if not more, prevalent and impactful.
According to the American College of Obstetricians and Gynecologists, approximately 40 percent of women report increased irritability, mood swings, anxiety, fatigue, and difficulty concentrating during and after menopause. This period is also identified as one of the most vulnerable times in a woman’s life for developing depression, a risk that is significantly amplified if she has a history of mental health struggles. The individual’s experience of inexplicable sobbing, heightened sensory sensitivity where normal sounds felt physically painful, and pervasive anxiety about previously mundane situations (like driving over bridges) perfectly illustrates the profound emotional shifts that can occur.
The Neurological Underpinnings: Hormones, Hot Flashes, and Sleep
The precise mechanisms driving these cognitive and emotional symptoms are complex, likely involving a combination of fluctuating hormone levels and typical age-related changes in brain structure and function. However, a less understood but critical factor is the role of vasomotor symptoms (VMS), commonly known as hot flashes during the day and night sweats at night. These episodes, far from being mere inconveniences, are increasingly recognized by experts as a treatable medical condition with significant implications for brain health.
During a hot flash, the body undergoes a cascade of physiological changes: norepinephrine and cortisol levels surge, blood vessels dilate in an attempt to dissipate heat, and both blood pressure and heart rate increase. While the exact trigger for hot flashes during menopause remains elusive, one prominent theory posits that falling estrogen levels disrupt the hypothalamus, the brain region responsible for temperature regulation, causing its internal thermostat to malfunction.
Emerging research indicates that VMS can have direct, detrimental effects on the brain and its vascular system. A study involving 226 women, utilizing monitors to track hot flashes and MRI scans to image their brains, revealed a striking correlation. Women experiencing more frequent hot flashes showed an abundance of "whole-brain white matter intensities" – patchy areas once considered a normal part of aging. However, neuroscientists now link these lesions to an increased risk of future cognitive decline, doubling the likelihood of dementia and tripling the risk of stroke. This vascular connection is further supported by a three-year study of 492 women, which found that those with frequent hot flashes also exhibited unhealthy changes in their blood vessels, such as impaired ability to dilate. Additionally, frequent hot flashes have been linked to increased levels of inflammatory markers, oxidative stress, and carotid intima-media thickness, all indicators of compromised vascular health.
Beyond these direct vascular effects, VMS severely impact the brain through profound sleep disruption. Many women, like the individual in this article, may not realize that hot flashes are the culprit behind their fragmented sleep, often attributing their awakenings to insomnia or sleep apnea. This misattribution occurs because the intense heat of a night sweat often dissipates by the time a woman is jolted awake by the surge of cortisol and norepinephrine, leaving her to wonder why she’s waking repeatedly. These frequent, often unnoticed, awakenings critically interfere with the brain’s ability to consolidate memories, metabolize toxins, and store new information. Chronic sleep loss also leads to reduced connectivity in the hippocampus, vital for learning and memory, and increases the reactivity of the amygdala, the brain’s emotional center, making individuals more prone to stress, anxiety, irritability, and rage. These detrimental brain changes can manifest after just days of disrupted sleep, underscoring the severe impact of years of menopausal sleep disturbances.
Navigating the Medical Landscape: Barriers to Accurate Diagnosis

The journey to an accurate diagnosis for menopausal symptoms is often fraught with challenges. A significant hurdle lies in the overlap of symptoms between menopause-related sleep deprivation and clinical depression. Standard diagnostic tools, such as the Patient Health Questionnaire (PHQ-9) depression scale, include items like trouble sleeping, fatigue, changes in appetite or weight, and feeling down or hopeless. A woman experiencing menopausal night sweats, brain fog, and mood swings could easily check off enough of these symptoms to receive a depression diagnosis, inadvertently masking the true underlying cause.
Furthermore, a systemic lack of menopause-specific training within the medical community exacerbates the problem. Surveys reveal that a staggering 80 percent of medical residents admit to feeling "barely comfortable" discussing menopause. Few residency programs, including those for obstetrics and gynecology, offer comprehensive training in menopausal health. This educational gap explains why many healthcare professionals fail to inquire about hot flashes or sleep disturbances when patients present with fatigue, lack of motivation, and cognitive difficulties.
Even when vasomotor symptoms are clearly identified as contributing to cognitive and emotional distress, many healthcare professionals remain hesitant to prescribe Menopausal Hormone Therapy (MHT), also known as Hormone Replacement Therapy (HRT). This reluctance, as described by Michigan-based menopause-trained gynecologist Dr. Jerrold H. Weinberg, often stems from "defensive medicine," driven by fear of litigation rather than current medical evidence.
Re-evaluating Menopausal Hormone Therapy (MHT): Dispelling Misconceptions
The widespread apprehension surrounding MHT largely originates from research conducted decades ago, which linked certain types of hormones to a slightly increased risk of breast cancer or stroke. However, more recent and nuanced research has significantly refined this understanding. It is now recognized that the magnitude of these risks is highly dependent on factors such as the woman’s age, the specific dose and type of hormonal preparation, and the duration of hormone use.
Current consensus among many experts is that for women under 60 and within 10 years of their last menstrual period, particularly those experiencing moderate to severe menopausal symptoms, the benefits of MHT often outweigh the risks. Dr. Weinberg emphasizes that MHT offers substantial health benefits, including a reduced risk of developing Alzheimer’s disease and osteoporosis, which can counterbalance the small increased risks for most women. While some antidepressants can alleviate mood disturbances, improve sleep, and even reduce hot flashes, they come with their own set of side effects and, from a defensive medicine perspective, may be perceived as a "safer bet" by some clinicians compared to MHT. However, for many women, addressing the hormonal imbalance directly through MHT offers a more comprehensive and effective solution.
Empowering Women: Strategies for Effective Healthcare Advocacy
Given the complexities of diagnosis and treatment, women experiencing menopausal symptoms must become proactive advocates for their own health. Dr. Weinberg and Helen Kollias, PhD, a physiology and molecular biology expert and science advisor at Precision Nutrition and Girls Gone Strong, offer critical advice:
- Seek Menopause-Trained Health Professionals: Prioritize practitioners who explicitly list "menopause" as an area of focus in their bios or hold certifications from organizations like the Menopause Society (formerly NAMS). Online databases can help locate such specialists.
- Document Symptoms Meticulously: Maintain a detailed log of symptoms, including their nature, frequency, severity, and impact on daily life. This documentation serves as an objective record, invaluable during appointments where cognitive fog or anxiety might hinder clear communication. Track hot flashes (time, intensity, triggers), sleep patterns (duration, awakenings, quality), mood fluctuations, cognitive issues (memory lapses, concentration difficulties), and energy levels.
- Be Specific in Communication: General statements like "I don’t sleep well" are less effective than precise details. For example, stating, "During the past seven days, I’ve only achieved four uninterrupted hours of sleep once. I wake, on average, five times a night, with my longest sleep stretch being three hours," provides actionable information. If using smartwatches or fitness trackers, be prepared to share the data.
- Engage in Shared Decision-Making: Actively participate in discussions about treatment options, including their benefits and risks. This collaborative approach, encouraged by many healthcare networks, fosters trust and can help shift clinicians away from a defensive mindset. Ask pointed questions such as: "What are the specific benefits of this treatment for my symptoms?" "What are the potential risks, and how do they compare to the risks of not treating my condition?" "Are there alternative treatments, and how do their risks and benefits compare?"
Holistic Approaches: Lifestyle Interventions for Menopausal Well-being
Beyond medical interventions, a range of lifestyle strategies can significantly improve mental and emotional health during menopause. These are not drastically different from general health recommendations but become even more critical during this transitional phase.
- Lean into Fundamental Health Strategies: Re-evaluate and reinforce foundational health behaviors. Ensure adequate intake of nutrient-dense foods, engage in regular physical activity, practice effective stress management, prioritize restorative sleep, cultivate social connections, and maintain a sense of purpose. Critically assess barriers preventing adherence to these fundamentals and seek ways to overcome them.
- Experiment with Creatine: This supplement, renowned for its role in muscle and bone health, also shows promise in bolstering mood, enhancing brain function, and reducing mental fatigue, even mitigating some negative effects of sleep deprivation. A daily dose of 5 to 7 grams of creatine monohydrate is often recommended.
- Get Regular About Light Exposure: Exposure to natural light, particularly in the morning and late afternoon, is crucial for regulating the body’s internal clock, promoting alertness during the day, and facilitating restful sleep at night. Studies show that morning sunlight exposure improves sleep quality, reduces sleep onset time, and decreases night awakenings. Sunlight also has known benefits for mood and concentration.
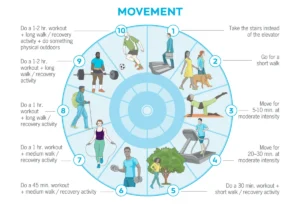
- Go Easier at the Gym: While exercise is vital, intense, prolonged workouts can exacerbate fatigue and increase injury risk in midlife. Instead, embrace shorter, moderate sessions. Short bursts of activity (e.g., a 5-10 minute walk, a quick set of push-ups) can boost daytime alertness. Gentle exercises like yoga or stretching can aid relaxation before bed, provided they aren’t overly intense, which could trigger adrenaline release. Listen to your body, especially after poor sleep, and adjust workout intensity or volume (e.g., opt for Zone 2 cardio instead of high-intensity, or reduce sets/reps in resistance training) to prioritize recovery.
- Investigate Cognitive Behavior Therapy for Insomnia (CBT-I): This evidence-based therapy equips individuals with skills and cognitive reframing techniques to improve sleep. CBT-I principles, such as maintaining a consistent wake-up time regardless of prior night’s sleep, can be transformative for chronic sleep issues.
- Get Real About Stress: Menopause often coincides with peak career responsibilities, caring for aging parents, and other life stressors. Critically evaluate current responsibilities to identify areas for reduction or downsizing. Track time and bandwidth usage for several days, then analyze where energy is being drained. Ask: "Is this activity essential?" "Can I delegate or eliminate this?" "Am I saying yes to too many demands?" Tools like the "Wheel of Stress Assessment" can help identify specific stress dimensions. Learning to say "no" more often and without regret is a powerful act of self-care.
- Experiment with Cooling Technology: A cooler sleep environment can significantly reduce night sweats and improve sleep quality. Strategies include lowering the thermostat, using fans, or investing in specialized cooling mattress pads.
- Take Frequent Breaks: When brain fog descends, productivity inevitably wanes. Rather than pushing through, permit yourself short, restorative breaks—20 minutes of complete disengagement, such as resting with eyes closed, engaging in light stretching, or simply observing surroundings. A 5-minute mind-body scan (focusing on physical sensations from head to toe without judgment) can also offer a quick mental refresh and insight into current physical and emotional states.
- Follow a Diet Promoting Healthy Circulation: Nutrition plays a crucial role in supporting brain and vascular health. Diets rich in vegetables, fruits, whole grains, healthy fats (olives, fish), and legumes, such as the MIND and Mediterranean diets, are associated with a reduced risk of Alzheimer’s disease and depression. Furthermore, nitrate-rich foods like beets and dark, leafy greens can temporarily improve memory by dilating blood vessels and increasing blood flow to the brain.
The Transformative Potential of Menopause
While the challenges of menopause, particularly cognitive and emotional distress, can be profoundly frustrating, this life stage presents a unique and often hidden opportunity for profound self-re-evaluation. The individual’s experience of diminished cognitive capacity forced an existential question: "Do I really need to be doing this?" This question, extending beyond career to all aspects of life, allowed for a reassessment of how limited mental resources should be allocated. It led to insights about simplifying daily tasks, reducing self-imposed obligations, and consciously choosing to say "no" more often to create space for what truly mattered: family, friendships, and personal well-being.
With appropriate medical support and intentional lifestyle adjustments, energy and mental clarity can return. More importantly, the journey through menopause can forge a deeper understanding of personal limits and priorities, leading to a more intentional, balanced, and fulfilling life post-menopause. The initial period of struggle, though challenging, can ultimately lead to a powerful redefinition of self and purpose, allowing women to emerge from this transition with renewed vigor and clarity, choosing to live life on their own terms.
References
Click here to view the information sources referenced in this article.