The Immediate Impact: How Pro-Inflammatory Meals Trigger Rapid Cellular Responses and Health Risks
Inflammatory markers in the human body can double within a mere six hours following the consumption of a pro-inflammatory meal, a rapid cellular response that underscores the immediate and profound impact of dietary choices on physiological health. This swift escalation in systemic inflammation, traditionally associated with chronic dietary patterns, is now increasingly recognized as an acute phenomenon with significant long-term implications for public health.
The Acute Inflammatory Cascade: A Rapid Response
The body’s inflammatory response is a complex biological process designed to protect against harmful stimuli such as pathogens, damaged cells, or irritants. However, when this system is overactive or persistently triggered, it can contribute to a range of chronic diseases. For years, scientific discourse primarily focused on the cumulative effects of a consistently unhealthy diet leading to chronic low-grade inflammation. Recent research, however, highlights that the "stimuli that jumpstart the destructive inflammatory cascade" are not limited to chronic intake but can be "evident after the consumption of a single meal."
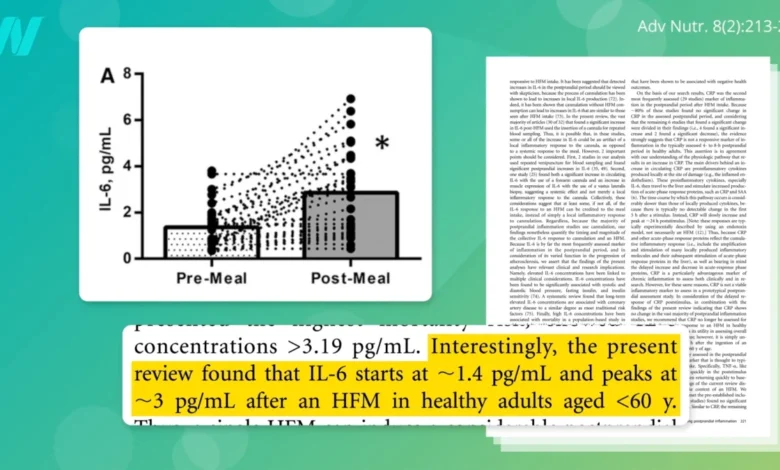
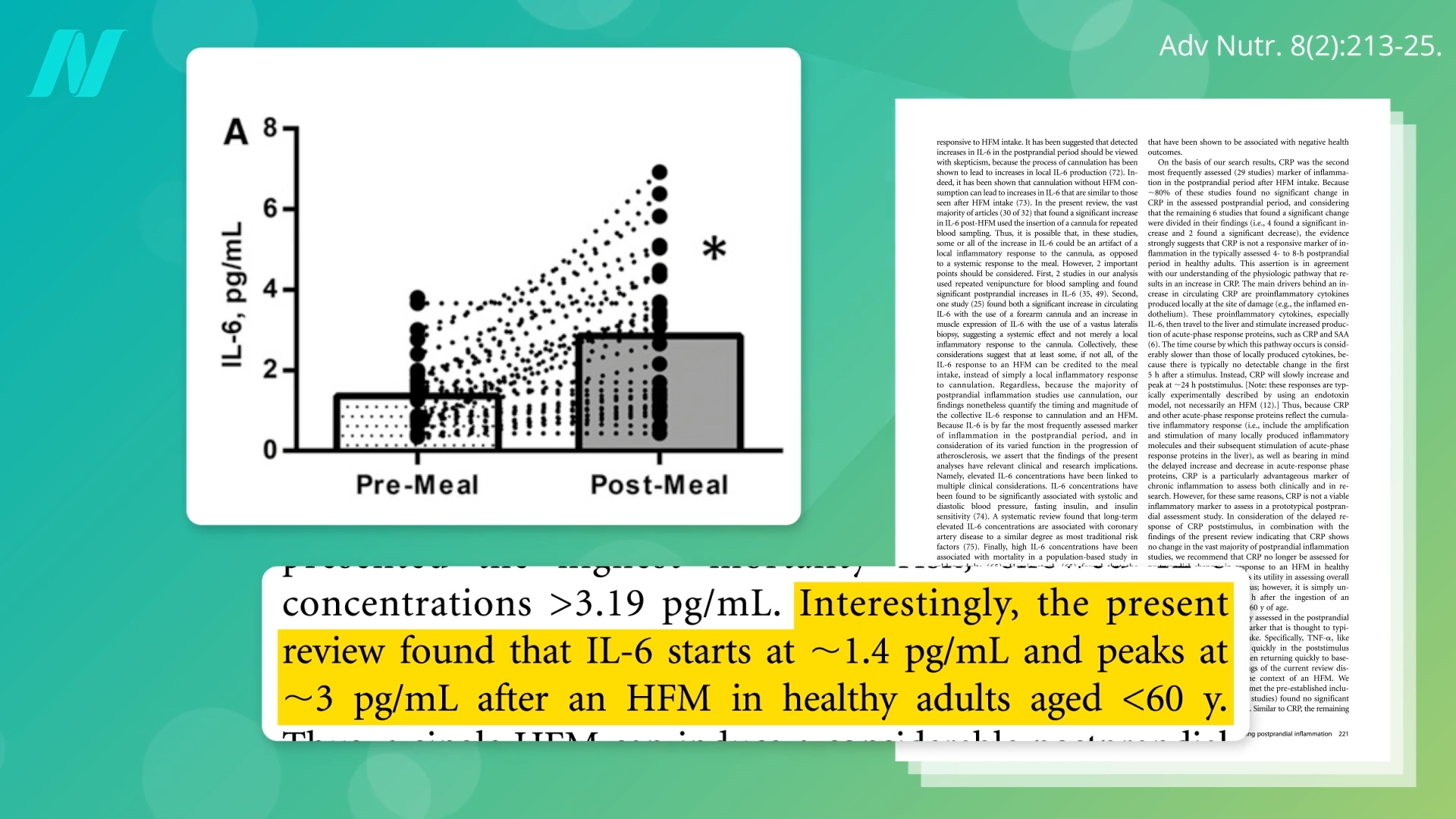
Within hours of ingesting certain foods, key inflammatory markers begin to rise dramatically. Interleukin-6 (IL-6), a cytokine that plays a crucial role in immune response and inflammation, is a prime example. Studies have consistently shown that IL-6 levels can skyrocket, often doubling within six hours, following a meal high in pro-inflammatory components. This rapid increase is not an isolated incident; it signifies a systemic activation of the immune system in response to the absorbed nutrients. Beyond IL-6, other critical markers like C-reactive protein (CRP), an acute-phase protein synthesized by the liver, and Tumor Necrosis Factor-alpha (TNF-α), another potent cytokine, also show significant elevation post-prandially. The quick onset of this inflammatory surge serves as a stark reminder of the body’s intricate and immediate connection to its nutritional environment.
Unmasking the Culprits: Foods That Fuel Inflammation
Extensive research has begun to pinpoint the specific dietary components responsible for this rapid inflammatory response. The culprits typically fall into two main categories: certain types of fats and refined carbohydrates/added sugars.

The Dual Threat: Fats and Sugars
High-fat meals, commonly comprising sources like meat, eggs, dairy, and various oils, have long been implicated in inflammation. The majority of studies investigating post-prandial inflammation have observed a significant increase in IL-6 levels after participants consumed high-fat meals. However, it’s crucial to note that these experimental meals often contained a blend of pro-inflammatory ingredients, including "junky refined carbohydrates like white flour and added sugar," making it challenging to isolate the exact drivers.
To dissect this further, researchers have conducted studies where participants were given isolated macronutrients. For instance, when individuals were provided with "essentially straight butter fat and no carbs," they still experienced a notable spike in inflammation within hours. This direct evidence confirms that added fats, irrespective of carbohydrate content, possess inherent pro-inflammatory properties. Simultaneously, similar experiments involving "straight sugar water without any fat" yielded identical results: a significant inflammatory response. This demonstrates unequivocally that added sugars are also independently pro-inflammatory, initiating a cellular cascade that contributes to systemic inflammation. These findings challenge the simplistic notion of ‘fat being bad’ or ‘sugar being bad’ in isolation, instead highlighting their synergistic or independent capacity to ignite inflammatory pathways.
The Unexpected Culprit: Lean Meats
A particularly revealing aspect of recent research challenges a long-held dietary assumption: that lean meats are universally healthier choices for managing inflammation. While high-fat meats are clearly pro-inflammatory, evidence suggests that even very lean animal protein can elicit a strong inflammatory response.
Reviews sometimes claim a drop in inflammatory markers after eating wild game, often touted for its leanness. However, these comparisons are often made against conventional, fattier store-bought meats. When compared to a non-meat diet, even extremely low-fat meats still demonstrate pro-inflammatory effects. For example, studies have shown that consuming a kangaroo steak, which is exceptionally low in fat—comparable to elk or moose—still triggers a "strong inflammatory response within hours of eating it." This indicates that the inflammatory potential of animal products may extend beyond just their fat content. Potential mechanisms include components like endotoxins (lipopolysaccharides or LPS) from animal guts that can translocate into the bloodstream, advanced glycation end products (AGEs) formed during cooking, or even specific amino acid profiles and heme iron found in meat, which can act as pro-oxidants and inflammatory triggers. While "certainly less inflammatory than conventional meat you might get at the store," the fact remains that even lean animal proteins are "pro-inflammatory nonetheless, increasing markers of inflammation within mere hours."
The Long-Term Repercussions of Acute Inflammation
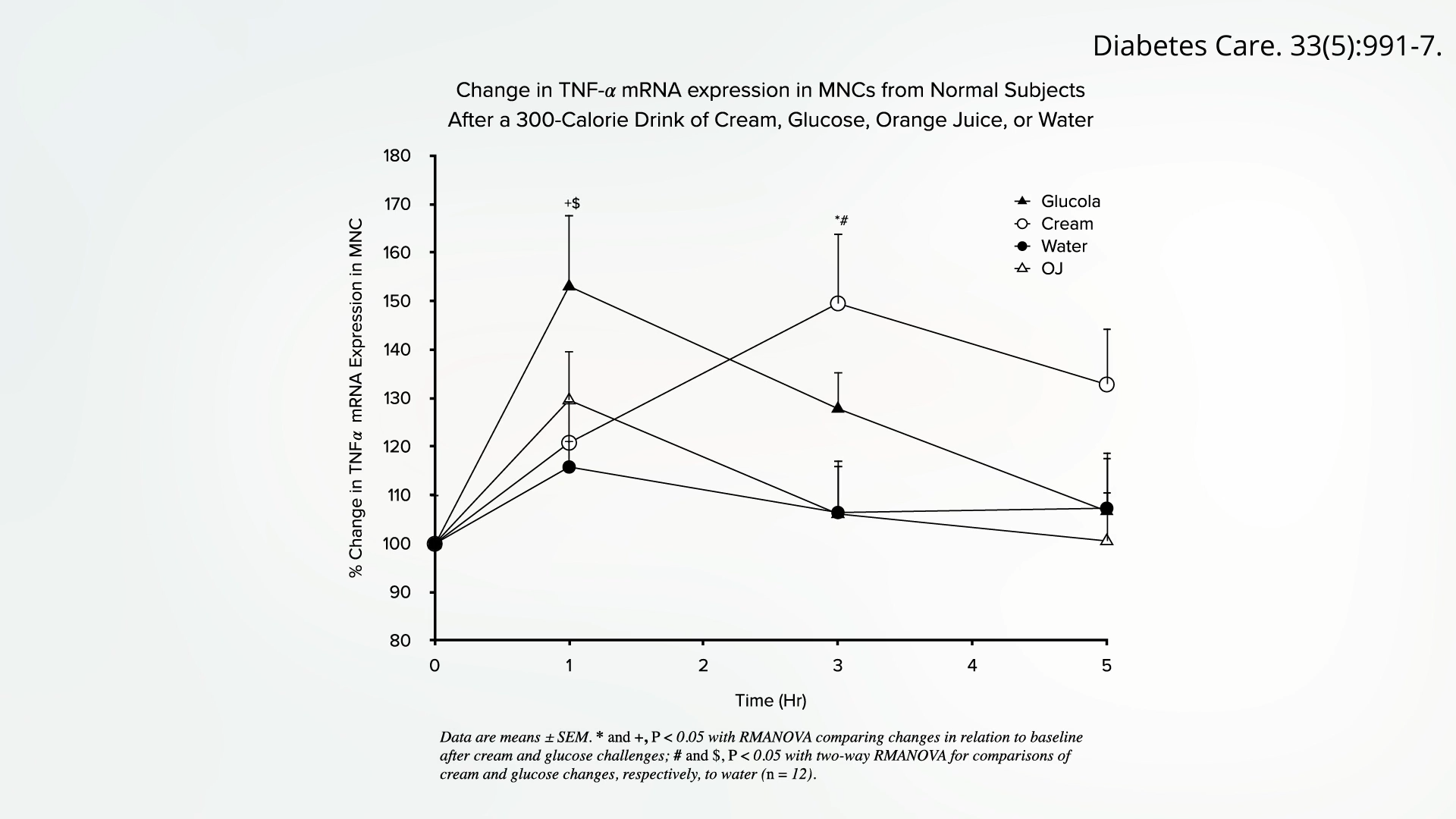
The rapid, post-meal inflammatory spikes are not isolated events without consequence. On the contrary, these acute responses contribute significantly to the development and progression of "persistent low-grade inflammation," which is recognized as an "underlying factor in several high-mortality chronic diseases." The cumulative effect of repeated inflammatory surges after each meal can overwhelm the body’s anti-inflammatory mechanisms, leading to a chronic state of heightened immune activity.
Disease Links and the Danger Threshold
The link between inflammation and chronic diseases is well-established:
- Type 2 Diabetes: Chronic inflammation contributes to insulin resistance, where cells become less responsive to insulin, leading to elevated blood sugar levels. It can also impair the function of pancreatic beta-cells, which produce insulin.
- Obesity: Adipose tissue, particularly visceral fat, is not merely a storage depot but an active endocrine organ that secretes pro-inflammatory cytokines, creating a vicious cycle where obesity fuels inflammation, and inflammation exacerbates obesity.
- Heart Disease: Inflammation plays a critical role in all stages of atherosclerosis, the hardening and narrowing of arteries. It contributes to endothelial dysfunction (damage to the lining of blood vessels), plaque formation, and plaque instability, increasing the risk of heart attacks and strokes. Indeed, inflammation is "linked with increased risk of heart disease, the number one killer of men and women, even as strongly as some other major well-known risk factors like high cholesterol."
The quantification of this risk is striking. When IL-6 levels consistently reach approximately 3 pg/mL—a level observed to jump after unhealthy meals—it is "associated with twice the risk of death." This increased mortality risk has been confirmed across multiple studies, highlighting the profound impact of even moderately elevated inflammatory markers. This threshold for concern underscores the importance of dietary interventions that can keep these markers in check.
Counteracting the Fire: The Role of Anti-Inflammatory Foods
While certain foods ignite inflammation, others possess powerful anti-inflammatory properties, offering a pathway to mitigate risks and promote health. The good news is that "not all high-fat foods cause inflammation."
Whole Plant Foods as Allies
The distinction lies largely in the source and context of nutrients. "Whole plant foods" stand out as potent anti-inflammatory agents. For instance, more than a dozen studies have consistently shown that "nuts do not increase inflammatory markers, even when eating up to handfuls of nuts a day." This is attributed to their rich profile of healthy fats (monounsaturated and polyunsaturated), fiber, antioxidants, and phytochemicals that actively combat oxidative stress and inflammation.
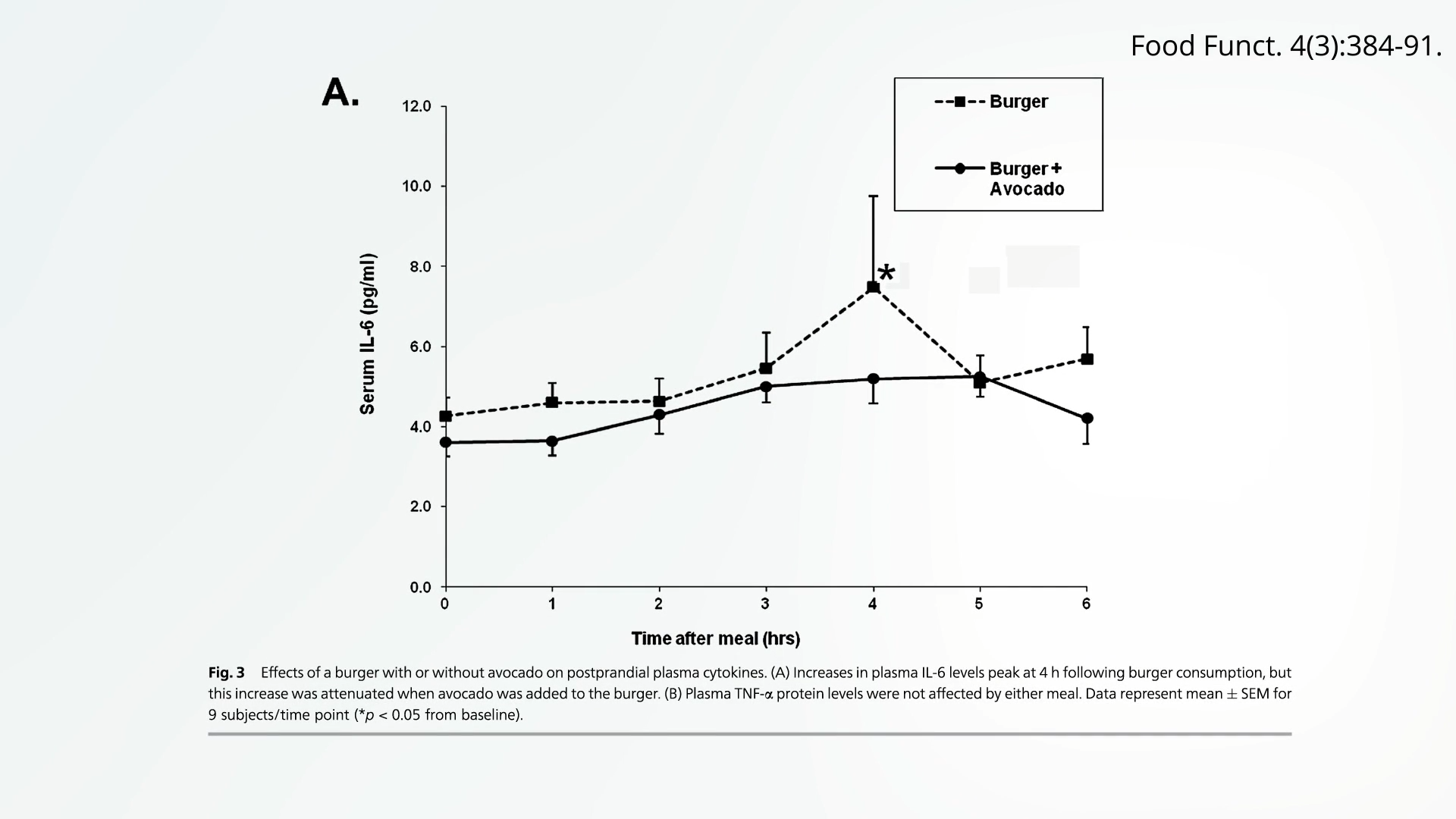
Furthermore, specific plant foods can even "blunt some of the inflammation" caused by pro-inflammatory components. A compelling example is the avocado: "spread half an avocado on a beef burger, and you may be able to blunt some of the inflammation caused by the meat—even lean meat." Avocados are rich in monounsaturated fatty acids, carotenoids, and other bioactive compounds that have been shown to have anti-inflammatory and antioxidant effects, helping to counteract the detrimental impact of other meal components.
This principle extends to a broader range of whole plant foods, including fruits, vegetables, legumes, and whole grains. These foods are abundant in fiber, which supports a healthy gut microbiome (a key regulator of systemic inflammation), and a vast array of antioxidants and phytochemicals that neutralize free radicals and modulate inflammatory pathways. Adopting a diet rich in these components, often exemplified by Mediterranean or largely plant-based dietary patterns, can actively attenuate inflammation.
Expert Perspectives and Public Health Implications
The growing body of evidence on post-prandial inflammation has significant implications for both scientific understanding and public health policy. Researchers increasingly emphasize that the immediate physiological response to a meal cannot be overlooked. This shift in perspective necessitates a more nuanced approach to dietary recommendations, moving beyond general advice to consider the acute impact of specific food combinations and macronutrient ratios.
Leading nutritionists and public health organizations are beginning to integrate these findings into their guidance, stressing the importance of not just long-term dietary patterns but also daily meal choices. The message is clear: every meal presents an opportunity to either fuel or quell inflammation. This empowers individuals with a more immediate sense of control over their health, highlighting that conscious food choices can lead to rapid and measurable improvements in inflammatory status. This understanding also challenges the marketing of certain "lean" or "healthy" animal products if they still trigger inflammatory responses.
The broader impact includes a re-evaluation of nutritional education, emphasizing the cellular mechanisms behind food choices. It also underscores the importance of a holistic approach to health, where diet is seen as a primary tool for disease prevention and management, working in concert with lifestyle factors like exercise and stress reduction.
Future Directions in Nutritional Science
The ongoing research into diet and inflammation continues to evolve. Future directions are likely to include more personalized nutrition approaches, leveraging genetic and gut microbiome data to predict individual inflammatory responses to specific foods. Deeper investigations into the precise molecular pathways by which different nutrients interact with the immune system will further refine dietary guidelines. The development of advanced biomarkers and diagnostic tools will also allow for more accurate monitoring of individual inflammatory states, enabling targeted dietary interventions.
Conclusion: A Call for Mindful Eating
The revelation that inflammatory markers can double within hours of eating certain meals is a powerful call to action. It transforms the abstract concept of "healthy eating" into a tangible, immediate physiological event. The evidence is compelling: common dietary staples, particularly those high in refined fats, added sugars, and even some lean animal proteins, can rapidly trigger an inflammatory cascade. Conversely, whole plant foods like nuts and avocados demonstrate a remarkable capacity to either prevent or mitigate this response.
Understanding the immediate impact of food choices empowers individuals to take proactive steps in managing their health. By opting for nutrient-dense, whole plant foods, and minimizing the consumption of known pro-inflammatory agents, individuals can significantly reduce their systemic inflammatory load, thereby lowering their risk for a spectrum of chronic diseases, from heart disease to type 2 diabetes. This knowledge solidifies the principle that every meal is an opportunity to nourish and protect the body, making mindful eating not just a dietary trend, but a fundamental pillar of long-term health and well-being.