Many people with IBS would trade 10 to 15 years of life expectancy for an instant cure for their condition.
This stark revelation comes from a comprehensive study involving nearly 2,000 individuals diagnosed with irritable bowel syndrome (IBS), underscoring the profound and often debilitating impact this chronic condition has on daily life. Further research corroborates this desperation, with IBS sufferers expressing willingness to take a medication carrying a one percent risk of sudden death if it promised an immediate and lasting cure for their symptoms. These symptoms – including unpredictable and urgent bouts of diarrhea, persistent constipation, excessive gas, and severe abdominal pain – are not merely discomforts; they are life-altering experiences that drive individuals to contemplate extreme trade-offs for relief.
The Invisible Burden: A Glimpse into Life with IBS
For many, IBS manifests as episodes of abdominal pain described as more excruciating than childbirth. These intense flare-ups have a cascading effect, siphoning concentration, disrupting sleep patterns, and severely compromising work productivity. The pervasive nature of these symptoms often forces individuals to meticulously plan their lives around the availability of private, clean restrooms. This constant fear of a sudden, uncontrollable flare-up leads to significant social withdrawal, with many avoiding public spaces like restaurants, social gatherings, and even exercise facilities.
This omnipresent apprehension has been formally recognized as gastrointestinal-specific anxiety. It’s a profound psychological burden that infiltrates every aspect of an individual’s existence, from the quality of their social relationships to their overall sense of well-being. This specialized anxiety is a primary driver behind the reported poorer quality of life among people with IBS compared to those managing other serious chronic conditions, including heart disease, diabetes, and even end-stage kidney disease. The silent suffering and social isolation inherent in IBS often go unrecognized, making these study findings a crucial call for increased awareness and support.
Navigating the Path to Management: Expert Insights
Despite the severity, there are tangible strategies for managing IBS. PN Super Coach Sarah Maughan, who holds certification from Monash University – a global leader in the study of food sensitivities and IBS – has observed firsthand how targeted lifestyle modifications can significantly mitigate flare-ups, calm GI anxiety, and empower individuals to reclaim their lives. "My hope is for everyone with IBS to know they have options, whether that’s turning to a physician for medication and/or a health coach to learn about lifestyle changes and how to put them into action," says Maughan. Her perspective highlights the critical importance of a multi-pronged approach to IBS care.
This article delves deeper into the nature of IBS, exploring its definition, symptoms, and underlying causes. It also outlines the diagnostic process, including the various types of IBS and how to prepare for a medical appointment. Crucially, it provides five evidence-based strategies for supporting bowel health and function. For health coaches, the article also offers clear guidelines on how to effectively support clients with IBS while strictly adhering to professional scope of practice.
IBS: Unpacking the World’s Most Common Digestive Disorder
Often colloquially referred to as "spastic colon," Irritable Bowel Syndrome holds the unfortunate distinction of being the most commonly diagnosed digestive disorder globally, affecting approximately 14 percent of the adult population. This prevalence translates to hundreds of millions of individuals worldwide grappling with its symptoms, creating a significant public health challenge and economic burden due to healthcare costs and lost productivity.
A key differentiator setting IBS apart from conditions like Crohn’s disease and other inflammatory bowel diseases (IBD) is its fundamental nature: IBS does not alter the structural architecture of the gut. When medical professionals employ diagnostic imaging techniques, they find no evidence of infections, inflammation, physical damage to the bowel wall, or other visible pathological signs of disease. This lack of observable physical markers historically led many healthcare providers to erroneously conclude that IBS was purely psychological, a "diagnosis of exclusion" that often left patients feeling dismissed and misunderstood.
However, scientific understanding has evolved dramatically. Today, experts unanimously view IBS as a functional neuro-gastrointestinal disorder. This modern perspective acknowledges that while there may be no visible structural damage, the communication pathways between the gastrointestinal tract and the brain are not functioning optimally. This dysregulation results in the brain transmitting unnecessary pain signals and interfering with the typical, rhythmic contractions and relaxations essential for healthy bowel function. This paradigm shift has been instrumental in validating the experiences of IBS patients and guiding more effective research and treatment approaches.
A Spectrum of Suffering: Understanding IBS Symptoms
The elusive nature of IBS is further complicated by the variability of its symptoms. They can wax and wane, with some individuals experiencing months or even years of relative relief, only to be struck by a severe flare-up that can persist for hours or even weeks. Moreover, IBS is not a monolithic condition; not everyone experiences the same constellation of symptoms, which significantly complicates diagnosis.

The primary symptoms typically include:
- Abdominal pain and cramping: Often relieved by a bowel movement.
- Stool irregularities: This can manifest as chronic constipation (IBS-C), frequent diarrhea (IBS-D), or an alternating pattern of both (IBS-M).
- Excessive gas and bloating: A common and often intensely uncomfortable symptom.
- Mucus in stools: Can be a sign of irritation.
- Incomplete bowel movements: A sensation that the bowels have not been fully emptied, leading to repeated attempts.
These symptoms collectively contribute to the profound impact on quality of life, ranging from physical discomfort to significant psychological distress and social limitations.
Peering Beneath the Surface: What Causes IBS?
Despite significant research, the precise mechanisms explaining why the gut functions differently in people with IBS are still being fully elucidated. However, several compelling theories have emerged, offering valuable insights into potential therapeutic targets.
One leading hypothesis centers on the idea that the nerve endings within the gastrointestinal tract of individuals with IBS may be inherently overly sensitive. This heightened sensitivity can lead to two distinct sets of symptoms:
- Hypersensitive nerves communicate exaggerated pain signals to the brain. This means that people with IBS become acutely aware of normal digestive processes that would typically go unnoticed by someone without the disorder. For instance, tiny gas bubbles, a routine byproduct of digestion, can trigger intense discomfort or even severe pain in an IBS patient, whereas they would be completely imperceptible to others.
- Overreactive nerves can trigger GI muscles to contract with excessive force. This hyperactivity can accelerate the passage of food through the intestines, leading to symptoms like gas, bloating, and diarrhea. Conversely, if these same nerves underreact, the GI muscles may not contract forcefully enough, slowing the transit of food and resulting in constipation. This dual possibility explains the diverse bowel habits seen across different IBS types.
Another significant theory points to disturbances in the gut microbiome – the vast ecosystem of bacteria, fungi, and other microorganisms residing in the digestive tract. This theory helps explain why a subset of individuals develops IBS symptoms after experiencing a severe gastrointestinal illness, such as Norovirus or bacterial gastroenteritis, a phenomenon known as post-infectious IBS. An imbalance or dysbiosis in the gut microbiome can affect digestion, nutrient absorption, and even influence gut-brain communication, contributing to IBS symptoms. Research continues to explore the intricate interplay between diet, environment, and microbial composition in the pathogenesis of IBS.
The Diagnostic Journey: Confirming IBS and Ruling Out Other Conditions
If you or a client suspects IBS, the paramount first step is to consult a credentialed health professional. This is critical because IBS symptoms overlap significantly with several other gastrointestinal diseases and health conditions that necessitate specific medical interventions, which could range from medication and surgery to medically supervised lifestyle changes. These conditions include infections, inflammatory bowel diseases (like Crohn’s and ulcerative colitis), celiac disease, certain cancers, and various food allergies. A thorough medical evaluation is essential to rule out these potentially more serious conditions.
It is particularly important to seek immediate medical attention if any of the following "red flag" symptoms are present, as they could indicate a condition other than IBS:
- Unexplained weight loss
- Rectal bleeding
- Anemia
- Fever
- New onset of symptoms after age 50
- Family history of colon cancer, IBD, or celiac disease
Beyond ruling out other GI conditions, a healthcare professional will conduct a detailed interview, asking specific questions about the nature, frequency, and severity of symptoms. This comprehensive assessment allows them to pinpoint the specific IBS "type" a patient might have, which is crucial for guiding personalized treatment strategies:
- IBS with Diarrhea (IBS-D): Characterized by frequent loose stools, urgency, and abdominal pain.
- IBS with Constipation (IBS-C): Defined by hard, lumpy stools, infrequent bowel movements, and straining.
- IBS with Mixed Bowel Habits (IBS-M): Involves alternating periods of both diarrhea and constipation.
- IBS Unclassified (IBS-U): Used when symptoms don’t clearly fit into the other categories.
The identified IBS type directly informs the healthcare professional’s recommendations. For IBS-D, a provider might suggest a short course of antibiotics to address bacterial overgrowth, along with anti-diarrheal medications. In contrast, for IBS-C, recommendations could include fiber supplements, non-habit-forming laxatives, or specific laxative-like medications designed to reduce pain perception and regulate bowel movements. This tailored approach underscores the complexity of IBS management.
Optimizing Your Medical Appointment: A Pre-Visit Checklist
To maximize the effectiveness of a medical consultation, preparing beforehand is highly recommended. For yourself or a client, considering responses to common questions can streamline the diagnostic process:
- When did your symptoms begin?
- How often do you experience symptoms?
- What makes your symptoms better or worse?
- Have you noticed any specific food triggers?
- What medications or supplements are you currently taking?
- What is your family history of digestive conditions?
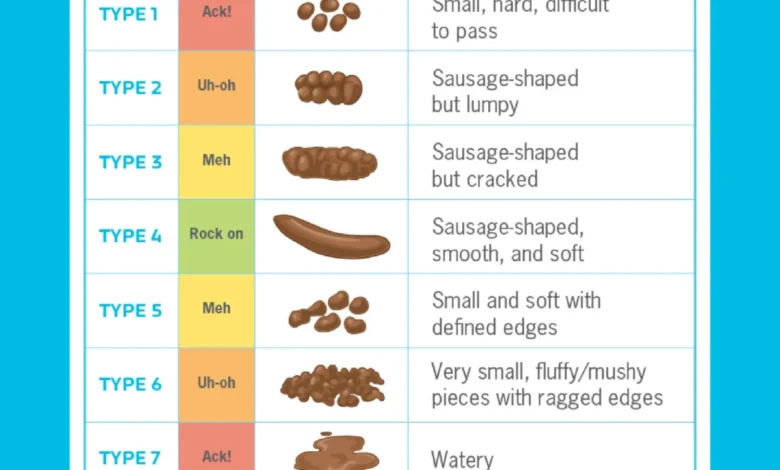
A perhaps less appealing but highly beneficial preparation step involves keeping a "poo diary" for a couple of weeks prior to the appointment. In this diary, meticulously track the frequency of bowel movements and other associated symptoms. Crucially, utilize the Bristol Stool Chart to objectively note the quality and consistency of stools. This detailed, objective information can provide invaluable insights to your healthcare professional, aiding them in accurately assessing whether IBS is present and, if so, which specific type. Observing stool characteristics can reveal critical clues about gut health, further empowering both patient and physician in the diagnostic journey.

Five Evidence-Based Strategies for IBS Relief and Gut Health
Recent years have seen significant advancements in IBS treatment, including the approval of several new prescription medicines by regulatory bodies like the U.S. Food and Drug Administration, as well as medical devices designed to stimulate cranial nerves. Concurrently, thousands of research papers have illuminated the intricate relationship between IBS and various lifestyle habits, yielding promising findings for non-pharmacological interventions. Here are five evidence-based strategies that can significantly reduce IBS symptoms and concurrently enhance overall health.
1. Integrate Regular Exercise
Consistent physical activity is a powerful ally against IBS. Individuals with IBS who engage in regular exercise typically report fewer symptoms and less frequent flare-ups compared to their sedentary counterparts. A study that involved IBS patients walking moderately for an hour three times a week demonstrated significant relief from bloating and abdominal pain within a mere 12 weeks. While the exact mechanisms are still being fully explored, exercise is believed to mitigate IBS symptoms through several pathways. It can reduce stress and improve mental health, which in turn positively influences the gut-brain axis. Furthermore, physical activity may promote the growth of beneficial gut bacteria, aiding in more efficient food breakdown and reducing inflammation, all contributing to a calmer digestive system.
2. Prioritize Stress Management
The profound connection between the mind and gut means that anxiety, stress, and depression can significantly exacerbate IBS symptoms. These psychological states activate stress hormones such as norepinephrine (noradrenaline) and cortisol, which can:
- Intensify pain signals in the gut.
- Alter gut motility, leading to either faster or slower transit.
- Increase gut permeability, potentially allowing inflammatory substances to enter the bloodstream.
However, stress is not something that can simply be switched off. Telling oneself to "stop being so stressed" is rarely effective and often counterproductive. This is where the guidance of certified coaches like Sarah Maughan becomes invaluable. They help clients focus on what is within their sphere of control – such as practicing self-compassion, incorporating nervous system regulators like yoga or meditation, or engaging in gentle walking. By shifting focus from uncontrollable external stressors to internal responses and coping mechanisms, clients often report feeling calmer, more capable, and experience a reduction in their IBS symptoms.
3. Embrace a Slower Eating Pace
The seemingly simple act of slowing down while eating can yield substantial benefits for IBS sufferers. Precision Nutrition coaches have long championed relaxed, deliberate eating, not just for calorie management but also for its profound impact on gastrointestinal health. Slower eating directly correlates with more thorough chewing, which mechanically breaks down food into smaller particles. This, coupled with increased exposure to digestive enzymes in the mouth, initiates pre-digestion, reducing the workload on the stomach and intestines. Moreover, eating in a calm, unhurried environment helps lower stress hormone levels, making it less likely that they will amplify GI pain signals. This strategy is particularly pertinent for busy individuals, such as young parents, who often find themselves rushing meals.
4. Troubleshoot Sleep Problems
Sleep quality is intrinsically linked to IBS symptom severity. Research indicates that individuals with IBS frequently experience more shallow, less restorative, and highly interrupted sleep. Paradoxically, many IBS patients may sleep more hours overall than those without the condition, yet still feel profoundly unrested. This fatigue creates a vicious cycle: poor sleep elevates stress hormone levels, which, in turn, can exacerbate gut pain. Additionally, unrested individuals often experience increased hunger and intensified cravings for fats and sweets – precisely the types of foods more likely to trigger IBS symptoms, and which are often consumed too quickly, further compounding digestive distress. Breaking this cycle is challenging but crucial. The previously mentioned strategies – exercise, stress management, and slower eating – all contribute positively to improving sleep quality. Practical tips such as eating a smaller dinner earlier in the evening or adopting a relaxing pre-bedtime routine (e.g., foam rolling, guided meditation, a warm bath, or journaling) can also be highly effective.
5. Systematically Investigate Your Diet
While there is no universal "IBS diet," experts have identified several food categories that are frequently problematic for a significant number of individuals. These include:
- Fermentable Oligosaccharides, Disaccharides, Monosaccharides, and Polyols (FODMAPs): This family of carbohydrate-rich foods is poorly absorbed in the small intestine. Even in healthy individuals, FODMAPs can slow digestion and draw water into the gut. When fermented by gut bacteria, they produce gas, which can stretch the intestinal wall. For most, this process is unnoticed; for those with IBS, it can lead to intense pain, bloating, and altered bowel habits. High-FODMAP foods encompass wheat, rye, barley, onions, garlic, beans, certain dairy products, honey, cashews, some processed meats, and numerous fruits and vegetables.
- Caffeinated beverages and foods: Especially coffee, which can trigger the release of stress hormones, stimulate stomach acid production, increase muscle contractions in the colon, and irritate the intestinal lining.
- Alcohol and spicy foods: Both are known irritants to the delicate lining of the gut, potentially provoking symptoms.
- High fructose corn syrup and sugar alcohols (e.g., sorbitol, mannitol): These sweeteners have been consistently linked to gas, bloating, and diarrhea in susceptible individuals.
- Fatty, greasy foods: High-fat meals can significantly slow digestion and attract water into the bowel, often leading to loose stools, bloating, and gas.
It is crucial to understand that not everyone with IBS is sensitive to the same foods or beverages. "Everyone can have different triggers," emphasizes Maughan. "That’s why it’s so important to figure out what makes your body feel good and what doesn’t." One individual might react to apples but tolerate berries, while another can drink green tea but not black. Gluten-free diets may offer relief for some but prove ineffective for others. Similarly, while many find relief by avoiding high-FODMAP foods, sensitivities are often specific; eliminating all FODMAPs might be unnecessarily restrictive if only a few types are problematic. For this reason, an elimination diet, under appropriate guidance, is often the most effective way to identify individual food and beverage triggers and determine tolerable quantities.
Coaching Clients with IBS: Navigating the Scope of Practice
A common question among health coaches in online communities is: "My client just told me she has IBS. Am I allowed to continue coaching this person?" The unequivocal answer is yes, absolutely. As Sarah Maughan, who specializes in digestive problems, affirms, coaching someone with IBS is fundamentally similar to coaching a client with any other nutritional goal.
"Because IBS is often largely associated with what someone eats, it’s within a coach’s wheelhouse—with some caveats," Maughan explains. "You can’t diagnose your client with the condition, and you should make it clear that you’re not prescribing a diet for them. In addition, you should encourage clients to seek care from a medical professional, especially if you suspect something other than IBS is going on."
To ensure coaches remain strictly within their professional scope of practice, here are key distinctions:
DO:

- Encourage clients experiencing digestive issues to consult a healthcare professional to obtain a definitive diagnosis.
- Share general information about potential lifestyle modifications, including the principles of elimination diets.
- Help clients design and run personalized "experiments" to gain insight into the connection between their lifestyle, diet, and bodily responses.
- Offer to collaborate with a client’s medical team, assisting the client in adopting and maintaining consistency with the lifestyle changes recommended by their healthcare providers.
- Support clients with optional recipes and tools that facilitate the practical application of their learned insights.
- Encourage clients to explore a multi-disciplinary approach to IBS management, empowering them to discover the unique combination of strategies that works best for them.
- Ensure clients understand that they retain autonomy to choose whether or not to implement any given lifestyle change.
DON’T:
- Diagnose clients by stating, "It sounds like you might have IBS."
- Promote a rigid and overly restrictive diet as a definitive "cure" for all digestive problems.
- Contradict medical professionals or suggest that the medical establishment is consistently incorrect about IBS.
- Create a prescriptive, anti-IBS meal plan for a client to follow.
- Claim to possess all the answers or suggest that clients do not require medical advice or therapies.
- Use manipulative tactics, force, or fear to coerce clients into following specific advice.
Adhering to these guidelines ensures ethical and effective support for clients with IBS.
Elimination Diets for IBS: A Scientific Approach to Personalized Nutrition
Elimination diets serve as systematic "science experiments" designed to identify specific food triggers. They involve a temporary exclusion of certain foods, typically for about three weeks, followed by a slow and careful reintroduction of individual foods to monitor for symptom reactions. While the term "elimination diet" might evoke images of bland, restrictive eating, there are various types, some far less stringent than others.
1. Elimination Diet "Lite" for IBS: This approach is ideal for individuals who already have a strong suspicion about which specific foods or beverages trigger their symptoms. The process involves eliminating up to four suspected trigger foods for several weeks. After this period, each food is slowly reintroduced one at a time, allowing the individual to observe any return of symptoms. For example, if dairy is a suspected culprit, it would be eliminated for three weeks and then reintroduced to assess its impact.
2. Elimination Diet "Medium" (Precision Nutrition Approach): For those uncertain about their food sensitivities but not yet ready for an extremely restrictive plan, the Precision Nutrition elimination diet offers a balanced pathway. Developed and approved by registered dietitians, this plan systematically removes many common problematic foods while ensuring a diverse intake of vegetables, fruits, starches, legumes, nuts, seeds, and meats. This design allows individuals to maintain a well-balanced diet throughout the elimination phase. Resources like the "Ultimate Guide to Elimination Diets" provide comprehensive guidance, including at-a-glance charts, recipes, meal ideas, and tip sheets.
3. The FODMAP Diet for IBS: Over several years, researchers at Monash University in Australia have rigorously developed and studied a low-FODMAP elimination diet specifically for individuals with IBS. Unlike other elimination diets, the FODMAP diet is a highly specialized form of medical nutrition therapy. Its list of problematic foods is not intuitive, and the reintroduction phase is considerably more complex than other elimination protocols. Consequently, if IBS has been diagnosed and a FODMAP issue is suspected, it is strongly recommended to seek the expertise of a FODMAP-certified practitioner. Monash University also offers a dedicated FODMAP Diet app, which serves as an invaluable tool for navigating low-FODMAP eating. High-FODMAP foods include specific vegetables (artichoke, asparagus, mushrooms, onions, garlic), fruits (apples, cherries, mango, watermelon), dairy (cow’s milk), legumes, and grains (wheat, rye, barley), while low-FODMAP alternatives like green beans, carrots, kiwi, oranges, almond milk, and oats are generally well-tolerated.
The Transformative Power of Health Coaching
While knowledge is foundational, it alone does not always translate into actionable change. There’s a significant difference between intellectually knowing that dairy aggravates your gut and consistently acting on that knowledge. Similarly, an individual might know they feel better with an early, small dinner but struggle to integrate this into a consistent lifestyle. This is precisely where the role of a certified health coach becomes invaluable.
"Many of my clients already have an idea of the foods that tend to cause them problems," says Maughan, "But they’re nervous to know for sure because they fear that the knowledge will make eating more challenging." Maughan’s approach reassures clients that even if an elimination diet identifies a favorite food as a trigger, they are not obligated to permanently eliminate it. The power lies in choice: clients can choose to continue enjoying certain foods, while also having the option to avoid them when it is critical to prevent IBS symptoms. "With knowledge, you have choices," Maughan concludes, encapsulating the empowering philosophy of informed self-management.
References
Click here to view the information sources referenced in this article.
If you’re a coach, or you want to be…
You can help people build sustainable nutrition and lifestyle habits that will significantly improve their physical and mental health—while you make a great living doing what you love. We’ll show you how. If you’d like to learn more, consider the PN Level 1 Nutrition Coaching Certification. (You can enroll now at a big discount.)