Natural Remedies for Constipation: Unpacking the Efficacy of Prunes, Figs, and Exercise
The profound and often debilitating impact of chronic constipation on public health is undergoing a critical re-evaluation, moving beyond cultural taboos and into the realm of evidence-based natural interventions, primarily focusing on dietary adjustments and physical activity. Despite its widespread prevalence and significant health implications, the act of defecation remains a largely private matter, frequently overlooked even within medical discourse. This silence, however, belies a serious health challenge: constipation accounts for an staggering three million annual visits to doctors in the United States and contributes to 800,000 emergency room visits each year. Depending on how the condition is clinically defined, it is estimated that up to 80% of the population may experience some form of constipation, with many individuals potentially suffering without recognizing their symptoms as clinically significant. For instance, studies have revealed that a quarter of purportedly healthy participants reported experiencing "incomplete emptying," and about half indicated "increased straining" during bowel movements. Alarmingly, more than half had observed blood on their toilet paper within the past year, underscoring the severity of the issue. In severe cases, the physiological strain associated with defecation can lead to a dangerous spike in blood pressure, potentially triggering acute cardiovascular events such as heart attacks or strokes, highlighting the critical need for effective and accessible remedies.
The Overlooked Burden of Chronic Constipation
The statistics paint a stark picture of constipation’s societal burden. Beyond the sheer volume of medical consultations, the condition exacts a heavy toll on individuals’ quality of life, often leading to chronic discomfort, bloating, and a significant psychological impact, including anxiety and depression stemming from the persistent struggle. The economic cost is also substantial, encompassing direct healthcare expenditures, pharmaceutical costs, and indirect costs related to lost productivity and absenteeism. The insidious nature of constipation often means individuals normalize their symptoms, unaware that they could be experiencing clinically defined constipation. This lack of awareness underscores the importance of public health education campaigns that demystify bowel health and encourage proactive management. The potential for severe health outcomes, such as the aforementioned cardiovascular events, elevates constipation from a mere inconvenience to a serious public health concern warranting robust, evidence-based solutions.
Limitations of Pharmacological Interventions
For many years, the primary approach to managing constipation has involved pharmacological interventions. A range of drugs is available, from bulk-forming agents and stool softeners to osmotic and stimulant laxatives. While these medications can offer temporary relief, they frequently come with a spectrum of undesirable side effects, including nausea, diarrhea, headaches, and abdominal pain. This often leaves patients feeling unsatisfied and seeking alternative, more holistic solutions that address the root causes rather than merely alleviating symptoms. The cyclical nature of laxative dependence, where the gut becomes reliant on external stimulation, further complicates long-term management and contributes to patient frustration. This dissatisfaction with conventional treatments has spurred a renewed interest in non-pharmacological approaches, shifting the focus towards lifestyle and dietary modifications.
Lifestyle: The Cornerstone of Constipation Relief
A fundamental principle in addressing chronic constipation lies in modifying diet and lifestyle. Medical consensus increasingly points towards non-pharmacological, clinically effective interventions as the preferred first-line treatment. These interventions primarily center on increasing the intake of whole plant foods rich in fiber, ensuring adequate hydration, and incorporating regular physical activity into daily routines.
Dietary Fiber and Hydration:
Common causes of chronic constipation often include a deficiency in dietary fiber and insufficient water intake. Whole plant foods are the only naturally concentrated sources of fiber, which is crucial for promoting healthy bowel function. Fiber adds bulk to stool, making it softer and easier to pass. It also acts as a prebiotic, feeding beneficial gut bacteria and promoting a healthy microbiome, which plays an integral role in digestive regularity. Experts recommend an average daily fiber intake of 25 to 30 grams for adults, a target often unmet in modern Western diets dominated by processed foods. Coupled with fiber, adequate hydration is paramount. Water helps soften the stool and lubricates the intestinal tract, facilitating smooth passage. Dehydration can exacerbate constipation, as the colon absorbs water from stool, making it harder and more difficult to move.
Physical Activity:
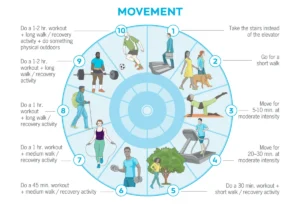
Beyond diet, engaging in regular physical activity is a potent, yet often underestimated, remedy for constipation. The recommendation typically involves about 30 minutes of moderate-intensity physical activity most days of the week. Scientific evidence supports this: a systematic review and meta-analysis of multiple studies found that aerobic exercise interventions significantly help alleviate constipation, with benefits observed starting at approximately 140 minutes per week. Exercise stimulates the natural contractions of the intestinal muscles, known as peristalsis, which moves stool through the digestive system. A sedentary lifestyle, conversely, can slow down gut motility, contributing to constipation. Integrating activities like walking, jogging, cycling, or swimming can therefore be a highly effective strategy.
Prunes: A Time-Honored Remedy Under Scrutiny
Among the natural remedies, prunes (dried plums) have long held a prominent place in folk medicine for their laxative properties. Recent scientific inquiry has sought to validate this traditional wisdom with rigorous, evidence-based research.
Early Investigations and the Placebo Effect:
Initial studies provided promising, albeit sometimes limited, insights. For instance, a study involving elderly women with severe constipation who were given approximately a dozen prunes a day reported significant improvement within the first week. However, the control group in this study received no intervention, a design limitation that raised questions about the potential influence of the placebo effect. The placebo effect in constipation trials is notoriously significant, with studies indicating that up to 44% of participants given an inert substance (a "sugar pill") might report an improvement in symptoms. This highlights the critical need for well-designed comparative studies to definitively ascertain the true efficacy of any intervention.
Rigorous Research: Prunes vs. Water and Psyllium:
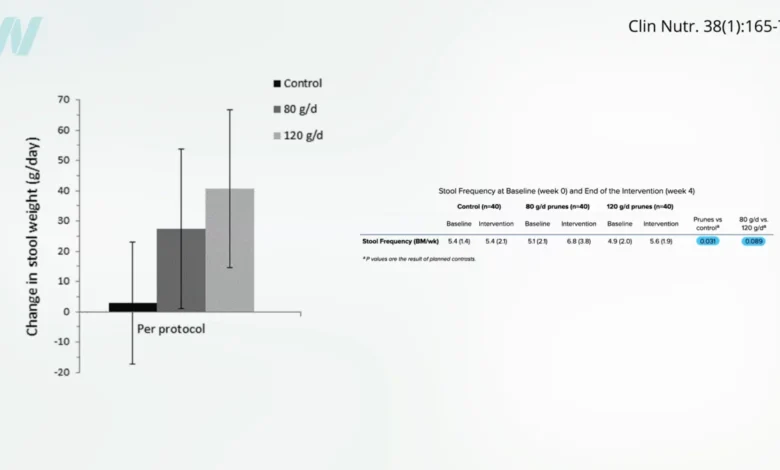
To overcome the limitations of earlier studies, more robust research designs were employed. One such randomized controlled trial assigned participants to one of three groups: about 8 prunes per day plus a large glass of water, 12 prunes per day plus water, or water alone. This design was crucial because even the control group received an intervention (water) known to potentially aid constipation. Researchers aimed to determine if a higher dose of prunes offered greater benefits than a moderate one. The findings were compelling: both prune groups showed a significant improvement in stool bulk and a significant increase in bowel movement frequency compared to the water-only control. Interestingly, there was no real statistical difference in efficacy between consuming 8 prunes and 12 prunes daily, suggesting that 8 prunes per day appears to be a sufficient and effective dose for most individuals.

Further strengthening the case for prunes, comparative studies have pitted them against common over-the-counter fiber supplements. Prunes have been found to be superior to psyllium, commonly sold as Metamucil, in terms of improving both stool frequency and consistency. This positions prunes not just as a natural alternative but potentially as a more effective option than some pharmaceutical-grade fiber supplements.
Mechanism Beyond Fiber and Safety Considerations:
For a long time, it was widely believed that the efficacy of prunes was solely attributable to their high fiber content. However, research into prune juice has challenged this notion. Prune juice, like most fruit juices, has its fiber largely removed during processing, yet it still demonstrates laxative effects. This suggests that other active components contribute to prunes’ therapeutic benefits. One such component is sorbitol, a natural sugar alcohol also found in some sugar-free gums. Sorbitol acts as an osmotic laxative, drawing water into the intestines and softening the stool. While effective, consuming more than a dozen or so large prunes a day could lead to sorbitol reaching laxative levels in susceptible individuals, potentially causing discomfort such as bloating or diarrhea. Therefore, moderation is key.
Interestingly, prunes have a dual historical use as both a laxative and an antidiarrheal remedy. This seemingly contradictory property underscores their unique physiological impact, likely related to their complex composition of fiber, sorbitol, and other phytochemicals that can help regulate bowel function depending on the existing gut state. Addressing concerns about whether individuals without constipation should avoid prunes, studies indicate that most people can safely consume around a dozen prunes a day without experiencing adverse effects, reinforcing their role as a beneficial dietary inclusion for general digestive health.
Figs: An Ancient Fruit’s Modern Efficacy
Figs, another fruit with a rich history spanning millennia and even mentioned in ancient texts like the Bible for their medicinal properties, have also garnered scientific attention for their potential in managing constipation.
Initial Studies and the IBS-C Challenge:
Early investigations into figs’ effectiveness included studies on patients with Irritable Bowel Syndrome characterized by constipation (IBS-C). In one such trial, participants were instructed to consume one fig with breakfast and one fig with lunch, each accompanied by a glass of water, while a control group maintained their normal diet. The fig group reported a significant improvement in the frequency of defecation and a notable reduction in the occurrence of hard stools. However, similar to the initial prune studies, the lack of an active control or a true placebo in this design raised concerns about the potential influence of the placebo effect. The placebo response in IBS trials is particularly pronounced, with up to 72% of patients sometimes reporting improvement from a fake sugar pill, underscoring the necessity for more rigorously controlled research.
The Gold Standard: Double-Blind, Placebo-Controlled Trials:
Recognizing the challenges posed by the placebo effect, researchers embarked on more sophisticated studies, employing randomized, double-blind, placebo-controlled designs. A notable example involved creating a "gross-sounding fake fig paste placebo" designed to mimic the taste, smell, and appearance of real figs, ensuring that neither participants nor researchers knew who was receiving the active treatment. Participants in this study consumed approximately six real figs daily. The findings suggested that those consuming real figs experienced "a significant reduction in colon transit time and a significant improvement in stool type [consistency] and abdominal discomfort" compared to the placebo group. Colon transit time, measured by having participants swallow small, radiopaque beads that could be tracked via X-rays through their digestive system, revealed that real figs sped up gut movement by a full 24 hours.
Despite these positive indicators, it’s important to note a key limitation: defecation frequency per week did not significantly outperform the placebo group in this study. Furthermore, the researchers tested numerous different outcomes, which increases the statistical probability of some "positive" findings occurring by chance (statistical flukes). Consequently, while figs show promise and offer some benefits, current evidence suggests that prunes may be a more consistently effective treatment choice for improving overall constipation symptoms, particularly regarding bowel movement frequency.
Expert Perspectives and Broader Implications
The growing body of evidence supporting the efficacy of natural remedies like prunes, figs, and lifestyle modifications marks a significant shift in the approach to managing constipation. Medical professionals increasingly advocate for these non-pharmacological interventions as a first-line strategy, particularly for mild to moderate cases. Organizations dedicated to digestive health often emphasize the "food first" approach, encouraging patients to explore dietary changes and increased physical activity before resorting to pharmaceutical options.
This renewed focus on natural remedies empowers patients, providing them with actionable strategies to manage their health proactively. It also informs public health messaging, highlighting the critical role of a balanced diet rich in whole plant foods and regular exercise in maintaining optimal digestive health and preventing chronic conditions. The implications extend beyond individual patient care, influencing dietary guidelines and health education programs aimed at reducing the overall burden of constipation on healthcare systems.
While natural remedies are highly effective for many, it is crucial to emphasize that severe or persistent constipation warrants medical consultation to rule out underlying conditions. The "Doctor’s Note" section in the original article points to other related topics such as carbonated drinks for stomach pain, the comparison of prunes with Metamucil, and the role of prunes in osteoporosis, underscoring the broader health benefits of these natural foods and the complexity of digestive health. Furthermore, ongoing research into the gut microbiome continues to shed light on how various dietary components, including fiber and prebiotics found in prunes and figs, influence gut health and motility.
In conclusion, the journey from cultural taboo to scientific validation for natural remedies like prunes, figs, and exercise represents a paradigm shift in constipation management. By addressing the root causes through a holistic approach encompassing diet, hydration, and physical activity, individuals can achieve significant relief and improve their overall quality of life, often bypassing the side effects and dissatisfaction associated with pharmacological alternatives. This integrative approach stands as a testament to the enduring power of natural interventions in modern healthcare.