Yeast infections causes and risk factors are crucial to understand for women’s health. This comprehensive guide delves into the various types of yeast infections, their common symptoms, and the underlying causes that contribute to their development. We’ll explore the role of hormonal changes, antibiotic use, and lifestyle choices in increasing susceptibility to these infections. Additionally, we’ll examine specific medical conditions and how they impact yeast infection risk.
Understanding the intricate interplay of factors that influence yeast overgrowth is essential for effective prevention and management. This article will guide you through a thorough exploration of the subject, covering everything from the normal vaginal flora to the latest medical interventions.
Introduction to Yeast Infections
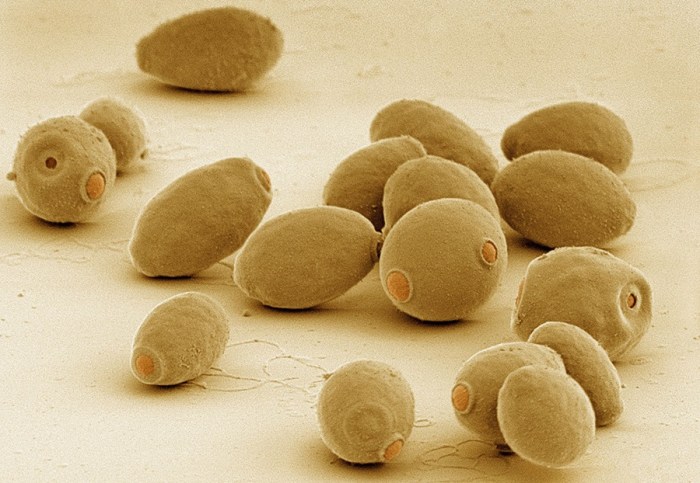
Yeast infections, also known as candidiasis, are common fungal infections caused by an overgrowth of the yeast
- Candida*, typically
- Candida albicans*. These infections can affect various parts of the body, leading to discomfort and sometimes requiring medical attention. Understanding the different types, symptoms, and causes is crucial for recognizing and managing these infections effectively.
Types of Yeast Infections
Yeast infections can manifest in various locations, each with its own characteristic symptoms. The most common types include vaginal, oral, and skin infections. The presence of normal vaginal flora plays a crucial role in preventing yeast infections. A healthy balance of bacteria and yeast in the vagina helps to keep the yeast population under control.
Vaginal Yeast Infections
Vaginal yeast infections are among the most prevalent types, affecting millions of women annually. These infections occur when the balance of the normal vaginal flora is disrupted, allowing the yeast population to multiply excessively. The symptoms of a vaginal yeast infection typically include itching, burning, redness, and a thick, white discharge resembling cottage cheese.
Oral Yeast Infections (Thrush)
Oral yeast infections, commonly referred to as thrush, are characterized by white patches or lesions on the tongue, inner cheeks, or roof of the mouth. These patches can sometimes be slightly raised and may cause pain or difficulty swallowing. Oral thrush can affect individuals of all ages, but it’s more prevalent in infants, young children, and people with weakened immune systems.
Skin Yeast Infections
Skin yeast infections, often referred to as cutaneous candidiasis, can occur on various parts of the body, including the skin folds, groin, and under the breasts. These infections can manifest as red, itchy, and inflamed skin, sometimes with a rash or cracking. Moist environments, such as those between skin folds, create ideal conditions for yeast overgrowth.
Normal Vaginal Flora and Yeast Infections
The normal vaginal flora, a complex ecosystem of bacteria and yeast, plays a vital role in maintaining a healthy vaginal environment. A healthy balance of bacteria inhibits the overgrowth ofCandida*. Disruptions to this balance, such as antibiotic use, hormonal changes, or stress, can disrupt the delicate equilibrium, leading to an overgrowth of yeast and subsequent infection.
Yeast infections, often uncomfortable, have various causes and risk factors, like antibiotic use or a weakened immune system. While dealing with these, exploring alternative pain management options like vertex painkiller opioid alternative can be helpful for managing other potential health concerns. Ultimately, understanding yeast infection causes and risk factors is key to preventing future issues and seeking appropriate medical advice.
Table of Yeast Infection Types
| Type of Yeast Infection | Location | Symptoms | Common Causes |
|---|---|---|---|
| Vaginal Yeast Infection | Vagina | Itching, burning, redness, thick white discharge | Antibiotic use, hormonal changes, pregnancy, diabetes |
| Oral Yeast Infection (Thrush) | Mouth | White patches or lesions on tongue, inner cheeks, roof of mouth, pain, difficulty swallowing | Weakened immune system, antibiotic use, dentures, poor oral hygiene |
| Skin Yeast Infection | Skin folds, groin, under breasts | Red, itchy, inflamed skin, rash, cracking | Moisture, tight clothing, diabetes, immune deficiency |
Underlying Causes of Yeast Infections
Yeast infections, also known as candidiasis, are a common vaginal issue. While often triggered by factors like hygiene and sexual activity, the underlying causes are frequently more complex, revolving around imbalances within the body’s environment. Understanding these underlying causes is key to prevention and effective management.The overgrowth ofCandida albicans*, the most common type of yeast found in the vagina, is the primary driver of these infections.
This overgrowth typically happens when the delicate balance of the vaginal microbiome is disrupted. This disruption can be due to a variety of factors, including hormonal fluctuations, antibiotic use, and underlying medical conditions. Understanding these factors helps us better comprehend the development and treatment of yeast infections.
Hormonal Changes
Hormonal fluctuations can significantly impact the vaginal environment, making women more susceptible to yeast infections. Pregnancy, with its associated hormonal shifts, is a prime example. The increased estrogen levels during pregnancy can lead to a more favorable environment for yeast overgrowth. Similarly, birth control pills, which also alter hormone levels, can affect the vaginal pH and create conditions that promote yeast colonization.
Menopause, with its fluctuating estrogen levels, can also increase the risk.
Antibiotic Use
Antibiotics, while crucial for treating bacterial infections, can disrupt the delicate balance of vaginal flora. This disruption occurs because antibiotics kill not only harmful bacteria but also beneficial bacteria, which help maintain the natural pH of the vagina and keep yeast populations in check. The reduction of these beneficial bacteria allows yeast to proliferate unchecked, leading to an infection.
A common example is a course of antibiotics for a urinary tract infection or a respiratory illness.
Medical Conditions
Certain medical conditions, particularly diabetes, can increase a woman’s risk of yeast infections. High blood sugar levels can create a more conducive environment for yeast growth. This is because the sugar in the vaginal area provides a nutrient source for yeast, allowing it to thrive. Other conditions like weakened immune systems, due to illness or medication, can also make individuals more prone to yeast infections.
This susceptibility arises from a compromised ability to fight off the overgrowth of yeast.
Comparison of Factors Influencing Yeast Overgrowth
| Factor | Mechanism | Impact on Yeast Overgrowth |
|---|---|---|
| Hormonal Changes (Pregnancy, Birth Control) | Increased estrogen levels create a more favorable environment for yeast growth. Changes in vaginal pH also contribute. | Increased susceptibility to yeast infections. |
| Antibiotic Use | Disruption of the vaginal microbiome by killing beneficial bacteria that maintain vaginal pH balance. | Increased risk of yeast overgrowth. |
| Medical Conditions (Diabetes) | High blood sugar levels provide nutrients for yeast growth. Compromised immune system can reduce the body’s ability to fight off infections. | Elevated risk of recurrent or persistent yeast infections. |
Risk Factors for Yeast Infections
Yeast infections, while common, can be uncomfortable and disruptive. Understanding the factors that increase your risk can empower you to take proactive steps toward prevention. Many lifestyle choices and underlying conditions can contribute to the overgrowth of yeast, leading to infection.Beyond the typical causes, several factors can make you more susceptible to yeast infections. These factors, often intertwined with everyday habits and health conditions, can significantly influence the risk of developing an infection.
Yeast infections are a common issue, often stemming from things like antibiotic use or a compromised immune system. But, sometimes, less obvious factors can play a role. For example, are you wondering about the potential effects of mixing certain medications, like antidepressants, with alcohol? If so, checking out this helpful guide on is it safe to mix lexapro and alcohol could provide some clarity.
Regardless, remember that a healthy lifestyle, including a balanced diet and regular exercise, can help mitigate the risk of yeast infections.
Understanding these risks is crucial for developing preventative strategies.
Lifestyle Choices Increasing Yeast Infection Risk
Certain lifestyle choices can create an environment more conducive to yeast overgrowth. Diet, stress levels, and even clothing choices play a role in your susceptibility.
- Tight Clothing: Tight-fitting clothing, particularly in the genital area, traps heat and moisture. This creates a warm, humid environment that encourages yeast growth. Examples include tight jeans or leggings, especially during warmer months. This increased moisture and warmth can lead to an environment ideal for the proliferation of yeast, contributing to the development of a yeast infection.
Yeast infections can be tricky, with various causes and risk factors. One thing that often gets overlooked is the impact of posture on overall health, including the potential effects on the immune system. Incorporating spinal extension and flexion exercise into your routine might help improve blood flow to the pelvic area, indirectly reducing the risk of yeast infections.
Of course, other risk factors like a weakened immune system or certain medications still need to be considered. Ultimately, understanding these factors can help you proactively manage your health. spinal extension and flexion exercise
- Hygiene Practices: While cleanliness is important, overly aggressive hygiene practices can disrupt the natural vaginal microbiome. Excessive douching, for example, can alter the balance of good bacteria, creating an opportunity for yeast to overgrow. Frequent use of harsh soaps or detergents in the genital area can also disrupt this balance.
- Stress Levels: Stress can weaken the immune system, making the body less able to fight off infections, including yeast infections. Chronic stress can negatively impact the body’s overall function and contribute to the development of a yeast infection. Stress hormones can alter the balance of vaginal bacteria, making it easier for yeast to thrive.
Impact of Douching on Vaginal Microbiome
Douching, a practice of rinsing the vagina with a liquid, is often perceived as a way to maintain hygiene. However, this practice can significantly disrupt the delicate balance of the vaginal microbiome.
Douching disrupts the natural vaginal flora, removing beneficial bacteria that help to keep yeast in check.
This disruption can lead to a decrease in healthy bacteria, creating a fertile ground for yeast to multiply and cause an infection. Furthermore, the chemicals in many douches can further irritate the vaginal tissues, compounding the problem.
Stress and Immune Function
Stress, a common aspect of modern life, has a significant impact on the immune system. Chronic stress can weaken the body’s natural defenses, making individuals more susceptible to various infections, including yeast infections.The connection between stress and immune function is well-documented. Stress hormones, released in response to stress, can suppress the immune system’s ability to fight off infections.
This compromised immune response creates an environment where yeast can proliferate more easily. Prolonged periods of high stress can lead to more frequent and severe yeast infections.
High-Risk vs. Low-Risk Lifestyle Factors
The table below contrasts lifestyle factors that increase the risk of yeast infections with those that contribute to a lower risk.
| Lifestyle Factor | Risk Level | Mechanism |
|---|---|---|
| Tight Clothing | High | Traps heat and moisture, creating a warm environment for yeast growth. |
| Excessive Douching | High | Disrupts the natural vaginal flora, allowing yeast to overgrow. |
| Chronic Stress | High | Weakened immune system allows for easier yeast infection development. |
| Balanced Diet | Low | Maintains overall health and supports a healthy immune system. |
| Loose, Breathable Clothing | Low | Allows for better ventilation, reducing moisture buildup. |
| Maintaining Proper Hygiene | Low | Preserves the natural balance of vaginal bacteria. |
Specific Factors and Conditions
Beyond the general risk factors, certain medical conditions and circumstances can significantly increase a woman’s susceptibility to yeast infections. Understanding these specific factors can help individuals proactively manage their health and seek appropriate medical attention when needed.Several factors, such as hormonal changes, immune system responses, and underlying health issues, can all contribute to an increased risk of yeast infections.
Understanding these factors can lead to preventative measures and effective treatment strategies.
Pregnancy
Pregnancy is a time of significant hormonal shifts, which can alter the balance of the vaginal environment. Elevated estrogen levels during pregnancy can create an environment more conducive to yeast overgrowth. Additionally, the physical changes and reduced mobility during pregnancy can make it more difficult to maintain good hygiene practices, further increasing risk. This heightened susceptibility often necessitates heightened vigilance and proactive care during this period.
Diabetes
Individuals with diabetes often experience recurring yeast infections. High blood sugar levels can provide an ideal environment for yeast to thrive. The persistent presence of glucose in the urine and on the skin can also contribute to the problem. Effective blood sugar management is crucial in preventing and managing these recurring infections.
Corticosteroids
Certain medications, particularly corticosteroids, can suppress the immune system, reducing the body’s ability to fight off infections. These medications are frequently used to treat various inflammatory conditions, but their immunosuppressive effects can increase the risk of yeast infections. Careful monitoring and consideration of alternative treatment options may be necessary in individuals taking corticosteroids.
Immunosuppression
Individuals with weakened immune systems, such as those undergoing chemotherapy or taking immunosuppressant medications, are particularly vulnerable to yeast infections. The reduced ability to fight off infections makes them more susceptible to opportunistic infections, including yeast infections. In these cases, prompt medical intervention and diligent hygiene practices are crucial.
Table: Medical Conditions and Yeast Infection Risk
| Condition | Mechanism | Impact on Yeast Infections |
|---|---|---|
| Pregnancy | Elevated estrogen levels, altered vaginal environment, reduced mobility, possible hygiene issues. | Increased susceptibility to yeast overgrowth; infections can occur more frequently. |
| Diabetes | High blood sugar levels, presence of glucose in urine and on skin. | Creates a favorable environment for yeast overgrowth, often leading to recurring infections. |
| Use of Corticosteroids | Suppression of the immune system, reducing the body’s ability to fight off infections. | Increases risk of yeast infections and other opportunistic infections. |
| Immunosuppression (e.g., Chemotherapy, certain medications) | Weakened immune response, reduced ability to fight off infections. | Significant vulnerability to opportunistic infections, including yeast infections. |
Prevention and Management
Yeast infections, while often manageable, can be frustrating and disruptive. Taking proactive steps to prevent them is key to maintaining comfort and overall well-being. Understanding the triggers and employing strategies to minimize their impact is crucial for long-term health.
General Preventive Measures
General preventive measures encompass a range of lifestyle adjustments aimed at reducing the risk of yeast overgrowth. These measures, when consistently practiced, can significantly lower the likelihood of recurring infections.
- Maintaining good hygiene is paramount. Regular cleaning of the genital area with mild soap and water, avoiding harsh chemicals, and thoroughly drying after bathing are crucial. Frequent douching should be avoided, as it can disrupt the natural pH balance and potentially introduce harmful substances.
- Wearing breathable clothing is essential. Tight-fitting, synthetic fabrics trap heat and moisture, creating an environment conducive to yeast growth. Loose-fitting, breathable cotton clothing allows for proper ventilation, helping to maintain a dry and healthy environment.
- Avoiding tight-fitting clothing, especially for extended periods, contributes to reducing moisture buildup and heat in the genital area, thus minimizing the risk of yeast infections.
Importance of Maintaining Good Hygiene
Proper hygiene plays a pivotal role in preventing yeast infections. Maintaining a healthy vaginal environment, free from irritants and conducive to a balanced microbiome, is essential. This involves avoiding harsh soaps, douches, and excessive cleaning. The natural pH balance of the vagina is delicate and should be respected. Disrupting this balance can lead to an overgrowth of yeast, triggering an infection.
Avoiding Triggers, Yeast infections causes and risk factors
Certain factors can act as triggers for yeast infections. Identifying and avoiding these triggers can significantly reduce the frequency and severity of infections.
- Using scented products in the genital area can disrupt the delicate vaginal pH balance, leading to an overgrowth of yeast. Choosing unscented products and avoiding scented hygiene products can prevent this trigger.
- Antibiotics can disrupt the normal vaginal flora, allowing yeast to overgrow. Taking antibiotics only when necessary and completing the full course of medication as prescribed is crucial.
- Tight clothing can increase moisture and heat in the genital area, creating an environment favorable to yeast growth. Opting for loose-fitting, breathable clothing is important.
Role of a Healthy Diet
A balanced diet rich in fruits, vegetables, and whole grains is crucial for maintaining a robust immune system. A strong immune system is better equipped to fight off infections, including yeast infections. Consuming foods rich in probiotics can also help to maintain a healthy vaginal microbiome, further reducing the risk of yeast overgrowth.
Preventive Strategies
| Strategy | Mechanism | Efficacy | Limitations |
|---|---|---|---|
| Wearing breathable clothing | Reduces moisture and heat in the genital area | High | May not be effective in all situations, such as extreme physical activity |
| Maintaining good hygiene | Removes irritants and promotes a balanced vaginal environment | High | Requires consistent practice and awareness |
| Avoiding triggers (e.g., scented products, antibiotics) | Prevents disruption of the vaginal pH balance and flora | High | Requires awareness of personal triggers and responsible use of medications |
| Maintaining a healthy diet | Supports immune function and promotes a healthy microbiome | Moderate | Diet alone may not be sufficient to prevent infections in all cases. |
Medical Interventions: Yeast Infections Causes And Risk Factors

Treating yeast infections often involves antifungal medications. These medications work by targeting the growth of the yeast, ultimately stopping the infection from spreading. Different forms of antifungal medication are available, each with varying degrees of effectiveness and side effects. Understanding these options allows individuals to make informed decisions about their treatment.
Common Antifungal Medications
Various antifungal medications are effective against yeast infections. These medications work by disrupting the yeast’s ability to reproduce or by directly killing the yeast cells. The choice of medication often depends on the severity of the infection, the location of the infection, and the individual’s overall health.
Types of Antifungal Medications
Antifungal medications come in various forms, each with its own advantages and disadvantages. Understanding the different forms helps individuals choose the most suitable treatment for their specific needs.
- Creams: Topical antifungal creams are commonly used for vaginal yeast infections. These creams are applied directly to the affected area, providing localized treatment. Examples include clotrimazole and miconazole creams, which are typically applied for a few days.
- Tablets: Oral antifungal tablets are often prescribed for more severe or recurrent yeast infections. These tablets work by targeting the yeast throughout the body. Examples include fluconazole, which is a single-dose treatment in many cases.
- Suppositories: Vaginal suppositories are another common treatment for vaginal yeast infections. These suppositories are inserted into the vagina and release medication to treat the infection. These medications typically work in a similar way to creams, but the medication is delivered in a different form.
Treatment Duration
The duration of treatment for yeast infections varies depending on the severity and the form of antifungal medication used. Typically, topical creams may require a few days of application, while oral tablets may need a single dose or a shorter course of treatment.
- Topical treatments: Topical creams and suppositories often require a 3-7 day treatment course, although some may be a single-dose treatment.
- Oral treatments: Oral treatments like fluconazole can often be resolved with a single dose, but multiple doses might be required for more complex cases. The specific duration depends on the individual’s response and the type of infection.
Efficacy and Side Effects of Treatments
The efficacy of antifungal medications varies. Some medications are highly effective at clearing up yeast infections, while others may not be as effective. Similarly, the potential side effects of different medications also vary. Some people may experience mild side effects, while others may experience more significant adverse reactions.
Summary Table of Antifungal Treatments
| Treatment | Mechanism | Benefits | Side Effects |
|---|---|---|---|
| Clotrimazole Cream | Disrupts fungal cell membrane function | Effective for localized infections, relatively low systemic absorption | Possible skin irritation, burning, itching |
| Fluconazole Tablets | Inhibits fungal cell growth | Effective for various yeast infections, often a single-dose treatment | Possible headache, nausea, diarrhea |
| Miconazole Cream | Disrupts fungal cell membrane function | Effective for localized infections, good for vaginal yeast infections | Possible vaginal irritation, burning, itching |
| Terconazole Suppositories | Disrupts fungal cell membrane function | Effective for vaginal yeast infections, good for deep infections | Possible vaginal irritation, burning, itching |
Concluding Remarks
In conclusion, yeast infections can stem from a variety of factors, ranging from hormonal fluctuations to lifestyle choices and underlying medical conditions. By understanding the causes, risk factors, and preventative measures, you can take proactive steps to manage and prevent yeast infections. This knowledge empowers you to make informed decisions about your health and well-being.

