What does vulvovaginitis look like? Understanding the visual cues and symptoms is crucial for early detection and treatment. This guide delves into the appearance of vulvovaginitis, covering everything from common symptoms to visual characteristics across different types. We’ll explore the various presentations, potential underlying causes, and when to seek medical attention.
This comprehensive overview will provide valuable insights into recognizing the signs of vulvovaginitis, empowering you to take proactive steps towards your well-being. We’ll also discuss how symptoms can vary based on individual factors, highlighting the importance of personalized care.
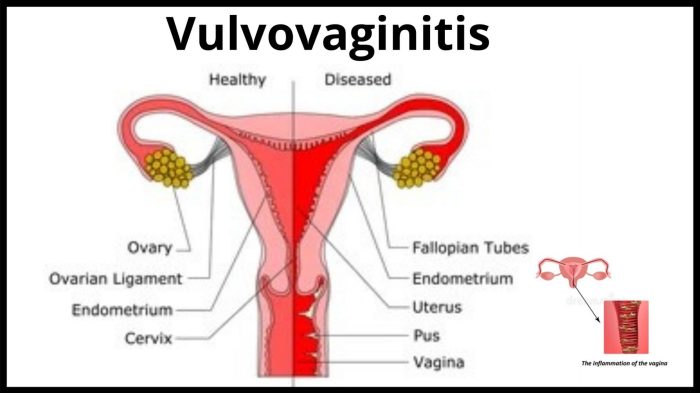
Defining Vulvovaginitis: What Does Vulvovaginitis Look Like
Vulvovaginitis is a general term for inflammation of the vulva and vagina. It’s a common condition affecting women of all ages, often presenting with discomfort and sometimes noticeable changes in vaginal discharge. Understanding the different types and causes of vulvovaginitis is crucial for proper diagnosis and treatment. This will help you better understand the symptoms and know when to seek medical attention.
Types of Vulvovaginitis
Vulvovaginitis can be caused by a variety of factors, resulting in different presentations. Common causes include bacterial infections, fungal infections, and other less frequent but still important factors. Understanding these distinctions allows for tailored treatment approaches.
Bacterial Vulvovaginitis
Bacterial vaginosis (BV) is a common cause of vaginitis, characterized by an overgrowth of bacteria normally present in the vagina. This imbalance disrupts the natural vaginal flora, leading to changes in vaginal discharge. Symptoms typically include thin, grayish-white discharge, a fishy odor, and itching or burning sensations. Some women may experience no symptoms at all.
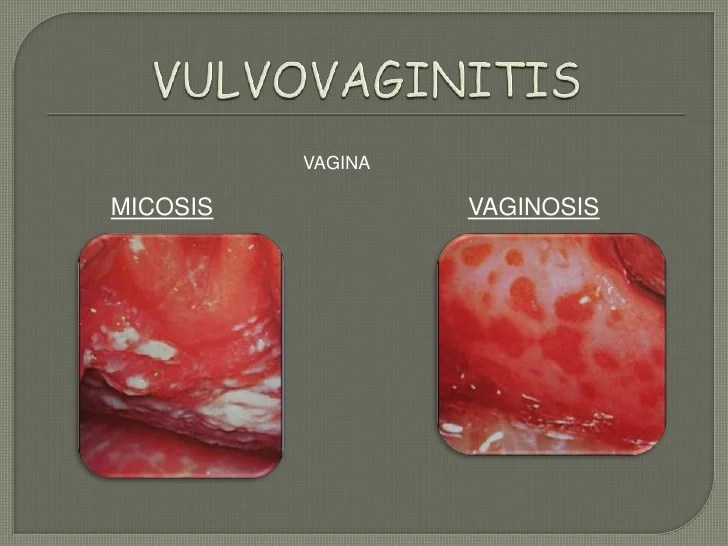
Fungal Vulvovaginitis
Yeast infections, caused by theCandida* fungus, are another frequent cause of vulvovaginitis. The fungus naturally resides in the vagina but can overgrow, leading to inflammation. Symptoms commonly include thick, white, clumpy discharge, intense itching, burning, and redness around the vulva. Symptoms can vary from mild to severe.
Other Causes of Vulvovaginitis
Various other factors can contribute to vulvovaginitis, including allergic reactions, irritants, hormonal changes, and sexually transmitted infections (STIs). These can produce a range of symptoms depending on the underlying cause.
Understanding what vulvovaginitis looks like can be tricky, as symptoms can vary. Sometimes it presents as redness and swelling, other times with unusual discharge. If you’re looking for expert advice on skin conditions, especially for those with skin of color, ask an expert dermatologist for skin of color for personalized guidance. Ultimately, seeking professional help is key to getting a proper diagnosis and treatment plan for vulvovaginitis.
Table of Vulvovaginitis Causes, What does vulvovaginitis look like
| Cause | Symptoms | Typical Presentation |
|---|---|---|
| Bacterial Vaginosis (BV) | Thin, grayish-white discharge; fishy odor; itching/burning; no symptoms in some cases | Often asymptomatic or presents with mild symptoms. Discharge may be noticeable after sexual activity. |
| Yeast Infection (Candidiasis) | Thick, white, clumpy discharge; intense itching; burning; redness around vulva | Frequently presents with noticeable symptoms like itching and discharge. |
| Allergic Reactions/Irritants | Itching, burning, redness, swelling; can vary depending on the allergen or irritant | Symptoms can be localized or widespread. May be triggered by specific products or materials. |
| Hormonal Changes | Irregular discharge; itching; burning; changes in vaginal dryness | Often associated with periods of hormonal fluctuation, such as pregnancy, menopause, or birth control changes. |
| Sexually Transmitted Infections (STIs) | Discharge (varying colors and consistency); pain during urination or intercourse; sores or blisters | Symptoms can range from mild to severe and can include signs of inflammation, pain, and discomfort. |
Identifying Symptoms
Recognizing the signs of vulvovaginitis is crucial for timely diagnosis and treatment. Understanding the range of symptoms, from mild irritation to severe pain, is key to seeking appropriate medical help. This section details the common symptoms associated with various types of vulvovaginitis, highlighting potential differences and severity levels.Identifying the specific type of vulvovaginitis can be challenging based solely on symptoms.
A healthcare professional will consider multiple factors, including medical history, physical examination, and potentially laboratory tests, to reach an accurate diagnosis. Self-diagnosis is not recommended.
Common Symptoms of Vulvovaginitis
Various symptoms can manifest, ranging from mild discomfort to severe pain. These symptoms often overlap between different types of vulvovaginitis, making precise identification difficult without professional evaluation.
- Burning sensation: A persistent or intermittent burning feeling in the vulva and vaginal area is a frequent complaint. This can range from a mild, irritating warmth to a more intense, sharp burning sensation.
- Itching: Intense itching in the vulvar area is another common symptom, often accompanied by redness and swelling. This itching can be constant or intermittent, and can be disruptive to daily activities.
- Discharge: Abnormal vaginal discharge is a hallmark symptom. This discharge may be different in color, consistency, or odor depending on the underlying cause. It can range from a thin, white discharge to a thick, yellow or green discharge.
- Pain during urination or intercourse: Painful urination (dysuria) or painful sexual intercourse (dyspareunia) can be associated with vulvovaginitis. This pain may vary in intensity and can be a significant factor in determining the need for medical attention.
- Swelling and redness: Swelling and redness of the vulva and vaginal area are common indicators of inflammation. The degree of swelling and redness can vary depending on the severity of the condition.
Differences in Symptoms Based on Type
Different types of vulvovaginitis can present with slightly varying symptom profiles. Recognizing these subtle differences can help healthcare professionals in making an accurate diagnosis.
| Type of Vulvovaginitis | Common Symptoms | Potential Differences |
|---|---|---|
| Bacterial Vaginosis (BV) | Thin, gray, or white discharge; fishy odor; burning; itching; redness | Discharge may be less noticeable in some cases. Odor is a key distinguishing factor. |
| Yeast Infection (Candidiasis) | Thick, white, clumpy discharge; itching; burning; redness; soreness | Symptoms may be more pronounced during menstruation or after antibiotic use. |
| Trichomoniasis | Greenish-yellow, frothy discharge; itching; burning; pain during urination or intercourse; bad odor | Symptoms may be more pronounced in women with a history of multiple sexual partners. |
| Atrophic Vaginitis | Dryness; burning; itching; pain during intercourse; bleeding after intercourse; postmenopausal women | Symptoms can be more prominent in postmenopausal women due to hormonal changes. |
Symptoms Varying by Age and Experience
The presentation of vulvovaginitis symptoms can differ based on age and individual experiences. For example, children may experience more subtle symptoms or present with behavioral changes.
- Children: Symptoms in children might include irritability, discomfort during urination, or difficulty sitting. Parents should be vigilant about unusual behavior and changes in hygiene habits.
- Adolescents: Symptoms in adolescents may mirror those in adults, but concerns about social implications or embarrassment may influence their willingness to seek help.
- Women experiencing hormonal fluctuations: Women experiencing hormonal changes, such as during pregnancy or menopause, may experience more severe symptoms or have symptoms that differ from their usual experience.
Visual Characteristics
Understanding the visual cues of vulvovaginitis is crucial for early diagnosis and appropriate treatment. Different types of vulvovaginitis can present with various appearances, and recognizing these patterns can help distinguish between potential causes. Paying close attention to the color, consistency, and location of any discharge, redness, or swelling can significantly aid in identifying the underlying issue.
Appearance of the Vulva and Vagina in Different Types of Vulvovaginitis
The visual presentation of vulvovaginitis can vary greatly depending on the specific cause. Factors like the presence of an infection, an allergic reaction, or a hormonal imbalance can all contribute to different visual characteristics. This section details common visual changes associated with different types of vulvovaginitis.
Visual Changes in Affected Areas
Visual changes in the vulva and vagina can include redness, swelling, itching, and discharge. The color, consistency, and amount of discharge, along with the location of any sores or lesions, are important diagnostic clues. For example, a thick, white discharge might suggest a yeast infection, while a thin, yellow-green discharge could point towards a bacterial infection.
Table of Visual Descriptions
The table below summarizes common visual characteristics associated with different types of vulvovaginitis. It provides a quick reference guide for identifying potential issues.
| Type of Vulvovaginitis | Color of Discharge | Consistency of Discharge | Location of Affected Areas | Other Visual Changes |
|---|---|---|---|---|
| Bacterial Vaginosis | Grayish-white or yellowish | Thin, watery, or frothy | Vaginal area, often with a fishy odor | Possible mild redness or irritation |
| Yeast Infection (Candidiasis) | Thick, white, clumpy | Often described as cottage cheese-like | Vaginal area, vulva, and surrounding skin | Intense itching and burning are common |
| Trichomoniasis | Yellow-green or greenish-gray | Frothy, sometimes foamy | Vaginal area, often with a strong odor | Redness, swelling, and painful urination |
| Allergic Reaction | Variable; may be clear or slightly cloudy | Watery or mucoid | Vulva, vagina, and surrounding skin | Significant itching, swelling, and possible burning |
Visual Representation of Normal Vulva and Vagina
A healthy vulva and vagina appear smooth and pinkish-red. The labia majora and minora are typically soft to the touch, and the vaginal opening is closed. There should be no noticeable swelling, redness, or discharge. In contrast, vulvovaginitis is characterized by inflammation and changes in the color, consistency, and amount of discharge. Comparing the normal appearance to the affected area can be helpful in identifying vulvovaginitis.
This can be done with a physical examination by a medical professional.
How Visual Cues Vary Based on Underlying Causes
The visual cues of vulvovaginitis can vary depending on the underlying cause. For instance, a yeast infection might present with a thick, white discharge, while an allergic reaction could manifest as intense itching and swelling. In some cases, the visual characteristics may be subtle and not readily apparent. Therefore, a thorough evaluation by a healthcare provider is crucial for accurate diagnosis and effective treatment.
Symptoms such as odor, pain, and other associated factors must be considered alongside the visual changes to create a comprehensive picture of the condition.
Differential Diagnosis
Understanding vulvovaginitis involves recognizing that similar symptoms can arise from various conditions. Accurate diagnosis hinges on distinguishing vulvovaginitis from other potential causes, leading to appropriate treatment. Differentiating between vulvovaginitis and other conditions requires careful symptom analysis and medical evaluation.Identifying the precise cause of vulvovaginal discomfort is crucial for effective treatment. Misdiagnosis can lead to inappropriate therapies and delayed resolution of the underlying issue.
Therefore, a thorough evaluation by a healthcare professional is essential.
Conditions Mimicking Vulvovaginitis
Several conditions can present with symptoms that overlap with vulvovaginitis, making differentiation challenging. These conditions include bacterial infections, yeast infections, sexually transmitted infections, allergic reactions, and skin disorders. Proper diagnosis requires a detailed history, physical examination, and potentially, laboratory testing.
Differentiating Symptoms
Precise symptom analysis is key to distinguishing vulvovaginitis from other conditions. For example, while itching and burning are common in vulvovaginitis, they can also be present in allergic reactions. The presence of other symptoms, such as discharge characteristics, odor, and pain during urination, can provide crucial clues for differentiation.
Importance of Medical Evaluation
Medical evaluation is paramount for accurate diagnosis. A healthcare provider can conduct a physical examination, assess the patient’s medical history, and order necessary tests, such as Pap smears, cultures, or swabs. These diagnostic tools aid in identifying the specific cause of the symptoms. This is especially important for conditions that may mimic vulvovaginitis, like sexually transmitted infections, which require specific treatments.
Comparison Table
| Condition | Symptoms | Key Differentiating Factors |
|---|---|---|
| Vulvovaginitis (Bacterial) | Burning, itching, unusual discharge (may be thick, white, or yellow), odor | Often associated with a history of douching or antibiotic use. May exhibit symptoms of bacterial vaginosis. |
| Vulvovaginitis (Yeast) | Itching, burning, thick, white, clumpy discharge | Often associated with a history of diabetes, pregnancy, or use of antibiotics. Discharge may resemble cottage cheese. |
| Sexually Transmitted Infections (STIs) | Burning, itching, unusual discharge (may be watery, green, or yellow), pain during urination, sores or blisters | Often accompanied by other symptoms, such as painful urination, sores, or blisters. May have a history of unprotected sexual activity. |
| Allergic Reactions | Itching, burning, redness, swelling, possible rash | Often triggered by contact with certain substances (soaps, perfumes, etc.). Symptoms may be localized to the vulva. |
| Skin Disorders | Itching, burning, redness, scaling, cracking | May exhibit characteristic skin changes. Often associated with a history of skin conditions. |
Significance of Medical Evaluation
A thorough medical evaluation is essential to rule out other potential causes of vulvovaginal symptoms. A healthcare professional can accurately assess the patient’s condition, considering factors such as medical history, lifestyle, and any recent changes. This approach helps in avoiding misdiagnosis and ensures the most appropriate and effective treatment. For example, a patient experiencing vaginal pain and discharge might initially suspect vulvovaginitis.
However, a medical evaluation might reveal an underlying condition requiring different treatment, like endometriosis.
Wondering what vulvovaginitis looks like? It can manifest as redness, swelling, and discharge, varying in color and consistency. Understanding how infections spread, like through the fecal-oral route, for example, fecal oral route for transmission of infection , is crucial. Knowing the different ways infections can be passed on helps us recognize the symptoms and take appropriate preventative measures.
Ultimately, paying attention to any unusual changes in your vaginal area is important for early diagnosis and treatment.
Important Considerations
Navigating vulvovaginitis can feel overwhelming. Understanding the nuances of when to seek help, maintaining good hygiene, and recognizing the impact on daily life is crucial for effective management. This section provides practical advice and insights to empower you in your journey toward recovery.
When to Seek Medical Attention
Persistent or worsening symptoms are a key indicator for seeking professional help. Symptoms like severe pain, fever, unusual discharge with a foul odor, or significant changes in urination should prompt immediate consultation with a healthcare provider. Untreated vulvovaginitis can lead to complications, making early intervention vital. If you experience any of these concerning symptoms, do not hesitate to schedule an appointment.
So, what does vulvovaginitis look like? It can manifest in various ways, from mild discomfort to more noticeable symptoms like itching, burning, and unusual discharge. Sometimes, these symptoms can be linked to underlying conditions, like the potential role of mood stabilizers in dementia. Exploring the effects of mood stabilizers in these situations, as detailed in this article on mood stabilizers role in dementia , is crucial to understanding the full picture.
Ultimately, it’s always best to consult a healthcare professional for accurate diagnosis and personalized treatment plans for vulvovaginitis.
Importance of Hygiene Practices
Maintaining proper hygiene plays a vital role in preventing vulvovaginitis. This involves using mild, unscented soaps and avoiding harsh chemicals or scented products in the genital area. Excessive cleaning can disrupt the natural pH balance, increasing the risk of infection. Changing underwear frequently, especially after physical activity or swimming, is also crucial.
Potential Impact on Daily Life and Well-being
Vulvovaginitis can significantly affect daily life, impacting physical comfort, self-esteem, and overall well-being. Painful symptoms can make sitting, walking, or engaging in intimate activities uncomfortable. The emotional toll of dealing with an infection should not be underestimated. Understanding that these symptoms are treatable and manageable can help ease anxieties and improve quality of life.
Importance of a Proper Diagnosis for Effective Treatment
A proper diagnosis is essential for successful treatment. Different types of vulvovaginitis require tailored approaches. An accurate diagnosis, obtained through a physical examination and potentially lab tests, ensures the most effective treatment plan. This personalized approach maximizes the likelihood of a positive outcome and prevents the risk of ineffective or inappropriate treatment.
Symptom Checklist for Potential Vulvovaginitis
This checklist can help you identify potential vulvovaginitis symptoms. It’s important to remember that this is not a substitute for professional medical advice. Consult a healthcare provider if you experience any of these symptoms:
- Burning or itching in the vulva and vagina
- Unusual vaginal discharge (color, odor, consistency)
- Pain during urination or sexual intercourse
- Swelling or redness in the vulva
- Changes in menstrual cycle (increased bleeding or unusual discharge)
- Painful sores or blisters in the genital area
- Fever or chills
- General discomfort or pain in the pelvic area
Illustrative Examples of Vulvovaginitis
Understanding the diverse presentations of vulvovaginitis is crucial for accurate diagnosis and effective treatment. Different causes and underlying conditions can lead to varied symptoms and visual characteristics, making a nuanced approach essential. This section provides detailed examples to illustrate the potential spectrum of vulvovaginitis presentations.
Scenarios Across Age Groups
Visual presentations and symptoms of vulvovaginitis can differ significantly based on age. This variation reflects the differing hormonal influences and potential underlying factors in various developmental stages. Analyzing these variations allows for a more targeted approach to diagnosis and management.
| Age Group | Potential Causes | Key Visual Cues | Symptoms |
|---|---|---|---|
| Infants and Toddlers (0-3 years) | Yeast infections, bacterial vaginosis, irritation from diapers, foreign bodies | Redness, swelling, excoriation (skin breakdown), possible discharge. May show localized or generalized redness around the vulva. | Irritability, fussiness, difficulty urinating, localized pain or discomfort, a thin, whitish, or yellowish discharge. Infants may exhibit increased frequency of diaper changes. |
| Prepubescent Girls (4-9 years) | Yeast infections, bacterial vaginosis, pinworms, foreign bodies, skin irritation, or allergies | Redness, swelling, itching, small spots or blisters, or patchy areas of irritation. Discharge might be minimal or absent, but there may be noticeable soreness or tenderness. | Itching, burning, discomfort during urination, localized pain or soreness, sometimes a whitish or yellowish discharge. May exhibit restlessness or difficulty with activities. |
| Pregnant Women | Bacterial vaginosis, yeast infections, trichomoniasis, irritation from certain hygiene products or clothing | Increased discharge, redness, swelling, possible odor, and pain or discomfort during urination or sexual intercourse. In some cases, there might be visible lesions or inflammation. | Increased vaginal discharge (may have a strong odor), burning, itching, discomfort during urination or sexual intercourse, pain during vaginal examination, or pelvic pain. |
| Postmenopausal Women | Atrophic vaginitis, yeast infections, bacterial vaginosis, irritation from hygiene products, or infections from other sources. | Dryness, thinning of the vaginal lining, redness, itching, burning, and possible bleeding. Vaginal discharge may be minimal or absent, but the area may be tender or painful. | Vaginal dryness, itching, burning, pain with intercourse, bleeding after intercourse or without any apparent reason, possible urinary issues. |
Impact of Underlying Medical Conditions
Certain medical conditions can significantly affect the presentation of vulvovaginitis. For example, diabetes can predispose individuals to recurrent yeast infections, manifesting with more frequent and severe symptoms. Similarly, autoimmune conditions may lead to a more chronic and persistent inflammatory response in the vulvovaginal area, characterized by unusual or persistent symptoms.
Examples of Different Presentations
A young girl presenting with vulvar itching, a small amount of whitish discharge, and localized redness could indicate a yeast infection. However, the same symptoms could also suggest an allergic reaction to a new laundry detergent or other irritants. A woman with a history of diabetes experiencing frequent, intense vaginal itching and a thick, clumpy discharge is more likely to have a persistent yeast infection.
This highlights the importance of a comprehensive history and physical examination to determine the most appropriate course of treatment.
Final Thoughts
In summary, recognizing the signs of vulvovaginitis involves understanding the range of visual and symptom presentations. While this guide offers valuable insights, remember that accurate diagnosis and treatment require a medical professional. Always consult a healthcare provider for any concerns regarding vulvovaginitis or similar conditions. Early intervention is key to managing symptoms and preventing potential complications.