Congestion and nasal symptoms during pregnancy can be a real drag, but understanding the causes, symptoms, and solutions can make a huge difference. From hormonal shifts to environmental factors, pregnancy brings a whole host of changes that can affect your sinuses. This guide explores the why, how, and what to do about nasal discomfort during…
Does Birth Control Make You Moody? A Deep Dive
Does birth control make you moody? This is a question that affects many women, and understanding the connection between hormonal birth control and mood is crucial for making informed decisions about your health. We’ll explore the hormonal shifts associated with various birth control methods, examining how they might impact mood, and discuss individual variations and…
Robaxin vs Amrix Similarities and Differences Explained
Robaxin vs Amrix similarities and differences explores the nuances of these muscle relaxants. Understanding their shared goals and distinct mechanisms of action is key for informed decisions about treatment. This comparison delves into chemical structures, potential side effects, dosages, and clinical applications, ultimately helping readers grasp the critical distinctions between these often-prescribed medications. This comprehensive…
Citicoline Cognitive Benefits Unveiled
The cognitive benefits of citicoline are increasingly recognized, offering a potential avenue for enhancing mental performance. This exploration delves into the fascinating world of citicoline, examining its chemical properties, mechanisms of action, and the scientific evidence supporting its role in cognitive enhancement. We’ll unpack how citicoline might bolster memory, learning, and overall cognitive function, while…
Cluster Headache vs. Migraine A Deep Dive
Cluster headache vs migraine – Cluster headache vs. migraine: Understanding the differences between these debilitating headaches is crucial for effective management. Both can significantly impact daily life, causing intense pain and discomfort. This in-depth exploration delves into the key similarities and differences, providing a comprehensive overview of symptoms, diagnosis, treatment, and the overall impact on…
Bendopnea A New Heart Failure Symptom
Bendopnea a new symptom of heart failure – Bendopnea, a new symptom of heart failure, describes a specific type of shortness of breath that occurs when bending over. This distinct respiratory response, different from typical dyspnea, may indicate underlying heart conditions. Understanding its characteristics, physiological mechanisms, and clinical presentation is crucial for accurate diagnosis and…
Portfolio Diet Heart Health Your Guide
Portfolio diet heart health is a comprehensive approach to achieving and maintaining cardiovascular well-being. It’s not about strict adherence to one single diet, but rather strategically incorporating diverse dietary patterns to support optimal heart health. This includes understanding different approaches like the Mediterranean or DASH diet, and recognizing the vital role of various nutrients and…
Milk of Magnesia How Quickly Will It Work?
Milk of magnesia how quickly will it work – Milk of magnesia, how quickly will it work? This question is crucial for anyone experiencing heartburn, indigestion, or other stomach upsets. Understanding the mechanisms behind its effectiveness, along with factors influencing its speed of action, is key to getting relief quickly and efficiently. We’ll delve into…
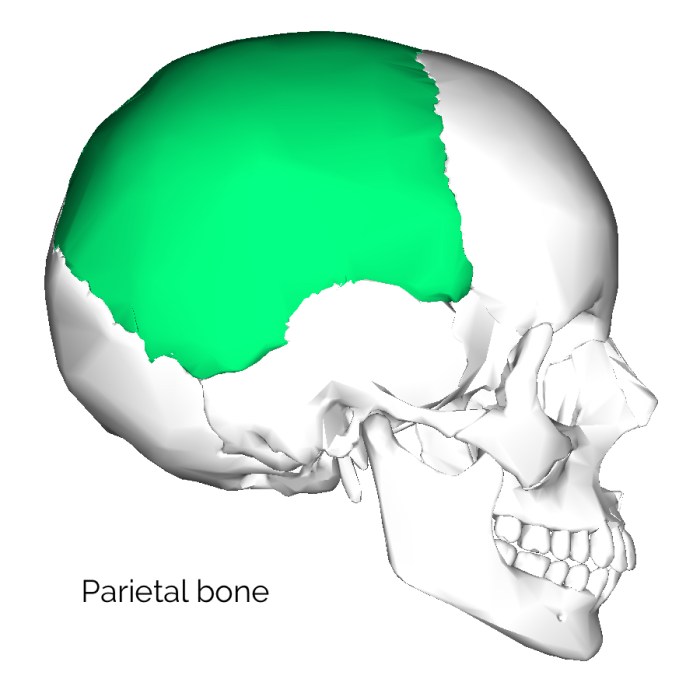
Effects of a Parietal Lobe Stroke A Comprehensive Guide
Effects of a parietal lobe stroke encompass a wide range of debilitating symptoms, impacting various aspects of daily life. This comprehensive guide delves into the intricate functions of the parietal lobe, exploring the different areas and their roles, as well as the common causes of strokes affecting this region. We’ll also explore the varied symptoms,…
Is Epstein Barr Linked to Autoimmune Disease?
Is Epstein Barr linked to autoimmune disease? This question delves into the complex relationship between the Epstein-Barr virus (EBV) and a range of autoimmune conditions. EBV, a common virus, infects many people, but its potential role in triggering or worsening autoimmune responses is a subject of ongoing research. Understanding this connection is crucial for diagnosis,…