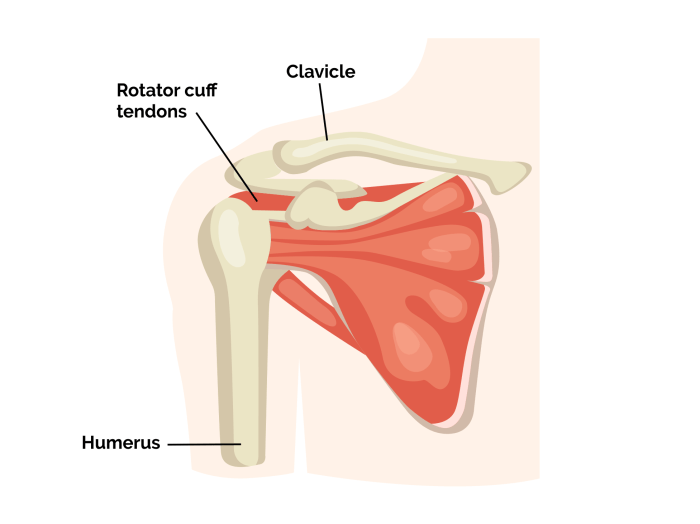
Rotator cuff tear surgery is a significant procedure that addresses a common shoulder ailment. Understanding the different types of tears, the diagnostic process, surgical techniques, and the crucial role of rehabilitation is essential for anyone considering this option. This comprehensive guide will delve into the intricacies of rotator cuff tear surgery, exploring everything from the…
How Much Ibuprofen Is Too Much?
How much ibuprofen is too much? This crucial question affects everyone who uses this common pain reliever. Understanding the proper dosage, potential side effects, and signs of an overdose is vital for safe and effective use. This comprehensive guide will explore the details of ibuprofen dosage, potential dangers of overuse, and steps to take if…
Become an OB/GYN Physician A Detailed Guide
Become ob gyn physician – Become an OB/GYN physician: This journey delves into the fascinating world of obstetrics and gynecology, exploring the educational requirements, necessary skills, and diverse career paths. From meticulous medical training to patient interaction, the path to becoming an OB/GYN physician is demanding yet incredibly rewarding. This guide Artikels the key steps,…
Nausea Medicine for Pregnancy A Comprehensive Guide
Nausea medicine for pregnancy is a crucial aspect of prenatal care, offering pregnant women essential support during a challenging time. This comprehensive guide explores the physiological causes of morning sickness, comparing them to other potential causes of nausea. We’ll delve into various over-the-counter and prescription medications, natural remedies, and lifestyle strategies for managing nausea. Dietary…
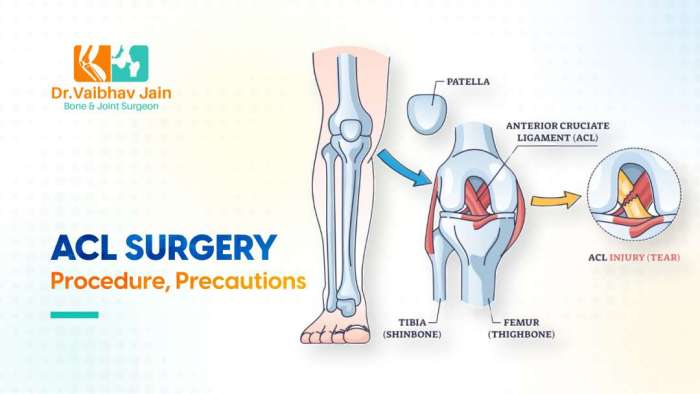
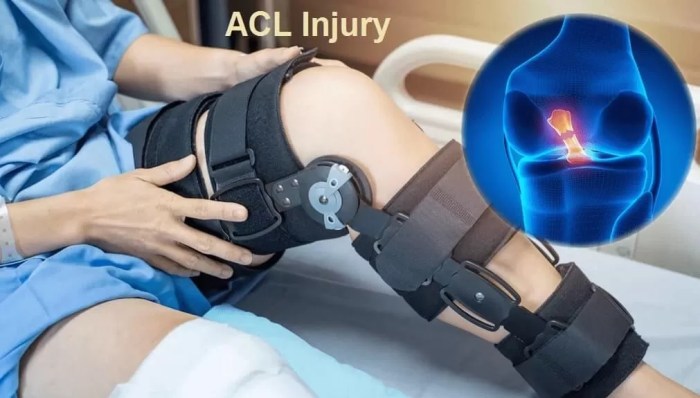
How ACL Surgery Is Performed A Comprehensive Guide
How ACL surgery is performed is a complex procedure, but understanding the process can ease anxieties. This in-depth look explores the various stages, from initial diagnosis to post-operative rehabilitation, offering a clear and concise overview of the entire journey. We’ll delve into pre-operative assessments, surgical techniques, and the critical role of post-operative care in achieving…
Finding the Best Doctor for Elderly Mother
Finding the best doctor for elderly mother is a crucial decision that demands careful consideration. It’s not just about finding someone who’s qualified, but about finding a doctor who understands and respects the unique needs of aging individuals. This involves looking at various factors, from location and insurance coverage to the doctor’s experience with elderly…
Responding to Confabulation in Dementia A Guide
Responding to confabulation in dementia is a crucial aspect of caregiving. This guide dives deep into understanding confabulation in dementia, from its definition and triggers to effective response strategies and communication techniques. We’ll explore how to identify confabulation, differentiate it from other cognitive impairments, and create supportive environments to help manage these episodes. This comprehensive…
ACL Surgery Making Your Decision
ACL surgery making a decision is a crucial juncture, often fraught with anxiety and uncertainty. This exploration delves into the multifaceted considerations surrounding this choice, from understanding the nuances of the injury itself to weighing surgical versus non-surgical options. We’ll navigate the decision-making process, examining the various factors that contribute to the best possible outcome…
What is Light Box Therapy? A Comprehensive Guide
What is light box therapy? This therapy uses specialized lights to treat various conditions, primarily impacting mood and sleep patterns. Different types of light boxes emit varying wavelengths, each potentially affecting the body in distinct ways. Understanding the science behind light box therapy, along with the types of light boxes and their applications, is crucial…
Health Benefits Jamu Drink A Deep Dive
Health benefits jamu drink, a traditional Indonesian herbal beverage, opens a fascinating window into the rich tapestry of natural remedies. From its historical roots in Southeast Asian cultures to its potential modern applications, jamu offers a unique perspective on holistic wellness. This exploration will delve into the diverse types of jamu drinks, their potent ingredients,…