VCF vaginal contraceptive film offers a novel approach to birth control, potentially providing a comfortable and effective alternative to traditional methods. This in-depth exploration covers everything from its history and different types to its effectiveness, application, and user experiences. We’ll also delve into the potential benefits and drawbacks, compare it to other contraceptives, and discuss…
Women Experience More Flu Shot Reactions A Deep Dive
Women experience more flu shot reactions, a topic demanding exploration. This post delves into the potential reasons behind this observation, from biological factors to pre-existing health conditions. We’ll examine common side effects, the severity of reactions, and strategies for managing them, ultimately aiming to provide a comprehensive understanding of this phenomenon. This in-depth analysis considers…
Can I Have Celiac Disease and Constipation?
Can I have celiac disease and constipation? This question touches on a common concern for those experiencing digestive issues. Celiac disease, an autoimmune disorder triggered by gluten, significantly impacts the small intestine. Constipation, characterized by infrequent bowel movements, can stem from various factors. This exploration delves into the potential overlap between these two conditions, examining…
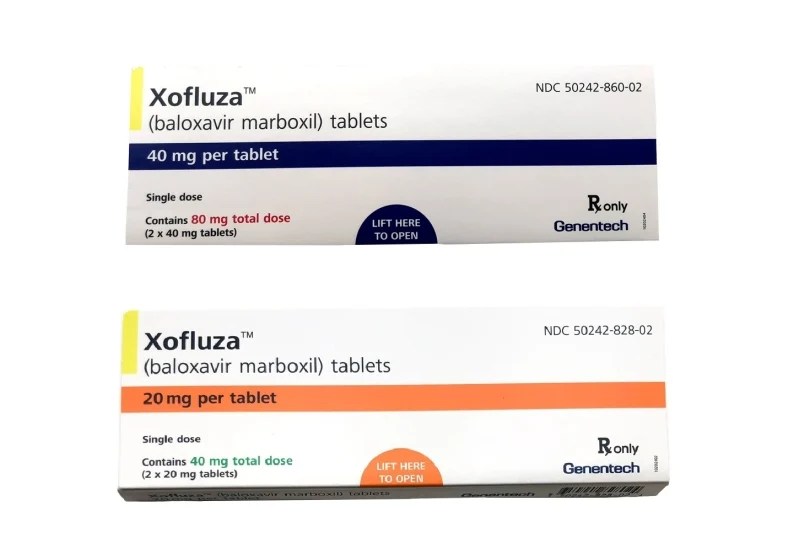
Xofluza vs Tamiflu for Flu Differences & Similarities
Xofluza vs Tamiflu for flu differences and similarities is a crucial comparison for anyone facing the flu. Both are antiviral medications, but how do they differ in their mechanisms of action, efficacy, side effects, and ultimately, which is best for you? This detailed look will explore their individual profiles and compare their effectiveness in treating…
What is the Relationship Between Blood Type and HIV?
What is the relationship between blood type and HIV? This complex question delves into the intricate interplay between our blood types, the human immunodeficiency virus (HIV), and our immune systems. While there’s no definitive proof of a direct link between blood type and increased HIV susceptibility, research has explored potential correlations. This exploration examines various…
Unexplained Weight Loss Definition and Causes
Unexplained weight loss definition and causes: This post delves into the complexities of weight loss that happens without a clear reason. We’ll explore the definition, common medical conditions, nutritional factors, lifestyle influences, diagnostic procedures, illustrative cases, and preventative strategies. Understanding these factors can be crucial for early detection and effective treatment. The definition of unexplained…
Can I Use Topical Steroid Creams on My Face?
Can I use topical steroid creams on my face? This question is frequently asked by those experiencing facial inflammation. Understanding the benefits, risks, and alternatives is crucial for making informed decisions. Topical steroids can effectively reduce inflammation, but their use comes with potential side effects. Careful consideration and consultation with a dermatologist are essential for…
Surgery for Bowel Obstruction A Comprehensive Guide
Surgery for a bowel obstruction is a critical procedure for restoring normal bowel function when blockages prevent waste passage. This comprehensive guide delves into the intricacies of this procedure, from understanding the causes and types of obstructions to the pre-operative assessments, surgical techniques, post-operative care, and potential complications. We’ll explore the differences between mechanical and…
What are Cancer Cells A Deep Dive
What are cancer cells? They’re essentially rogue cells, out of control and wreaking havoc on the body’s delicate balance. Unlike healthy cells that follow specific instructions for growth and division, cancer cells ignore these rules, multiplying rapidly and aggressively. This relentless growth disrupts normal bodily functions, potentially leading to severe health consequences. Understanding what drives…
Esotropia Crossing of the Eyes A Comprehensive Guide
Esotropia crossing of the eyes is a condition where one or both eyes turn inward, creating a “crossed-eyes” appearance. Understanding this complex condition requires exploring its various types, from accommodative to non-accommodative, and the underlying mechanisms that cause these misalignments. This guide will delve into the causes, symptoms, diagnostic methods, treatment options, and the lasting…