Benefits of essential oils are gaining popularity, and this comprehensive guide delves into the fascinating world of these natural extracts. From their ancient uses to modern scientific research, we’ll explore their origins, properties, potential benefits, and crucial safety considerations. Understanding the diverse ways essential oils can impact our well-being requires a nuanced approach, so let’s…
What is Full Spectrum CBD? A Deep Dive
What is full spectrum CBD? It’s more than just a buzzword; it’s a complex topic encompassing plant extraction, potential benefits, and important safety considerations. This exploration delves into the intricacies of full spectrum CBD, from its definition and production methods to its potential applications and the regulations surrounding it. We’ll cover everything from the science…
The Benefits of Rutin Supplements A Deep Dive
The benefits of rutin supplements are gaining traction in health circles. This comprehensive exploration delves into the potential advantages of incorporating rutin into your daily regimen. We’ll examine its sources, forms, dosages, and potential health benefits, while also addressing potential risks and side effects. Rutin, a naturally occurring flavonoid, is found in various fruits and…
Isoflavones Benefits Side Effects, Dosage, and Interactions
Isoflavones benefits side effects dosage and interactions are a complex topic, but understanding the nuances can be key to harnessing their potential. These plant compounds, found in various foods, are gaining attention for their potential health benefits. However, it’s crucial to consider the potential side effects, appropriate dosage, and possible interactions with other substances. This…
The Benefits of Arnica A Deep Dive
The benefits of arnica, a plant with a long history of use in traditional medicine, are now being explored through a modern lens. This comprehensive exploration delves into the various forms of arnica, its purported healing properties, and the scientific evidence behind its use. From muscle soreness to joint pain, we’ll examine how arnica might…
Conjugated Linoleic Acid Weight Loss A Deep Dive
Conjugated linoleic acid weight loss is a popular topic, but understanding the science behind it is key. This post explores the potential benefits, drawbacks, and considerations surrounding CLA supplementation for weight management. We’ll delve into the science, examine different types of CLA, and look at how diet and exercise play a crucial role in achieving…
Krill vs Fish Oil A Deep Dive
Krill vs fish oil: This in-depth comparison explores the nutritional differences and potential health benefits of these popular omega-3 supplements. Krill oil, derived from tiny crustaceans, boasts unique properties, while fish oil, a familiar choice, offers a wealth of omega-3 fatty acids. Understanding the nuances of each can empower informed dietary decisions. Both krill and…
Do Fevers Cause Brain Damage? Exploring the Risks
Do fevers cause brain damage? This question is a crucial one for parents and healthcare professionals alike. While fevers are a natural part of the immune response, understanding the potential risks and protective factors is key to ensuring a healthy outcome. This blog post delves into the complex relationship between fever and brain damage, exploring…
Ozempic Novo Nordisk High Prices A Deep Dive
Ozempic Novo Nordisk high prices are a significant concern, prompting questions about affordability and accessibility. This blog post delves into the complexities surrounding this issue, examining the medication’s purpose, production costs, public perception, and potential solutions. From Novo Nordisk’s role in production to the impact on healthcare systems, we’ll explore the multifaceted factors driving these…
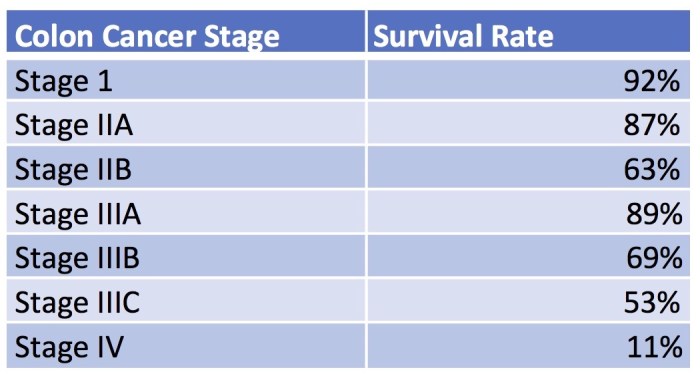
Rectal Cancer Survival Rates A Comprehensive Guide
Rectal cancer survival rates are a critical factor for patients and their families. This blog post delves into the intricacies of survival, examining factors like stage at diagnosis, treatment approaches, and even geographical influences. We’ll explore the 5-year survival rates across different stages, discuss the impact of treatment options, and analyze recent advancements in treatment….