Triple bypass surgery recovery is a journey filled with both challenges and triumphs. From pre-surgery preparations to long-term lifestyle adjustments, this guide delves into every crucial aspect of this significant procedure. We’ll explore the medical evaluations, surgical approaches, immediate post-operative care, and the essential steps for a successful recovery, including nutritional considerations, physical therapy, and…
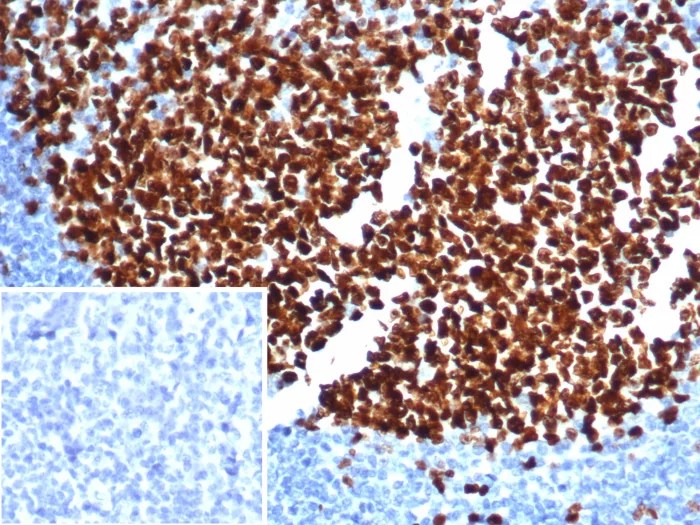
Understanding the Ki-67 Tumor Marker Test
Ki 67 tumor marker test – The Ki-67 tumor marker test is a crucial tool in oncology, providing insights into a tumor’s growth and proliferation rate. This test measures the presence of the Ki-67 protein, which is heavily associated with cell division. By understanding the different types of Ki-67 tests, their clinical applications, and the…
Chest Pain Anxiety or Panic Disorder Understanding the Link
Chest pain anxiety or panic disorder is a complex condition where anxiety and panic attacks can manifest as physical chest pain. This often leads to significant distress and uncertainty, as the symptoms can mimic those of a heart attack. It’s crucial to understand the potential overlap in symptoms, the underlying physiological mechanisms, and how to…
1 Year Old Shots A Comprehensive Guide
1 year old shots are a crucial step in your child’s development, safeguarding them against various diseases. This comprehensive guide delves into the specifics of the vaccine schedule, types, potential side effects, and essential considerations for parents. We’ll explore the reasoning behind the timing of each shot, different vaccine types, and how to manage any…
What Kind of Doctor Treats Fibromyalgia?
What kind of doctor treats fibromyalgia? This question is crucial for those navigating the complexities of this chronic condition. Understanding the various medical professionals involved in diagnosis and management can empower patients to make informed decisions about their care. From primary care physicians to specialists, and even alternative practitioners, the landscape of fibromyalgia care is…
HBsAb Hepatitis B Surface Antibody A Comprehensive Guide
HBsAb Hepatitis B surface antibody is a crucial marker in understanding immunity to hepatitis B virus (HBV). It indicates the presence of antibodies produced by the body in response to HBV infection or vaccination. Understanding HBsAb levels is vital for diagnosis, disease management, and predicting the course of the disease. This guide explores everything from…
Should My Blood Pressure Be Even After Exercise?
Should my blood pressure be even after exercise? This question sparks curiosity for anyone incorporating physical activity into their routine. Understanding how blood pressure reacts during and after exercise is crucial for maintaining overall health and well-being. We’ll delve into the normal responses, potential causes for stable readings, and when to seek medical advice. The…
Xarelto vs Eliquis Similarities and Differences Explained
Xarelto vs Eliquis similarities and differences is a crucial topic for patients and healthcare providers alike. These anticoagulants, both commonly prescribed for blood clot prevention, have key similarities and notable distinctions in their mechanisms, usage, and potential side effects. Understanding these nuances is essential for informed decision-making. This comprehensive guide delves into the intricacies of…
Why is Water So Important? A Deep Dive
Why is water so important? It’s more than just a thirst quencher; it’s fundamental to life on Earth. From sustaining our bodies to shaping our planet, water plays a crucial role in countless processes. This blog post will explore the vital importance of water in biological systems, environmental health, human well-being, agriculture, industry, and society….
Is Hypothyroidism an Autoimmune Disease?
Is hypothyroidism an autoimmune disease? This question delves into the complex relationship between the thyroid gland, the immune system, and various health conditions. Understanding this connection is crucial for diagnosis and effective management, as the answer significantly impacts treatment strategies. We’ll explore the science behind hypothyroidism, autoimmune diseases, and the specific link between them, including…