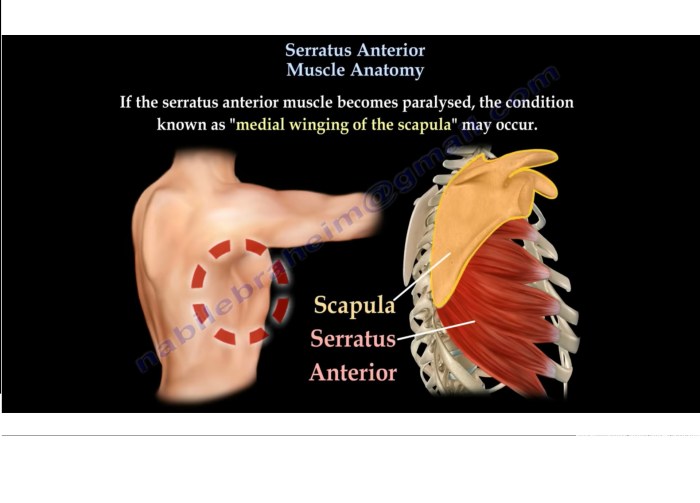
Serratus anterior muscle anatomy is crucial for understanding upper body movement. This detailed exploration delves into the muscle’s location, function, and intricate relationships with surrounding structures. We’ll examine its origin and insertion points, fiber arrangement, innervation, and blood supply, ultimately connecting these elements to its vital role in actions like pushing, reaching, and protraction. Prepare…
Fentanyl in Surgery Dosage Risks & Side Effects
Fentanyl and surgery dosage risks and side effects are a critical concern in modern surgical practice. Understanding the nuances of fentanyl use, from its role in various procedures to potential complications, is paramount. This exploration delves into the complexities of fentanyl administration, examining dosage ranges, potential adverse effects, and crucial monitoring procedures. We’ll cover the…
When Back Pain Is Serious Understanding the Signs
When back pain is serious, it’s crucial to understand the potential indicators and know when to seek immediate medical attention. This comprehensive guide delves into the various symptoms, underlying conditions, diagnostic procedures, and treatment options associated with serious back pain. We’ll explore the nuances between acute and chronic pain, red flag symptoms, and the importance…
PCOS Truths Hidden in Plain Sight
Things no one tells you about PCOS. This isn’t just about the obvious symptoms like irregular periods and acne. It’s about the hidden struggles, the emotional toll, and the often-overlooked challenges women face navigating this condition. We’ll delve into the nuances, separating fact from fiction, and sharing real experiences that shed light on the often-unseen…
Exercises for Arthritic Knees A Guide
Exercises for arthritic knees are crucial for managing pain and improving mobility. This guide provides a comprehensive overview of various exercises, tailored to different levels of knee arthritis severity. We’ll explore different types of exercises, safety precautions, and how to design a personalized program to help you stay active and comfortable. From strengthening to flexibility,…
Tardive Dyskinesia and COVID-19 A Look
Tardive dyskinesia and covid 19 – Tardive dyskinesia and COVID-19: A growing concern is emerging about the potential link between these two conditions. Tardive dyskinesia (TD) is a neurological disorder characterized by involuntary movements, often affecting the face and mouth. Understanding how COVID-19 might impact TD is crucial for healthcare professionals and patients alike. This…
Understanding Your PSA Results A Comprehensive Guide
Understanding your PSA results is crucial for prostate health. This comprehensive guide delves into what a PSA test is, how results are interpreted, and the factors that can influence them. We’ll cover everything from normal ranges and potential causes of elevated PSA to the relationship between PSA levels and prostate cancer risk, as well as…
How Long Do Short People Live? Unveiling the Truth
How long do short people live? This question delves into the complex relationship between height, health, and lifespan. While simple correlations might appear, a deeper exploration reveals the interwoven factors of genetics, environment, culture, and societal influences. The narrative explores a range of perspectives, from defining “short” across demographics and time periods to examining potential…
How to Treat an Impaled Object A Guide
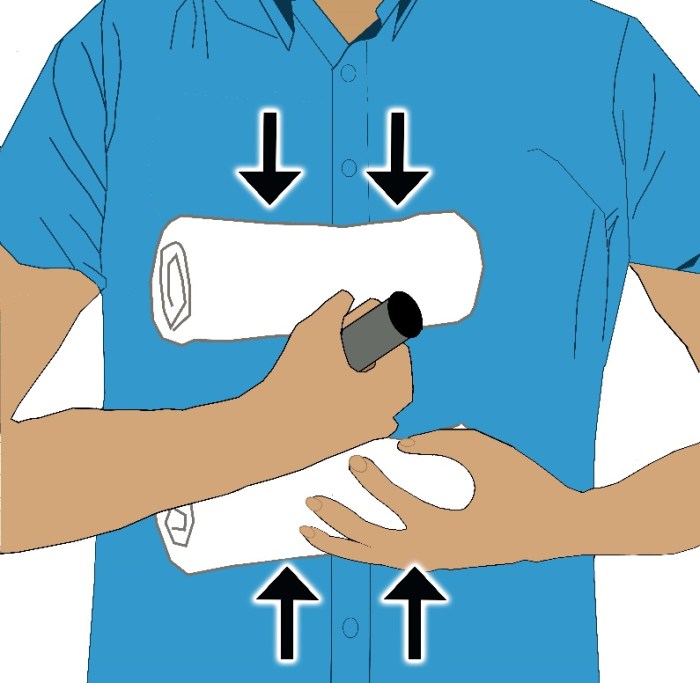
How to treat an impaled object is a critical skill to possess. This guide will walk you through the essential steps for initial assessment, stabilization, first aid, and transport, ensuring the best possible outcome for the injured person. From recognizing potential dangers to understanding specific scenarios, this comprehensive approach will empower you to handle this…
Can Receding Gums Grow Back? A Comprehensive Guide
Can receding gums grow back? This question sets the stage for a fascinating exploration into the world of gum health. We’ll delve into the causes, treatments, and long-term management strategies for receding gums, providing insights into the potential for regrowth and overall gum health. Understanding the factors that contribute to gum recession, from genetics to…