Bronchitis asthma types symptoms are a common respiratory issue that affects many people. This in-depth guide will explore the different types of bronchitis and asthma, their common symptoms, how they’re diagnosed, and how they’re treated. We’ll also cover preventative measures and lifestyle recommendations to help manage these conditions.
Understanding the differences between acute and chronic bronchitis, and the various types of asthma (like allergic, non-allergic, and exercise-induced) is crucial for effective management. This guide aims to provide a clear overview of each aspect, from the initial onset to long-term care. We’ll examine how symptoms can vary and why accurate diagnosis is vital.
Introduction to Bronchitis and Asthma: Bronchitis Asthma Types Symptoms
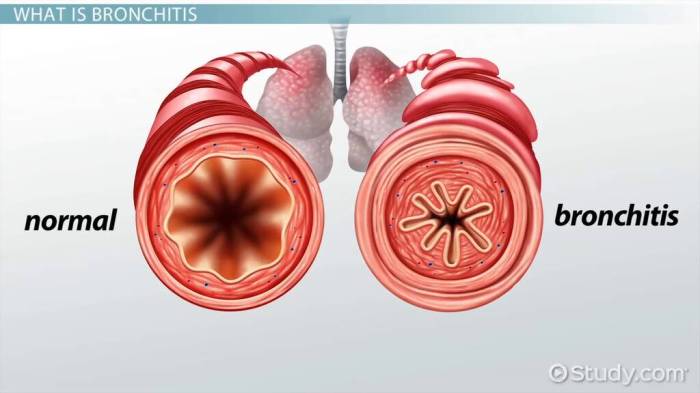
Bronchitis and asthma are both respiratory conditions that cause inflammation and narrowing of the airways, leading to breathing difficulties. While both affect the lungs, they differ significantly in their underlying causes, symptoms, and treatment approaches. Understanding these differences is crucial for accurate diagnosis and effective management.These conditions often coexist or are misdiagnosed, so distinguishing between bronchitis and asthma is essential for appropriate medical interventions.
Understanding the different types of bronchitis and asthma, and their associated symptoms, is crucial for managing these conditions effectively. Knowing the various presentations of these respiratory issues can help you determine the best course of action, and before you buy allegra, it’s important to consult with a healthcare professional. They can help you understand if it’s the right medication for your specific needs and symptoms, especially when dealing with bronchitis or asthma.
Ultimately, staying informed about these conditions is key to managing your health.
Early diagnosis and personalized treatment plans are critical to minimizing long-term complications and improving quality of life.
Defining Bronchitis and Asthma
Bronchitis is characterized by inflammation of the bronchial tubes, the airways that carry air to and from the lungs. Asthma, on the other hand, is a chronic inflammatory disorder of the airways, causing recurring episodes of wheezing, breathlessness, chest tightness, and coughing. The key difference lies in the underlying cause and the nature of the airway response.
Common Causes and Risk Factors
Several factors can contribute to the development of bronchitis and asthma. Infections, particularly viral infections like the common cold or flu, are frequent triggers for bronchitis. Exposure to irritants such as smoke, dust, and chemical fumes can also exacerbate bronchitis and increase the risk of developing it. Asthma triggers are diverse and include allergens like pollen, pet dander, and mold; respiratory infections; and environmental factors like air pollution and exercise.
Individuals with a family history of asthma or allergies are at a higher risk of developing the condition.
Onset and Progression
Bronchitis can manifest acutely, often following a viral infection, or develop into a chronic condition in individuals exposed to persistent irritants. Acute bronchitis typically resolves within a few weeks with supportive care. Chronic bronchitis, however, is characterized by persistent inflammation and coughing, often associated with long-term exposure to irritants. Asthma, similarly, can have acute episodes triggered by various factors, or progress into a chronic condition characterized by recurring symptoms and varying degrees of airway narrowing.
The severity and frequency of asthma attacks can fluctuate over time, influenced by environmental factors and triggers.
Key Differences Between Bronchitis and Asthma
| Characteristic | Bronchitis | Asthma |
|---|---|---|
| Definition | Inflammation of the bronchial tubes, often triggered by infection. | Chronic inflammatory disorder of the airways, causing recurring episodes of airway narrowing. |
| Causes | Viral infections, exposure to irritants (smoke, dust, chemicals). | Allergies, respiratory infections, environmental factors (air pollution, exercise). |
| Symptoms | Cough (often productive, with mucus), chest discomfort, shortness of breath. | Wheezing, breathlessness, chest tightness, coughing. |
| Treatment | Rest, fluids, over-the-counter medications to relieve symptoms. In severe cases, antibiotics or other medications. | Inhaled bronchodilators, corticosteroids, and other medications to control inflammation and open airways. Avoidance of triggers is crucial. |
| Chronic form | Chronic bronchitis is possible with persistent exposure to irritants, characterized by chronic cough and mucus production. | Asthma can become chronic with recurring episodes of airway narrowing. |
Types of Bronchitis and Asthma
Understanding the different types of bronchitis and asthma is crucial for effective diagnosis and treatment. Knowing the specific type can help pinpoint the underlying causes, predict potential complications, and tailor management strategies. This deeper understanding allows for more targeted interventions and improved long-term outcomes.
Types of Bronchitis
Bronchitis encompasses various forms, each with unique characteristics. Recognizing these distinctions helps healthcare professionals in their assessment and treatment planning.
Acute bronchitis is a common, often self-limiting inflammation of the bronchial tubes. It typically arises from viral infections, such as influenza or the common cold. Symptoms generally manifest as a cough, which may produce mucus, and may include chest discomfort, shortness of breath, and fever.
Chronic bronchitis, on the other hand, is a persistent cough that produces mucus over a prolonged period, typically at least three months a year for two consecutive years. This condition is frequently linked to long-term exposure to irritants like cigarette smoke, air pollution, or industrial dust. Chronic bronchitis can lead to significant respiratory complications.
Bronchiolitis is a specific type of bronchitis that primarily affects infants and young children. It’s characterized by inflammation and narrowing of the bronchioles, the smallest air passages in the lungs. Respiratory syncytial virus (RSV) is a frequent culprit behind bronchiolitis. Symptoms include rapid breathing, wheezing, and difficulty breathing.
Types of Asthma
Asthma, a chronic respiratory condition, manifests in diverse forms. Understanding these variations is key to appropriate treatment.
Allergic asthma is triggered by specific allergens, such as pollen, pet dander, or dust mites. Exposure to these allergens can stimulate an immune response, leading to inflammation and narrowing of the airways. Symptoms often include wheezing, coughing, and shortness of breath.
Non-allergic asthma, as the name suggests, is not linked to allergic reactions. Triggers for this type can include respiratory infections, exercise, cold air, stress, or certain medications. Symptoms may overlap with allergic asthma, presenting as wheezing, chest tightness, and shortness of breath.
Exercise-induced asthma is a specific form of non-allergic asthma triggered by physical exertion. The increased breathing rate and volume during exercise can cause airway narrowing, resulting in wheezing and shortness of breath. This typically resolves after exercise ceases.
Occupational asthma is triggered by specific substances or irritants encountered in the workplace. Exposure to these substances can lead to chronic inflammation and narrowing of the airways, causing symptoms such as wheezing, coughing, and shortness of breath.
Comparison of Bronchitis and Asthma Types
| Type | Triggers | Treatments | Long-Term Effects |
|---|---|---|---|
| Acute Bronchitis | Viral infections, irritants | Rest, fluids, over-the-counter medications for symptom relief | Usually resolves without long-term effects. Potential for complications in individuals with underlying health conditions. |
| Chronic Bronchitis | Smoking, air pollution, industrial dust | Smoking cessation, bronchodilators, inhaled corticosteroids, pulmonary rehabilitation | Increased risk of respiratory infections, chronic lung disease (COPD), and heart problems. |
| Bronchiolitis | Respiratory viruses (e.g., RSV) | Supportive care, hydration, oxygen therapy (in severe cases) | Can lead to complications like pneumonia. Infants and young children are particularly vulnerable. |
| Allergic Asthma | Pollen, pet dander, dust mites | Allergen avoidance, medications (inhaled corticosteroids, bronchodilators), immunotherapy | Chronic airway inflammation, increased risk of exacerbations, and potential for permanent lung damage. |
| Non-allergic Asthma | Respiratory infections, exercise, cold air, stress, certain medications | Medications (inhaled corticosteroids, bronchodilators), avoidance of triggers | Chronic airway inflammation, increased risk of exacerbations, and potential for permanent lung damage. |
| Exercise-induced Asthma | Physical exertion | Warm-up before exercise, bronchodilators before exercise | Can limit physical activity. Effective management can allow for continued participation in physical activities. |
| Occupational Asthma | Workplace irritants and substances | Avoiding workplace triggers, medications, and sometimes a change in employment | Chronic airway inflammation, potential for permanent lung damage. |
Symptoms of Bronchitis and Asthma
Understanding the symptoms of bronchitis and asthma is crucial for early diagnosis and effective management. Both conditions affect the airways, leading to inflammation and narrowing, but the specific symptoms can differ. Recognizing these differences can help distinguish between the two and guide appropriate treatment.Recognizing the symptoms of bronchitis and asthma is essential for timely intervention. Different symptoms manifest at various severity levels, impacting daily life.
This section will delve into the common symptoms associated with each condition, emphasizing variations based on severity and type.
Common Symptoms of Bronchitis
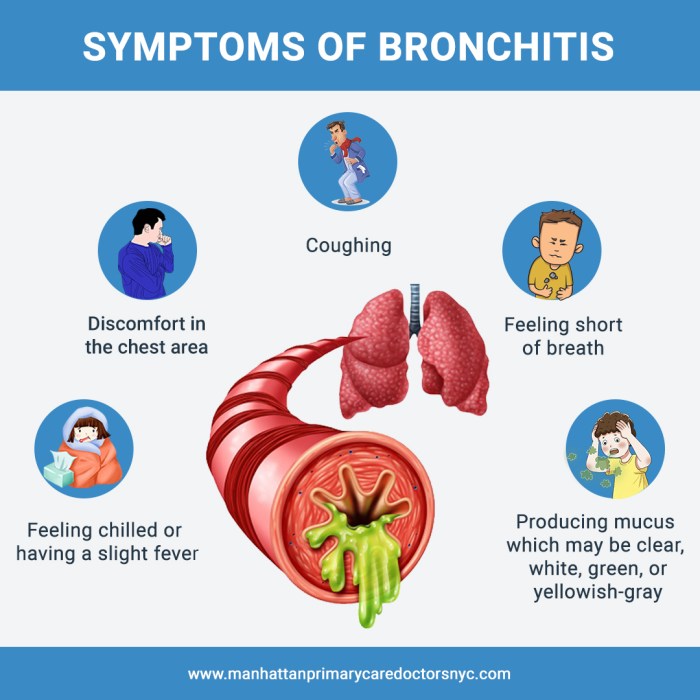
Bronchitis, characterized by inflammation of the bronchial tubes, often presents with a persistent cough as a primary symptom. This cough, frequently productive, means it produces mucus. The mucus can vary in color, from clear to yellow or green, depending on the underlying cause. Other common symptoms include chest tightness, shortness of breath, and a feeling of discomfort in the chest.
These symptoms can range from mild to severe, impacting an individual’s ability to perform daily tasks.
- Cough: A persistent cough, often productive (meaning it produces mucus), is a hallmark of bronchitis. The cough can be dry initially, then become productive as the condition progresses. The color of the mucus can range from clear to yellow or green, depending on the cause of the infection.
- Mucus Production: The production of mucus is a key symptom of bronchitis. The mucus can vary in color and consistency. Clear mucus might indicate a viral infection, while yellow or green mucus often suggests a bacterial infection.
- Chest Tightness: A feeling of tightness or pressure in the chest can accompany bronchitis. This discomfort can be mild or severe, depending on the inflammation levels.
- Shortness of Breath: Difficulty breathing, or shortness of breath, is another possible symptom of bronchitis, particularly during exertion. The severity of shortness of breath can vary significantly depending on the individual and the extent of the inflammation.
Common Symptoms of Asthma
Asthma, a chronic inflammatory disorder of the airways, typically presents with wheezing, a characteristic whistling sound during breathing. Shortness of breath is also a prominent symptom, often triggered by exertion or exposure to allergens. Chest tightness is another frequent symptom, making breathing difficult. Coughing, especially at night, is a common symptom for many individuals with asthma.
- Wheezing: Wheezing, a whistling sound during breathing, is a common and recognizable symptom of asthma. The wheezing can range from mild to severe, depending on the severity of the asthma attack.
- Shortness of Breath: Difficulty breathing, or shortness of breath, is a prominent symptom of asthma. This symptom can be triggered by exertion, allergens, or other asthma triggers.
- Chest Tightness: A feeling of tightness or pressure in the chest is a frequent symptom of asthma. This discomfort can make breathing challenging.
- Coughing (especially at night): A persistent cough, particularly at night, is a common symptom of asthma. The cough may be dry or produce mucus. Nighttime coughing is often associated with airway inflammation and narrowing.
Comparison of Bronchitis and Asthma Symptoms
While both bronchitis and asthma affect the airways, their symptoms can overlap. Both conditions can cause coughing, shortness of breath, and chest tightness. However, wheezing is a more distinctive symptom of asthma, while a productive cough (producing mucus) is more characteristic of bronchitis.
“The key to differentiating between bronchitis and asthma lies in the presence of wheezing and the presence or absence of mucus production.”
Symptom Variation Based on Severity
The severity of symptoms can vary significantly based on the type and severity of the condition. Mild cases might present with only a slight cough or shortness of breath, while severe cases can lead to significant breathing difficulties. This variation is important for recognizing and managing the condition appropriately.
Symptom Summary Table
| Symptom | Bronchitis (Mild) | Bronchitis (Moderate) | Bronchitis (Severe) | Asthma (Mild) | Asthma (Moderate) | Asthma (Severe) |
|---|---|---|---|---|---|---|
| Cough | Occasional | Frequent | Persistent | Occasional | Frequent | Persistent |
| Mucus Production | Minimal | Moderate | Significant | Absent | Absent | Absent |
| Wheezing | Absent | Absent | Absent | Occasional | Frequent | Persistent |
| Shortness of Breath | Mild | Moderate | Severe | Mild | Moderate | Severe |
| Chest Tightness | Mild | Moderate | Severe | Mild | Moderate | Severe |
Diagnosing Bronchitis and Asthma
Accurately diagnosing bronchitis and asthma is crucial for effective treatment and management. These conditions, while distinct, can share overlapping symptoms, making differentiation challenging. Proper diagnosis relies on a combination of patient history, physical examination, and specific diagnostic tests.Differentiating between bronchitis and asthma often hinges on identifying the underlying causes and patterns of symptoms. Understanding the diagnostic process empowers both patients and healthcare professionals to make informed decisions regarding treatment strategies.
Physical Examination and Medical History Review
A thorough physical examination is a vital initial step in diagnosing bronchitis and asthma. The physician will assess the patient’s overall condition, listen to their lungs using a stethoscope (auscultation), and evaluate their breathing patterns. This process helps identify signs indicative of inflammation or obstruction in the airways. A review of the patient’s medical history, including previous respiratory illnesses, allergies, and family history of respiratory conditions, provides valuable context for understanding the current presentation.
Understanding bronchitis and asthma types and their symptoms is crucial for effective management. While exploring the complexities of these respiratory conditions, it’s interesting to note the recent progress being made in anti-obesity drugs, which can significantly impact the management of co-morbidities like asthma. This progress in progress of anti obesity drugs could lead to better outcomes for individuals with bronchitis and asthma, as obesity is often a contributing factor to the severity of these conditions.
Ultimately, a holistic approach encompassing various treatments and lifestyle modifications is key to managing these conditions effectively.
The medical history also helps pinpoint potential triggers or risk factors associated with the patient’s symptoms.
Diagnostic Procedures for Bronchitis
The diagnostic approach for bronchitis typically focuses on identifying the cause and confirming the presence of inflammation in the airways. This often involves:
- Review of symptoms: A detailed account of the patient’s symptoms, including the duration, severity, and accompanying symptoms (e.g., fever, cough, sputum production) aids in determining the likely cause and the appropriate diagnostic path.
- Physical examination: Auscultation, or listening to the lungs with a stethoscope, reveals characteristic sounds indicative of inflammation, such as wheezing or crackles. The presence of other findings, such as fever or chest pain, can provide additional clues.
- Imaging tests (optional): In some cases, chest X-rays might be necessary to rule out other conditions or assess the extent of inflammation. This is particularly important if complications are suspected or the diagnosis is uncertain. An X-ray can help distinguish bronchitis from other conditions that may present with similar symptoms.
Diagnostic Procedures for Asthma
Diagnosing asthma involves a more comprehensive approach, considering potential triggers and the patient’s response to various stimuli. Key procedures include:
- Lung function tests (spirometry): Spirometry measures the volume and flow of air in and out of the lungs. This test helps identify airway obstruction and assess the degree of airflow limitation, which is a hallmark of asthma. A decrease in airflow, particularly during forced exhalation, suggests airway narrowing.
- Allergy testing: If allergies are suspected, allergy testing (skin prick tests or blood tests) can identify specific allergens that might trigger asthma symptoms. This helps in identifying potential triggers and tailoring management strategies.
- Peak flow monitoring: This involves using a peak flow meter to track the patient’s ability to exhale air forcefully. This is a valuable tool for monitoring asthma symptoms and response to treatment, as well as to detect periods of exacerbation.
- Medical history review: A thorough review of the patient’s medical history, including previous respiratory illnesses, family history of asthma, and any known allergies, is crucial to understand the context of the current presentation.
Overlapping Symptoms and Differentiation
Bronchitis and asthma can exhibit similar symptoms, particularly cough and shortness of breath. This overlap complicates diagnosis. Healthcare professionals use a combination of factors to differentiate between the two conditions:
- Symptom duration: Bronchitis typically presents with symptoms lasting a few weeks, while asthma can manifest as intermittent episodes.
- Presence of triggers: Asthma symptoms often respond to specific triggers like allergens or exercise, while bronchitis is less frequently associated with these specific triggers.
- Response to treatment: Asthma typically responds well to bronchodilators, while bronchitis may not.
Step-by-Step Diagnostic Process
A typical diagnostic process involves these steps:
- Detailed patient history collection, including symptom duration, frequency, and potential triggers.
- Thorough physical examination, including auscultation of the lungs.
- Lung function tests (spirometry) to assess airflow obstruction.
- Allergy testing if allergies are suspected.
- Imaging tests (e.g., chest X-ray) to rule out other conditions.
- Monitoring of symptoms and response to treatment to track the effectiveness of interventions.
Treatment and Management of Bronchitis and Asthma
Managing bronchitis and asthma effectively involves a multifaceted approach that prioritizes symptom relief, prevention, and overall health. Understanding the specific treatments for each condition, and recognizing the importance of personalized care, is crucial for successful management. Effective treatment plans often combine medication with lifestyle modifications, tailored to individual needs and triggers.Effective treatment for bronchitis and asthma requires a comprehensive understanding of the underlying causes and contributing factors.
Addressing the root causes, combined with appropriate medication and lifestyle changes, leads to better outcomes. This approach fosters long-term well-being and reduces the frequency and severity of episodes.
Common Bronchitis Treatments
Bronchitis treatments typically focus on alleviating symptoms and supporting the body’s natural healing process. Rest and hydration are fundamental to recovery. Adequate rest allows the body to dedicate energy to fighting the infection, while sufficient fluids help thin mucus and facilitate its removal.
- Rest: Sufficient rest is essential for allowing the body to heal and recover from bronchitis. This includes avoiding strenuous activities and prioritizing sleep to promote healing.
- Fluids: Drinking plenty of fluids, such as water, herbal teas, or clear broths, helps thin mucus and reduce congestion. This facilitates easier breathing and reduces discomfort.
- Over-the-Counter Medications: Over-the-counter medications like cough suppressants, decongestants, and pain relievers can provide symptomatic relief. However, it’s crucial to follow dosage instructions carefully and consult a healthcare professional if symptoms worsen or persist.
Common Asthma Treatments
Asthma treatments aim to manage and control inflammation in the airways, preventing exacerbations and improving breathing. Different medications are often used in combination to achieve optimal control.
Understanding bronchitis and asthma symptoms can be tricky, with various types affecting individuals differently. While exploring these respiratory conditions, it’s important to remember that other digestive issues, like IBS, can also significantly impact quality of life. For example, learning more about IBS, specifically the alternating type known as IBS-A, might offer a better understanding of the interplay between different body systems.
IBS-A, alternating type irritable bowel syndrome can manifest in a variety of ways, just as bronchitis and asthma symptoms do. Ultimately, a holistic approach to health considers how various systems connect, and focusing on comprehensive symptom analysis remains crucial for effective management of respiratory conditions like bronchitis and asthma.
- Inhaled Corticosteroids: These medications are crucial in reducing inflammation in the airways, preventing the narrowing of airways, and reducing the frequency of asthma attacks. They are typically the cornerstone of long-term asthma management.
- Bronchodilators: These medications quickly relax the muscles around the airways, opening them up and easing breathing. They are often used as quick-relief medications to alleviate sudden attacks. Short-acting bronchodilators are used for immediate relief, while long-acting bronchodilators help control symptoms over a longer period.
- Other Medications: Other medications, such as leukotriene modifiers and theophylline, can also be part of an asthma treatment plan. Their role is often supplementary to inhaled corticosteroids and bronchodilators, targeting specific inflammatory pathways.
Comparing and Contrasting Treatments
While both conditions involve respiratory issues, the treatment approaches differ significantly. Bronchitis typically involves supportive care to help the body fight off an infection, while asthma management emphasizes controlling inflammation and preventing exacerbations. Individualized care is paramount. Factors such as age, severity of symptoms, and underlying health conditions influence treatment decisions.
Preventive Measures
Preventing bronchitis and asthma exacerbations is crucial. Avoiding triggers and maintaining a healthy lifestyle are key strategies.
- Avoiding Triggers: Identifying and avoiding triggers, such as allergens (pollen, dust mites), irritants (smoke, strong odors), and environmental factors, is vital. This can significantly reduce the frequency and severity of episodes.
- Maintaining a Healthy Lifestyle: A balanced diet, regular exercise, and adequate sleep contribute to overall health and a stronger immune system. These factors play a crucial role in preventing respiratory illnesses and managing their impact.
Treatment Comparison Table
| Feature | Bronchitis | Asthma |
|---|---|---|
| Primary Goal | Symptom relief and infection resolution | Inflammation control and prevention of exacerbations |
| Common Medications | Cough suppressants, decongestants, pain relievers | Inhaled corticosteroids, bronchodilators, leukotriene modifiers, theophylline |
| Lifestyle Modifications | Rest, fluids, avoiding irritants | Avoiding triggers, maintaining a healthy lifestyle |
Prevention and Lifestyle Recommendations
Protecting your respiratory health from bronchitis and asthma involves proactive steps and mindful lifestyle choices. A combination of environmental controls, healthy habits, and trigger avoidance significantly reduces the risk of developing these conditions and managing symptoms effectively. By understanding the factors contributing to these respiratory illnesses, you can empower yourself to take control of your health.Adopting preventative measures is crucial for both preventing the onset of bronchitis and asthma, as well as managing existing conditions.
Lifestyle choices play a vital role in reducing inflammation and improving overall respiratory function. Proactive steps to mitigate triggers and allergens are critical in preventing asthma attacks. These strategies promote a healthier respiratory system, contributing to a better quality of life.
Preventive Measures to Reduce Bronchitis and Asthma Risk
Preventive measures are essential for minimizing the risk of developing bronchitis and asthma. These strategies target environmental factors, lifestyle choices, and the management of triggers and allergens. By proactively addressing these factors, individuals can significantly reduce their risk of developing these respiratory conditions.
- Avoidance of Respiratory Irritants: Exposure to smoke (cigarette, environmental), dust, fumes, and chemical irritants can trigger bronchitis and asthma. Strategies include avoiding smoke-filled environments, using appropriate respiratory protection when working with irritants, and maintaining a clean and well-ventilated home or workplace. Proper ventilation and air filtration systems are particularly important in environments with high levels of pollutants.
- Healthy Diet and Hydration: A balanced diet rich in fruits, vegetables, and whole grains, coupled with adequate hydration, supports overall health and strengthens the immune system, which is vital in defending against respiratory infections.
- Regular Exercise: Physical activity improves lung function and strengthens the cardiovascular system, bolstering the body’s ability to fight off infections and maintain respiratory health. Regular exercise is an essential component of a preventative strategy for both bronchitis and asthma.
- Stress Management: Chronic stress can weaken the immune system, making individuals more susceptible to respiratory infections. Stress-reduction techniques, such as meditation, yoga, or spending time in nature, can be helpful in mitigating this risk factor.
Role of Lifestyle Choices in Managing Bronchitis and Asthma
Lifestyle choices significantly influence the management and prevention of bronchitis and asthma. The impact of diet, exercise, and stress management on respiratory health is profound. Consistent healthy habits contribute to improved lung function and a stronger immune system, making individuals better equipped to manage symptoms.
- Vaccinations: Staying up-to-date with vaccinations, especially the flu and pneumonia vaccines, can help prevent respiratory infections that can exacerbate bronchitis and asthma symptoms. These vaccinations are an essential preventative measure against potential triggers.
- Allergen Avoidance: Identifying and avoiding allergens is critical for preventing asthma attacks. This may involve minimizing exposure to dust mites, pet dander, pollen, or mold. Creating a hypoallergenic environment is crucial in preventing asthma triggers.
- Proper Sleep Hygiene: Adequate sleep allows the body to repair and regenerate, contributing to a healthier immune response and improved respiratory function. A regular sleep schedule and a relaxing bedtime routine can significantly improve overall health.
Maintaining a Healthy Respiratory System
Maintaining a healthy respiratory system is a key component of preventative care. This involves understanding and addressing potential triggers, fostering healthy habits, and proactively supporting the respiratory system. A strong respiratory system is better equipped to manage and prevent respiratory conditions.
| Preventive Lifestyle Measure | Actionable Steps |
|---|---|
| Air Quality Control | Regularly clean and maintain HVAC systems. Use air purifiers in areas with high pollution. Avoid exposure to smoke, dust, and chemical irritants. |
| Nutrition | Consume a balanced diet rich in fruits, vegetables, and whole grains. Stay hydrated by drinking plenty of water. |
| Exercise | Engage in regular physical activity, such as brisk walking, jogging, or swimming. Consult with a healthcare professional before starting a new exercise regimen. |
| Stress Management | Practice stress-reducing techniques, such as meditation, yoga, or deep breathing exercises. Prioritize relaxation and mental well-being. |
Illustrations and Visual Aids
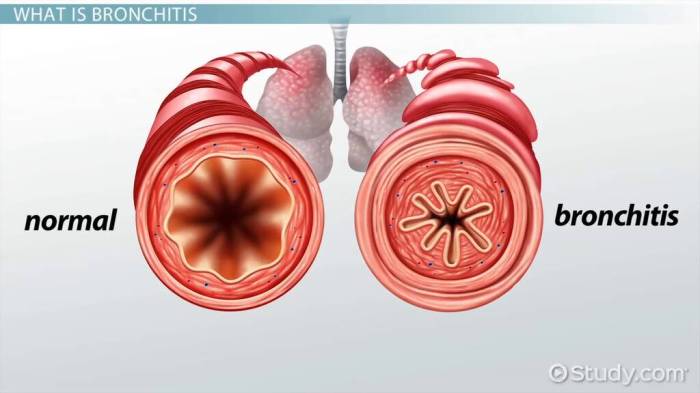
Visual aids are crucial for understanding complex medical conditions like bronchitis and asthma. They transform abstract concepts into tangible representations, making it easier to grasp the intricacies of the respiratory system, triggers, diagnostic processes, and treatment methods. These visual tools can enhance patient education and support better communication between healthcare professionals and patients.
Respiratory System Anatomy
A diagram of the respiratory system is essential for understanding the location of the bronchi and lungs. The diagram should clearly illustrate the trachea branching into the left and right bronchi, leading to the lungs. The bronchi should be highlighted, showcasing their branching structure within the lungs, and the delicate alveoli where gas exchange occurs should be depicted.
This visualization aids in understanding how air flows through the system and the potential sites of obstruction in bronchitis and asthma. The diagram should include labels for key structures, including the nasal cavity, pharynx, larynx, trachea, bronchi, bronchioles, and alveoli.
Asthma Triggers
Visualizing asthma triggers can be helpful for both patients and healthcare professionals. A graphic representation can display common triggers, such as allergens (pollen, dust mites, pet dander, mold), exercise, respiratory infections (colds, flu), and environmental factors (air pollution, smoke). The graphic can use icons or symbols to represent each trigger, categorized for easy identification. The visual representation can also include information about the intensity of the response each trigger may provoke.
Diagnostic Flowchart, Bronchitis asthma types symptoms
A flowchart illustrating the diagnostic process for bronchitis and asthma can greatly aid in understanding the steps involved. The flowchart should begin with initial symptoms and progressively follow the diagnostic steps, such as physical examination, medical history, pulmonary function tests (PFTs), chest X-rays, and allergy testing. Each step should be clearly represented by boxes or shapes connected by arrows, showing the logical progression of the diagnosis.
For instance, the flowchart should demonstrate how certain symptoms or test results might lead to further investigations or alternative diagnoses.
Inhaler Types
An image showcasing different types of inhalers used in asthma treatment should illustrate their various functions and usage. The image could include metered-dose inhalers (MDIs), dry powder inhalers (DPIs), and nebulizers. Each type of inhaler should be labeled, and the image should visually depict how to use the device correctly, highlighting the proper inhalation technique. For instance, the image could show how to activate the MDI or how to load the DPI with medication.
It should also indicate the intended use of each type of inhaler.
Medication Effects on Lung Function
A graph illustrating the effects of medication on lung function can be highly informative. The graph should display lung function measurements (e.g., forced expiratory volume in one second, or FEV1) over time, both before and after the administration of medication. The x-axis should represent time (e.g., days or weeks), and the y-axis should represent the lung function values.
The graph should clearly show the improvement in lung function after the administration of medication, providing concrete evidence of its effectiveness. The graph can include error bars to indicate the variability in lung function measurements. An example could depict a patient with asthma whose FEV1 improves significantly after using an inhaled corticosteroid.
Closing Notes
In conclusion, bronchitis and asthma, while sharing some overlapping symptoms, are distinct conditions with varying causes, types, and treatments. This guide has provided a comprehensive overview of these respiratory issues, from their definitions to their management. By understanding the intricacies of each, you can better equip yourself or a loved one with the knowledge needed to navigate the complexities of these conditions.