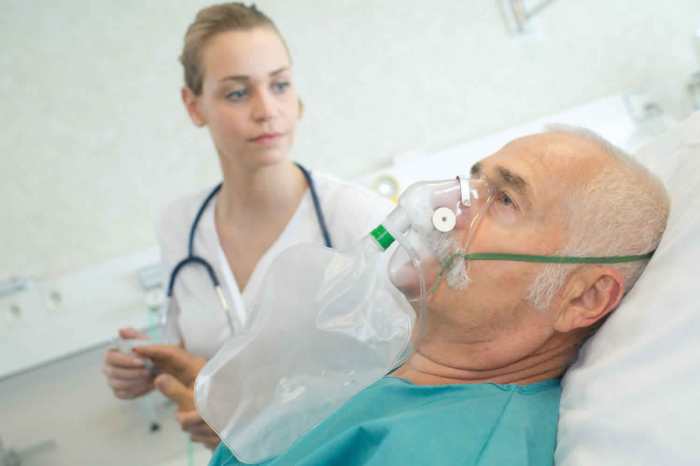
Bendopnea a new symptom of heart failure – Bendopnea, a new symptom of heart failure, describes a specific type of shortness of breath that occurs when bending over. This distinct respiratory response, different from typical dyspnea, may indicate underlying heart conditions. Understanding its characteristics, physiological mechanisms, and clinical presentation is crucial for accurate diagnosis and effective management of heart failure.
This article explores the intricacies of bendopnea, delving into its defining characteristics, potential physiological mechanisms, clinical presentation, diagnostic considerations, and treatment strategies. We will examine the role of fluid accumulation in the lungs, the impact of cardiac output and blood pressure, and the importance of distinguishing bendopnea from other respiratory conditions.
Defining Bendopnea
Bendopnea, a newly recognized symptom of heart failure, presents a unique challenge in diagnosis and management. Understanding its distinct characteristics, how it differs from other respiratory symptoms, and potential triggers is crucial for healthcare professionals and individuals experiencing this condition. This post aims to provide a comprehensive overview of bendopnea.
Definition of Bendopnea
Bendopnea is characterized by shortness of breath or dyspnea that is specifically triggered or exacerbated by bending over or assuming a flexed posture. It’s important to differentiate this from other respiratory symptoms like dyspnea at rest, which is a general feeling of shortness of breath not directly linked to body position. Bendopnea is a symptom tied to the specific mechanics of bending and the impact on cardiovascular function in individuals with heart failure.
Distinguishing Bendopnea from Other Respiratory Symptoms, Bendopnea a new symptom of heart failure
Bendopnea is distinct from other respiratory symptoms, primarily due to its posture-dependent nature. While general dyspnea can arise from various causes, bendopnea is uniquely linked to the increased hydrostatic pressure in the chest cavity when bending. This pressure difference affects the return of blood to the heart, thus impacting breathing capacity. The difference lies in the specific triggering mechanism and the immediate response.
Typical Characteristics of Bendopnea
Bendopnea typically presents with a gradual onset, often noticeable as the individual bends forward. The duration can vary, from a few seconds to several minutes, depending on the severity of the heart failure and the degree of bending. The intensity of bendopnea can also range, from a mild discomfort to a severe and incapacitating feeling of breathlessness.
Potential Triggers and Factors Associated with Bendopnea
Several factors can potentially trigger or exacerbate bendopnea. These include activities that involve bending, such as stooping, lifting heavy objects, or even prolonged periods of standing. In addition, factors like exertion, certain medications, and changes in posture all can influence the severity and frequency of bendopnea.
Key Differences Between Bendopnea and Dyspnea
| Characteristic | Bendopnea | Dyspnea |
|---|---|---|
| Trigger | Bending, assuming a flexed posture | Various factors (e.g., exertion, anxiety, underlying disease) |
| Onset | Gradual, often noticeable during or shortly after bending | Sudden or gradual, can occur at rest or during exertion |
| Duration | Variable, from seconds to minutes | Variable, from seconds to hours |
| Intensity | Ranges from mild discomfort to severe breathlessness | Ranges from mild discomfort to severe breathlessness |
| Associated Factors | Heart failure, increased hydrostatic pressure in the chest cavity | Many potential underlying conditions |
Physiological Mechanisms
Bendopnea, the symptom of shortness of breath triggered by bending, presents a unique challenge in understanding heart failure’s impact on respiratory function. While a common symptom like shortness of breath might be associated with various underlying conditions, the specific link between bending and breathing difficulties in heart failure is a crucial area of investigation. This section delves into the potential physiological mechanisms driving this symptom.The physiological underpinnings of bendopnea in heart failure stem from a complex interplay of factors, primarily related to fluid accumulation in the lungs and the impact on the cardiovascular system’s efficiency.
Bendopnea, a newly recognized symptom of heart failure, is characterized by shortness of breath that worsens when bending over. This can often be mistaken for other conditions. Doctors are now exploring diagnostic tools like the straight leg raise test to help differentiate between bendopnea and other causes of pain and discomfort. Ultimately, understanding the nuances of bendopnea is crucial for accurate diagnosis and effective treatment of heart failure.
Understanding these mechanisms is crucial for accurate diagnosis and effective treatment strategies.
Fluid Accumulation in the Lungs
Fluid buildup in the lungs, a hallmark of heart failure, directly affects breathing mechanics. When the heart struggles to pump blood efficiently, fluid can leak into the alveoli, the tiny air sacs in the lungs. This fluid accumulation hinders the exchange of oxygen and carbon dioxide, leading to shortness of breath. The increased weight of the fluid in the lungs, especially during bending, creates resistance against expansion, thus exacerbating breathing difficulties.
Gravity plays a significant role in this process, as fluid tends to pool in the lower parts of the lungs, particularly when in a bent position. This pooling effect is further intensified in individuals with heart failure.
Cardiac Output and Blood Pressure
Cardiac output, the volume of blood pumped by the heart per minute, directly impacts blood flow to the lungs. In heart failure, a reduced cardiac output results in decreased blood flow to the lungs, potentially impacting the efficient exchange of gases. Furthermore, alterations in blood pressure can affect the hydrostatic pressure within the pulmonary capillaries, influencing fluid movement and accumulation in the lungs.
Reduced cardiac output and low blood pressure, particularly during bending, can cause a further reduction in blood flow to the lungs and increase the chances of fluid build-up in the lungs, contributing to bendopnea.
Chest Wall Compliance
Heart failure can also impact chest wall compliance, the ability of the chest wall to expand and contract. Fluid buildup and the resulting pressure in the lungs can affect the mechanics of breathing. In heart failure, the stiffening of the chest wall may increase the effort required for breathing, particularly during bending, when the increased pressure on the diaphragm might make it harder to fully expand the lungs.
Comparison of Bending Effects
The physiological effects of bending differ significantly between individuals with and without heart failure. In healthy individuals, bending minimally affects breathing mechanics. The cardiovascular system efficiently adjusts to the postural change. However, in individuals with heart failure, bending exacerbates the pre-existing fluid accumulation in the lungs, leading to a more pronounced shortness of breath.
Correlation Between Bending and Lung Filling
| Posture | Lung Filling (Individuals with Heart Failure) | Lung Filling (Healthy Individuals) |
|---|---|---|
| Upright | Moderate fluid accumulation, but tolerable breathing | Minimal fluid accumulation, effortless breathing |
| Bent Forward | Increased fluid accumulation in the lower lung fields, significantly impacting breathing | Minimal change in lung filling, no significant impact on breathing |
This table highlights the distinct differences in lung filling and breathing mechanics between individuals with and without heart failure during bending. The increased fluid accumulation in the lower lung fields of individuals with heart failure during bending directly correlates with the symptom of bendopnea.
Clinical Presentation
Bendopnea, the symptom of shortness of breath triggered by bending, presents a unique diagnostic challenge in heart failure patients. Its subtle nature and potential overlap with other respiratory conditions can lead to delayed or missed diagnoses. Understanding the clinical presentation is crucial for accurate identification and prompt management.
Scenarios of Bendopnea Observation
Bendopnea can manifest in various situations where patients with heart failure adopt a bent posture. For example, it might be observed during tasks like stooping to pick up an object, gardening, or performing household chores. It can also occur during activities that involve prolonged bending, such as prolonged work or exercise that requires bending.
Bendopnea, a newly identified symptom of heart failure, is intriguing. It’s a fascinating development in understanding this condition, but diet plays a significant role. Foods high in saturated fats and processed sugars can contribute to inflammation throughout the body, potentially impacting heart health and the development of symptoms like bendopnea. Learning more about foods that cause inflammation might offer further insights into managing the risk factors for bendopnea and other heart conditions.
So, let’s explore how our choices at the dinner table can affect our overall well-being and potential susceptibility to heart-related symptoms like bendopnea.
Typical Patient Presentation
Patients experiencing bendopnea often describe a specific pattern of shortness of breath that worsens upon bending over. This is frequently accompanied by a sensation of tightness or pressure in the chest. The onset of symptoms is often gradual, with the patient potentially experiencing worsening symptoms over time. Important considerations include the patient’s history of heart failure, as well as the timing and duration of the symptom.
The patient may report a feeling of breathlessness and discomfort during the act of bending, which resolves when the patient resumes an upright position. Symptoms are often described as more pronounced after exertion.
Accompanying Symptoms
Several symptoms frequently accompany bendopnea in heart failure patients, providing crucial clues for diagnosis. These include fatigue, orthopnea (shortness of breath while lying down), paroxysmal nocturnal dyspnea (sudden awakening with shortness of breath), and edema (swelling in the legs and ankles). Additionally, patients may experience persistent cough, especially at night. The presence of these symptoms, along with the bendopnea, significantly increases the suspicion for heart failure.
Clinical Evaluation Procedures
The clinical evaluation for suspected bendopnea includes a thorough history taking, focusing on the specific characteristics of the shortness of breath, its relation to bending, and the presence of other symptoms. A physical examination is crucial, paying close attention to the patient’s respiratory status, heart rate and rhythm, and signs of fluid retention. Auscultation of the lungs may reveal crackles or wheezes, which could suggest pulmonary congestion.
Vital signs, including blood pressure and oxygen saturation, should be documented. A detailed review of the patient’s medical history, including any previous heart conditions, is also important.
Diagnostic Criteria for Suspected Heart Failure Based on Bendopnea
| Criterion | Description |
|---|---|
| History of Heart Failure | Patient has a prior diagnosis of heart failure. |
| Bendopnea Triggered by Bending | Shortness of breath significantly worsens upon bending and improves with upright posture. |
| Accompanying Symptoms | Presence of at least two of the following: orthopnea, paroxysmal nocturnal dyspnea, edema, persistent cough, fatigue. |
| Pulmonary Congestion Signs | Physical examination reveals crackles or wheezes in the lungs. |
| Elevated BNP Levels | Blood test shows elevated levels of brain natriuretic peptide (BNP). |
Diagnostic Considerations

Accurately diagnosing bendopnea, a newly recognized symptom of heart failure, is crucial for timely and effective treatment. Misdiagnosis can lead to delays in appropriate care, potentially worsening the patient’s condition. Differentiating bendopnea from other respiratory issues requires careful consideration of various factors, including patient history, physical examination findings, and specific diagnostic tests.
Distinguishing Bendopnea from Other Respiratory Conditions
Differentiating bendopnea from other respiratory conditions is essential to ensure accurate diagnosis and treatment. Common respiratory conditions, such as asthma, chronic obstructive pulmonary disease (COPD), and pneumonia, may present with symptoms similar to bendopnea. A comprehensive patient history, including details about the onset, duration, and characteristics of the breathlessness, is vital. The presence of associated symptoms, such as chest pain, edema, or orthopnea, can also aid in distinguishing bendopnea from other conditions.
A detailed physical examination, including auscultation of the lungs and evaluation of the cardiovascular system, is crucial in identifying distinguishing features. The specific context of the bendopnea, particularly its relation to body position and exertion, can further differentiate it from other respiratory issues. By considering these factors, healthcare providers can develop a more focused diagnostic approach.
Role of Imaging Techniques
Imaging techniques play a critical role in evaluating the underlying cause of bendopnea. Chest X-rays are commonly used to assess the presence of pulmonary congestion or other structural abnormalities. They can reveal signs of fluid accumulation in the lungs, which can be suggestive of heart failure. Echocardiograms provide a detailed visualization of the heart’s structure and function.
This allows clinicians to assess the pumping ability of the heart and identify any structural abnormalities that might be contributing to bendopnea. Echocardiograms are particularly valuable in evaluating the presence of systolic or diastolic dysfunction. Furthermore, the presence of an abnormal cardiac output, detected via echocardiography, can provide valuable diagnostic information.
Significance of Cardiac Biomarkers
Cardiac biomarkers, such as BNP (B-type natriuretic peptide) and NT-proBNP (N-terminal pro-B-type natriuretic peptide), are important in evaluating the likelihood of heart failure. Elevated levels of these biomarkers are strongly associated with heart failure and can support the diagnosis of bendopnea. The degree of elevation in cardiac biomarkers can help clinicians assess the severity of the underlying heart failure and guide treatment decisions.
The correlation between cardiac biomarker levels and the severity of heart failure, demonstrated in numerous studies, is a critical aspect of diagnosis.
Bendopnea, a newly identified symptom of heart failure, is intriguing. It’s a fascinating area of research, but considering the diverse spectrum of health conditions, it’s also important to remember factors like multiple sclerosis life expectancy can significantly impact overall well-being. Ultimately, understanding bendopnea and its implications for heart failure patients is crucial for better treatment and management.
Use of Physical Examination Findings
Physical examination findings are essential in assessing the severity and characteristics of bendopnea. Observations such as the presence of peripheral edema, jugular venous distention, or abnormal heart sounds can provide valuable clues about the underlying cardiac condition. The patient’s respiratory rate and oxygen saturation levels can also be assessed during the physical examination to gain insights into the severity of the respiratory distress.
By combining these findings with the patient’s history and imaging studies, a more comprehensive picture of the patient’s condition can be developed.
Diagnostic Tests Summary
| Diagnostic Test | Implications for Heart Failure Diagnosis (Considering Bendopnea) |
|---|---|
| Chest X-ray | Detects pulmonary congestion, pleural effusions, or other structural abnormalities suggestive of heart failure. |
| Echocardiogram | Evaluates heart function, identifies structural abnormalities, and assesses cardiac output, which are key indicators of heart failure. |
| Cardiac Biomarkers (BNP/NT-proBNP) | Elevated levels strongly suggest the presence of heart failure and help quantify its severity. |
| Physical Examination | Evaluates for peripheral edema, jugular venous distension, abnormal heart sounds, respiratory rate, and oxygen saturation, providing crucial clinical context for the diagnosis. |
Treatment Strategies
Bendopnea, the difficulty breathing when bending, is a significant symptom in heart failure patients, impacting their quality of life. Effective management requires a multifaceted approach targeting the underlying heart failure and its resultant effects on breathing. Treatment strategies should consider both pharmacological and non-pharmacological interventions tailored to individual patient needs.Addressing bendopnea involves more than simply treating the symptom; it’s crucial to understand and address the root cause of the difficulty in breathing during bending.
This includes optimizing heart function, improving fluid balance, and reducing strain on the respiratory system. Pharmacological interventions, alongside lifestyle modifications, are essential components of an effective treatment plan.
Medication for Improved Breathing During Bending
Medications play a pivotal role in managing bendopnea by addressing the underlying heart failure. Angiotensin-converting enzyme (ACE) inhibitors, angiotensin receptor blockers (ARBs), and beta-blockers are frequently prescribed to reduce fluid retention and improve heart function, thus decreasing strain on the respiratory system. These medications can significantly impact the ability to breathe comfortably during bending. Diuretics, such as furosemide, help to eliminate excess fluid from the body, easing the pressure on the lungs.
In some cases, oxygen therapy may be necessary to supplement the body’s oxygen supply, particularly in severe cases.
Non-Pharmacological Interventions
Non-pharmacological interventions are equally important in reducing the symptoms of bendopnea. Strategies focus on minimizing strain during bending and optimizing breathing techniques. Positioning and postural changes can be instrumental in reducing the effort required to breathe. Learning and practicing specific breathing exercises, such as diaphragmatic breathing, can enhance lung capacity and reduce shortness of breath during bending.
These techniques can improve respiratory efficiency, reducing the sensation of bendopnea.
Lifestyle Modifications
Lifestyle modifications can complement pharmacological and non-pharmacological interventions. A balanced diet low in sodium and saturated fats is essential for managing fluid balance, contributing to better overall heart health. Regular exercise, tailored to individual capabilities, can improve cardiovascular fitness and reduce the strain on the heart, easing the symptoms of bendopnea. Weight management is also crucial in reducing the burden on the cardiovascular system.
Limiting activities that exacerbate bendopnea, like strenuous physical activity immediately before or after bending, is another important lifestyle adjustment.
Comparison of Treatment Effectiveness
| Treatment | Mechanism of Action | Effectiveness (Moderate/High/Low) | Potential Side Effects |
|---|---|---|---|
| ACE Inhibitors | Reduce fluid retention, improve heart function | High | Dry cough, dizziness, kidney problems |
| ARBs | Reduce fluid retention, improve heart function | High | Dizziness, fatigue, headache |
| Beta-Blockers | Slow heart rate, reduce workload on the heart | High | Fatigue, dizziness, nausea |
| Diuretics | Remove excess fluid from the body | High | Dehydration, electrolyte imbalances |
| Breathing Exercises | Improve lung capacity, enhance breathing mechanics | Moderate | No significant side effects |
| Postural Changes | Reduce strain on the respiratory system during bending | Moderate | No significant side effects |
Research and Future Directions: Bendopnea A New Symptom Of Heart Failure
Bendopnea, the sensation of shortness of breath triggered by bending, presents a compelling area for further research. While initial observations suggest a correlation with heart failure, a robust body of evidence is crucial to solidify its recognition as a distinct symptom. Understanding the underlying mechanisms and refining diagnostic tools are paramount to improving patient care.The need for rigorous investigation into bendopnea’s role in heart failure diagnosis is underscored by the potential for early detection and intervention.
Early identification could lead to timely treatment and improved patient outcomes.
Areas of Current Research
Research into bendopnea is currently focused on establishing its physiological basis in heart failure patients. Studies are examining the interplay between cardiac function, pulmonary mechanics, and the postural changes associated with bending. Further exploration is also needed to determine if bendopnea is specific to heart failure or if it can be observed in other cardiovascular conditions.
Need for Further Studies
Validating bendopnea as a specific symptom requires large-scale, well-designed studies. These studies should incorporate detailed patient histories, comprehensive physical examinations, and objective measurements of respiratory function. Comparative analyses between patients with and without bendopnea and heart failure are essential to identify distinguishing characteristics. For instance, studies could compare the severity of bendopnea with other symptoms like dyspnea, orthopnea, and paroxysmal nocturnal dyspnea in different patient populations.
Potential Impact on Diagnosis and Management
The recognition of bendopnea as a reliable symptom could revolutionize the diagnostic process for heart failure. It could potentially serve as an early warning sign, enabling earlier intervention and potentially improving treatment outcomes. This new symptom could assist clinicians in differentiating heart failure from other respiratory conditions, leading to more accurate diagnoses. Consider a scenario where a patient experiencing bendopnea is initially misdiagnosed with asthma.
By incorporating bendopnea into the diagnostic algorithm, clinicians can identify and treat heart failure earlier, potentially improving patient prognosis.
Ongoing Investigations and Research Gaps
Ongoing investigations include exploring the correlation between bendopnea severity and the degree of cardiac impairment. Research gaps exist in defining the precise mechanisms linking postural changes, cardiac output, and respiratory function. The development of validated diagnostic tools specific to bendopnea, such as standardized questionnaires or objective physiological measurements, is also a significant need. Further research into the frequency and severity of bendopnea in different heart failure subtypes is required to refine its clinical utility.
Research Methodology for a Bendopnea Study
| Phase | Description |
|---|---|
| Patient Recruitment | Recruit a diverse cohort of patients suspected of having heart failure. Inclusion criteria should include confirmed heart failure diagnoses (based on established clinical guidelines) and a demonstrable history of bendopnea. Exclusion criteria should define specific conditions that might confound the study results. |
| Clinical Evaluation | Perform a thorough clinical assessment, including a detailed medical history, physical examination, and electrocardiogram (ECG) to evaluate the heart’s electrical activity. Pulmonary function tests, including spirometry, should be conducted to assess lung capacity. |
| Bendopnea Assessment | Develop a standardized questionnaire to assess the frequency, intensity, and characteristics of bendopnea. This questionnaire should be administered before and after specific exercises that induce postural changes, like bending over. |
| Cardiac Function Evaluation | Utilize echocardiography and other imaging modalities to measure cardiac output, ejection fraction, and left ventricular function. This is crucial for linking the observed bendopnea to underlying cardiac abnormalities. |
| Data Analysis | Employ statistical methods to analyze the collected data. Correlation analyses between bendopnea severity and cardiac function parameters will be crucial. Comparative analyses with similar patient groups without bendopnea are essential to determine the symptom’s specificity. The study should consider potential confounders, such as age, sex, and comorbidities. |
Closing Notes
In conclusion, bendopnea, while a relatively novel symptom, appears to be a significant indicator of heart failure. Further research is crucial to validate its diagnostic value and develop targeted treatment approaches. The identification of bendopnea as a distinct symptom may revolutionize how we diagnose and manage heart failure, potentially leading to earlier intervention and improved patient outcomes. Recognizing its unique presentation, physiological underpinnings, and clinical implications is key to ensuring timely and effective care.