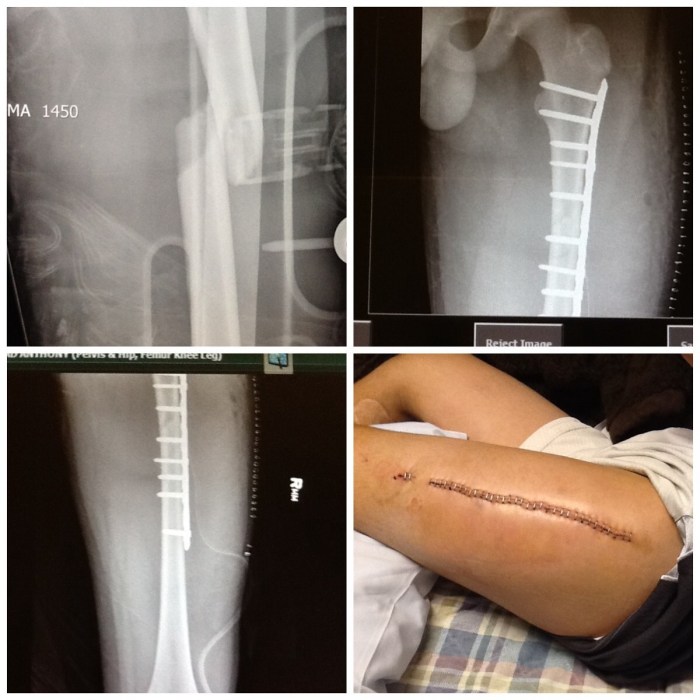
Removing metal plates screws rods after surgery – Removing metal plates, screws, and rods after surgery is a crucial procedure for many patients who have undergone various types of surgeries. This often involves a careful assessment of the patient’s condition, the type of implants used, and the specific surgical techniques employed. The process is carefully orchestrated to ensure the best possible outcome for the patient, minimizing risks and maximizing recovery.
This comprehensive guide dives into the nuances of removing metal implants after surgery. From the initial considerations and surgical techniques to post-operative care and potential complications, we explore the entire process to provide a thorough understanding for both patients and healthcare professionals.
Introduction to Post-Surgical Metal Removal
Post-surgical metal removal, a crucial aspect of patient recovery, involves the careful removal of metal plates, screws, and rods implanted during a surgical procedure. This procedure is often necessary to allow for the complete healing and restoration of the body’s natural structure. It’s important to understand the reasons behind this process, the types of implants commonly removed, and the history behind the development of this technique.This procedure aims to reduce the risk of complications associated with long-term metal implants.
These complications can range from infections to pain and discomfort, and even potential issues with the body’s natural healing processes. Understanding the rationale behind this procedure is crucial for patients and healthcare providers alike.
Common Reasons for Metal Removal
The decision to remove metal implants is not arbitrary. It’s driven by a range of factors, including potential infection risks, persistent pain, and the body’s ability to heal and regenerate. Sometimes, the implant itself can hinder proper bone growth or alignment. Furthermore, ongoing discomfort or limitations in mobility can prompt the need for removal.
Types of Metal Implants Removed
A variety of metal implants are used in surgical procedures. These implants can include plates, screws, and rods, each tailored to the specific needs of the surgical site. The material composition of these implants often includes titanium or stainless steel, chosen for their biocompatibility and strength.
History of Metal Implant Removal
The practice of removing metal implants has evolved over time. Early techniques were often less precise and carried higher risks. However, advances in surgical tools and techniques have significantly improved the safety and efficacy of this procedure. Improved imaging and surgical instruments, along with a deeper understanding of bone healing, have further refined the approach.
Types of Surgeries Requiring Metal Removal
The table below Artikels common surgical procedures where metal implant removal is a typical practice.
| Surgical Procedure | Description |
|---|---|
| Fracture Repair | Used to stabilize fractured bones, especially in long bones like the femur or tibia. The metal plates, screws, and rods provide support during healing. |
| Spinal Fusion | Involves joining two or more vertebrae to stabilize the spine. Metal plates and screws are often used to achieve this fusion. |
| Joint Replacement | Involves replacing damaged joints with artificial ones. Metal components may be used in the prosthesis, but these are not usually removed post-surgery. |
| Trauma Repair | Metal implants are crucial in situations like severe bone trauma, where stability is paramount. This includes situations like car accidents or other severe injuries. |
Pre-Removal Considerations: Removing Metal Plates Screws Rods After Surgery
Removing metal implants after surgery requires careful planning and patient evaluation. This stage isn’t just about scheduling the procedure; it’s about ensuring the patient is healthy enough to undergo the removal and minimizing potential complications. Understanding the patient’s overall health, the surgical approach, and the specific implant type are crucial for a successful and safe outcome.Thorough assessment of a patient’s readiness for metal removal is paramount.
This involves a multi-faceted evaluation considering the patient’s physical condition, the nature of the original surgery, and the potential impact of the removal on their ongoing health. It is not simply a matter of scheduling a procedure; rather, it is a comprehensive process of determining the best possible time and method for the removal of metal implants, taking into account the potential risks and benefits.
Patient Assessment for Metal Removal
A thorough medical history and review of previous surgical records are essential. This includes details about the initial surgery, the type of implant used, any complications experienced, and the patient’s current medical conditions. Knowledge of the patient’s current medications, allergies, and any pre-existing health issues is critical for tailoring the removal procedure to their specific needs. The medical history provides context for the patient’s overall health and helps predict potential risks or complications.
For example, a patient with a history of bleeding disorders would require a different approach than a patient with no such history.
Factors Influencing Removal Timing
Several factors influence the ideal timing for metal removal. The healing process following the initial surgery is crucial. Complete tissue healing and stabilization are prerequisites for a safe and effective removal procedure. Furthermore, the patient’s overall health, including their immune system function and ability to tolerate anesthesia, plays a significant role. The patient’s general health condition should be evaluated to ensure they are in the best possible condition to undergo the procedure.
For example, a patient with an uncontrolled infection would require addressing the infection before considering metal removal. The timing is also dependent on the specific implant and its location.
Importance of Patient History and Medical Records
Patient history and medical records provide valuable insights into the patient’s past surgical experiences and current health status. This information helps to identify any potential risks associated with the removal procedure, enabling proactive measures to mitigate those risks. For example, a patient with a history of poor wound healing might require extra monitoring during and after the removal process.
The medical records document the initial surgery and any complications encountered, which helps the surgical team understand the specific challenges of the removal process.
Potential Complications of Improper Removal
Inadequate planning or execution of metal removal can lead to various complications. These include, but are not limited to, infection, bleeding, nerve damage, damage to surrounding tissues, and the need for further surgical interventions. A thorough evaluation of the surgical approach is crucial to minimize these risks. For example, if the metal is located near vital nerves or blood vessels, the procedure may need to be modified to protect these structures.
Proper assessment of the patient’s health, surgical approach, and implant location are crucial to avoid complications.
Contrasting Surgical Approaches and Metal Removal Implications
| Surgical Approach | Implant Type | Potential Challenges in Removal | Notes |
|---|---|---|---|
| Open Approach | Large, exposed implants | Higher risk of tissue damage, potential for significant bleeding | Requires a larger incision and more extensive surgical exposure. |
| Minimally Invasive Approach | Smaller, less exposed implants | Lower risk of tissue damage, less bleeding | Often leads to faster recovery and less scarring. |
| Laparoscopic Approach | Implants within the abdominal cavity | Potential for damage to surrounding organs, specific instruments required | Suitable for certain abdominal procedures, offering less invasive access. |
The table above illustrates the potential differences in surgical approaches and their impact on the removal process. Each approach presents unique challenges, and the surgical team must carefully weigh the advantages and disadvantages for each patient.
Surgical Techniques for Metal Removal
Post-surgical metal removal, a crucial aspect of patient recovery, involves careful consideration of surgical techniques. The optimal approach depends on various factors, including the type of implant, the patient’s anatomy, and the surgeon’s expertise. Different techniques offer varying advantages and disadvantages, and a thorough understanding of these nuances is essential for successful outcomes.
Open Techniques
Open techniques for metal removal involve a larger incision compared to minimally invasive procedures. This approach provides direct access to the implant, allowing for greater visualization and precise manipulation of the implant and surrounding tissues. Open procedures often allow for a more thorough removal of the implant and any associated complications, which may include removal of scar tissue, or damaged surrounding tissue.
Getting those metal plates, screws, and rods out after surgery is a big deal, physically and emotionally. It’s a relief to finally have them removed, but the recovery process can sometimes be challenging. While you’re focused on healing, it’s also important to consider the potential emotional impact of the surgery, like how long depression might last after such a significant procedure.
Understanding the nuances of this emotional landscape is just as crucial as understanding the physical healing process. The journey of recovery from such a procedure often involves a lot of mental fortitude and a good understanding of your emotional well-being, like how long does depression last. Ultimately, the focus should return to the physical recovery, which is equally important to ensure a full and complete return to health.
- Direct Approach: A direct approach involves a straight incision over the implant. This method is commonly used for implants located in easily accessible areas. It offers good visualization and control, allowing for removal of the implant with minimal damage to surrounding structures. However, it may result in larger scars and potentially increased postoperative pain compared to minimally invasive approaches.
- Indirect Approach: An indirect approach involves making an incision at a location slightly removed from the implant. This method is used when direct access is difficult or the implant is located in a region that may be sensitive to a large incision. While this may reduce scarring, it can potentially make the procedure more complex, requiring greater surgical dexterity and precise maneuvering.
Minimally Invasive Techniques
Minimally invasive techniques are increasingly popular for metal removal. These approaches involve smaller incisions, often utilizing specialized instruments and techniques to reduce tissue trauma. Minimally invasive procedures typically result in less postoperative pain, faster recovery times, and smaller scars compared to open techniques.
- Percutaneous Techniques: Percutaneous techniques utilize small incisions or punctures to access the implant. This method often involves the use of specialized instruments, such as small retractors, and tools designed for navigating the target area with minimal disruption. Percutaneous techniques are advantageous in areas where minimizing scarring and promoting rapid recovery are priorities.
- Endoscopic Techniques: Endoscopic techniques employ a thin, flexible tube with a camera attached (endoscope) to visualize the implant and surrounding tissues. This method allows for a minimally invasive approach to access the implant, which can be especially beneficial in complex anatomical locations. This method requires significant surgical expertise to manipulate the implant while maintaining proper visualization through the endoscope.
Instrumentation
The choice of instruments used in metal removal surgery depends on the chosen surgical technique and the specific implant. A variety of specialized tools are available to assist in the procedure.
Getting those metal plates, screws, and rods removed after surgery is a big relief, but the recovery process can be mentally taxing. Think about how your brain is working during this period. Supplementing with citicoline, for instance, might support cognitive function, the cognitive benefits of citicoline are worth exploring. Ultimately, focusing on a healthy lifestyle and good nutrition will aid in the healing process and overall recovery after having the metal hardware removed.
| Instrument | Function |
|---|---|
| Osteotome | Used for cutting bone around the implant |
| Bone Rasp | Used for smoothing bone surfaces after implant removal |
| Screw Extractor | Specifically designed for removing screws |
| Plate Cutter | Used to cut the metal plate into smaller pieces for easier removal |
| Forceps | Used to grasp and manipulate the implant |
Post-Operative Care
The removal of metal plates, screws, and rods after surgery is a significant step toward recovery. Post-operative care plays a crucial role in ensuring a smooth healing process and minimizing potential complications. This phase involves meticulous attention to pain management, wound care, and adherence to prescribed instructions. A diligent approach to post-operative care significantly influences the patient’s overall outcome.
Crucial Steps in Post-Operative Care
Post-operative care encompasses a range of essential steps, all designed to promote healing and prevent complications. This involves close monitoring of the surgical site, diligent pain management, and adherence to prescribed medication regimens. Careful attention to nutritional needs and mobility is also crucial.
- Wound Care: Maintaining the integrity of the surgical incision is paramount. This includes keeping the wound clean and dry, as directed by the healthcare provider. Proper wound care prevents infection and promotes healing. Follow instructions regarding dressing changes, and report any signs of redness, swelling, pus, or excessive drainage immediately.
- Pain Management: Pain is a common post-operative experience. Healthcare professionals prescribe appropriate pain medications to manage discomfort. Patients should strictly adhere to the prescribed dosage and schedule. Non-pharmacological methods, such as ice packs and elevation, may also be recommended to manage pain.
- Medication Adherence: Taking prescribed medications, including antibiotics and pain relievers, as directed is critical. Skipping doses can compromise the effectiveness of treatment and potentially lead to complications. It is vital to understand the purpose of each medication and to promptly report any side effects.
- Diet and Nutrition: A balanced diet is essential for proper healing. Patients should focus on consuming nutrient-rich foods to support the body’s recovery process. Adequate protein intake is particularly important for tissue repair. Ensure you are drinking enough fluids, especially if taking pain medication.
- Activity Restrictions: Following the physician’s instructions regarding activity restrictions is crucial. Overexertion can hinder the healing process and potentially lead to complications. This includes avoiding strenuous activities, lifting heavy objects, and engaging in vigorous exercise.
Expected Healing Process
The healing process after metal removal surgery varies depending on individual factors such as age, overall health, and the extent of the procedure. Generally, the initial days involve inflammation and swelling around the surgical site. The body’s natural healing mechanisms kick in to repair the tissues, leading to gradual improvement.
- Early Healing: Early stages often involve discomfort, swelling, and bruising. These are normal responses to the surgical intervention and typically subside with time. Follow-up appointments will be scheduled to monitor healing progress.
- Mid-term Healing: As the healing progresses, swelling and discomfort reduce. Patients may experience a return to normal activities, gradually increasing their mobility. Monitoring the incision site for signs of infection is essential.
- Late-term Healing: The final stage involves complete wound closure and tissue regeneration. The surgical site heals completely, and the patient recovers full functionality. Continued monitoring is crucial to ensure long-term well-being.
Potential Complications
While metal removal surgery is generally safe, potential complications can occur. These complications, although rare, can be serious if not addressed promptly. Diligent post-operative care can help mitigate the risk of these complications.
- Infection: Infection is a possible complication that can manifest as redness, swelling, pain, or drainage at the surgical site. Prompt medical attention is crucial if any signs of infection appear.
- Bleeding: Excessive bleeding at the surgical site can be a complication. This is why monitoring the incision for excessive bleeding is critical. If bleeding occurs, contact your physician immediately.
- Nerve Damage: While rare, nerve damage is a potential complication that can manifest as numbness, tingling, or pain in the affected area. Immediate medical attention is essential.
- Adverse Drug Reactions: Reactions to pain medication or other prescribed medications can occur. If any unusual side effects arise, report them to your physician promptly.
Importance of Follow-up Appointments
Regular follow-up appointments are essential to monitor the healing process and address any concerns. These appointments allow healthcare providers to assess the surgical site, evaluate the patient’s progress, and adjust treatment plans if necessary. It is crucial to attend all scheduled appointments.
Pain Management Strategies and Side Effects
Effective pain management is critical during the post-operative period. A multi-pronged approach is often employed to minimize discomfort. These strategies can include oral medications, topical creams, and non-pharmacological interventions. It’s important to discuss potential side effects with your physician.
- Medications: Pain medication, as prescribed, is essential to control post-operative discomfort. Patients should closely follow the instructions provided by the healthcare provider regarding dosage and frequency.
- Non-Pharmacological Methods: Non-pharmacological methods, such as ice packs, elevation, and gentle exercises, can aid in pain management. These methods can be combined with medications to achieve better results.
- Potential Side Effects: Side effects of pain medications can vary. These may include nausea, vomiting, constipation, and drowsiness. Discuss any concerns or unusual side effects with your physician.
Post-Operative Care Instructions for Patients
Adherence to post-operative instructions is essential for successful recovery. These instructions are designed to guide patients through the healing process and minimize complications. Follow these instructions meticulously.
- Wound Care: Keep the incision site clean and dry. Follow the prescribed dressing instructions.
- Medication: Take prescribed medications as directed, and report any side effects.
- Activity: Avoid strenuous activities and follow the physician’s instructions on mobility.
- Diet: Maintain a balanced diet to support healing. Consume nutrient-rich foods.
- Follow-up: Attend all scheduled follow-up appointments.
Potential Complications and Risks
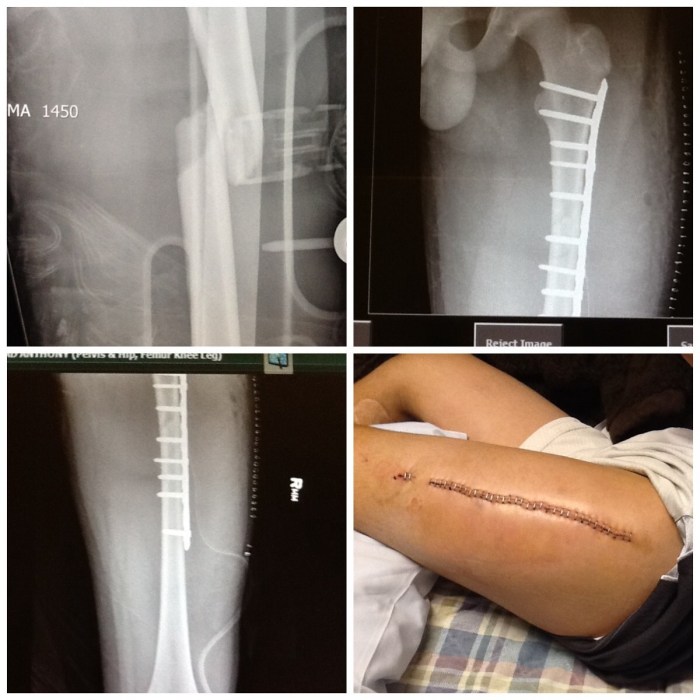
Post-surgical metal removal, while generally safe, carries potential complications. Understanding these risks allows for proactive measures to minimize harm and ensure a smooth recovery. Careful pre-operative assessment, meticulous surgical technique, and vigilant post-operative monitoring are crucial in managing these potential issues.
Potential Surgical Site Complications
Surgical site complications are a significant concern following any invasive procedure, including metal removal. These can manifest in various ways, affecting the healing process and potentially leading to discomfort or more serious issues. Careful attention to detail during the surgical procedure and meticulous post-operative care is paramount.
- Infection: Infections at the surgical site are a common concern, particularly in individuals with weakened immune systems or those who have underlying health conditions. Infections can range from mild, superficial skin infections to more serious deep tissue infections requiring prolonged treatment. Prompt recognition and appropriate antibiotic therapy are vital for managing infections effectively.
- Bleeding: Excessive bleeding at the surgical site is another potential risk. This can occur due to factors such as poor clotting, surgical trauma, or underlying blood disorders. Surgical techniques employing hemostatic agents and meticulous surgical hemostasis are implemented to minimize bleeding risk. In cases of significant bleeding, immediate intervention is required to prevent complications.
- Nerve Damage: Nerves are delicate structures that can be inadvertently damaged during the removal process. This can lead to varying degrees of sensory or motor dysfunction. Minimally invasive techniques and meticulous surgical dissection help to minimize nerve damage. Post-operative neurological assessment is critical in detecting and managing any potential nerve injury.
- Wound Dehiscence: Wound dehiscence, or the separation of the surgical wound edges, is a significant concern. This can be exacerbated by factors such as poor wound healing, excessive coughing, or straining. Proper wound closure techniques, appropriate wound dressings, and patient education on avoiding strain are crucial.
Potential Systemic Complications
While primarily focused on the surgical site, metal removal can occasionally lead to systemic complications, impacting the patient’s overall health. A thorough pre-operative evaluation helps identify potential risk factors.
- Adverse Reactions to Anesthesia: Patients undergoing anesthesia are at risk for various adverse reactions, ranging from allergic responses to more serious complications such as respiratory depression. Pre-operative assessment for allergies and other medical conditions, alongside careful monitoring during and after anesthesia, are critical.
- Blood Clots: Blood clots, particularly deep vein thrombosis (DVT), are a possible complication in the postoperative period, particularly in patients with a history of blood clotting disorders or prolonged immobility. Early mobilization, anticoagulant therapy, and regular monitoring for signs of blood clots are important preventative measures.
Management Strategies
A comprehensive approach to mitigating these risks involves a multi-faceted strategy.
| Potential Complications | Management Strategies |
|---|---|
| Infection | Antibiotic prophylaxis, meticulous wound care, prompt treatment of infection |
| Bleeding | Hemostatic agents, meticulous surgical technique, blood transfusions (if needed) |
| Nerve Damage | Minimally invasive techniques, meticulous surgical dissection, post-operative neurological assessment |
| Wound Dehiscence | Proper wound closure, appropriate wound dressings, patient education on avoiding strain |
| Adverse Reactions to Anesthesia | Pre-operative assessment, careful monitoring during and after anesthesia, appropriate management of reactions |
| Blood Clots | Early mobilization, anticoagulant therapy, regular monitoring for signs of blood clots |
Patient Education and Preparation
Navigating the path to metal removal surgery can feel daunting. This section focuses on empowering you with the knowledge and tools necessary to confidently prepare for your procedure. Understanding the process, both physically and emotionally, is key to a smoother recovery. We’ll delve into the importance of patient cooperation, the potential psychological impact, and the practical steps you can take to ensure a positive experience.
Understanding the Procedure
Metal removal surgery, while often a necessary step in post-surgical recovery, can raise concerns. This section clarifies the procedure’s nature, its purpose, and the expected outcome. A thorough understanding of the procedure will significantly reduce anxiety and promote a more positive experience. The surgical team will discuss all aspects of the procedure in detail.
Importance of Patient Understanding and Cooperation
Active participation in the pre-operative process is crucial for a successful outcome. Your understanding of the procedure, its purpose, and potential risks is vital for informed consent and cooperation during the procedure. This will lead to a better outcome and quicker recovery. Your active involvement and cooperation with the medical team significantly influence the overall success of the surgery.
Removing metal plates, screws, and rods after surgery can be a complex process, often requiring careful consideration of the specific procedure. For example, in a splenectomy, or spleen removal surgery, splenectomy spleen removal surgery might involve different removal strategies than other types of surgeries. Ultimately, the best approach to removing these implants is determined by the surgeon and the patient’s unique circumstances.
Potential Psychological Impact, Removing metal plates screws rods after surgery
The anticipation of surgery can evoke various emotional responses. These responses can range from anxiety and fear to apprehension and uncertainty. Addressing these concerns proactively is paramount to maintaining emotional well-being. Patients may experience anxiety, fear, or uncertainty regarding the surgery. Open communication with the surgical team and support from loved ones can alleviate these concerns.
Pre-Operative Instructions
Proper preparation significantly impacts the surgical process and post-operative recovery. Adhering to pre-operative instructions is essential to ensure a safe and successful operation.
- Fasting Guidelines: A crucial step in preparing for surgery is adhering to fasting instructions. This helps prevent complications during the procedure. Specific guidelines vary, but typically involve abstaining from food and drink for a set period before surgery. Consult your physician for precise details, as the time frame depends on the type of procedure.
- Medication Management: Inform your doctor about all medications you’re currently taking, including prescription drugs, over-the-counter medications, and supplements. This is crucial for managing potential interactions or adjusting dosages as needed. Be honest about your medication history, even if it seems insignificant.
- Arranging Post-Operative Care: Ensure you have a support system in place for post-operative care. Arrange for transportation and someone to assist with daily tasks after surgery. This includes ensuring you have a designated person to accompany you home and assist with activities of daily living.
Step-by-Step Guide for Preparing for the Procedure
A well-structured pre-operative plan reduces stress and ensures a smooth transition to the procedure. This section provides a clear roadmap to guide you through the preparation process.
- Initial Consultation: Schedule a consultation with the surgeon to discuss your medical history, concerns, and expectations. This initial meeting allows you to ask questions and receive personalized guidance regarding the procedure.
- Pre-operative Tests: Understand and prepare for any necessary pre-operative tests, such as blood work or imaging studies. These tests help evaluate your overall health and ensure the safety of the procedure.
- Medication Review: Review all medications with your doctor, including prescription drugs, over-the-counter medications, and supplements. This step ensures that there are no harmful interactions with the medications used during the procedure.
- Follow-up Appointments: Attend all scheduled follow-up appointments with your doctor and the surgical team. These appointments provide crucial updates, answer questions, and allow for monitoring of your progress.
- Emotional Preparation: Engage in stress-reducing activities, such as meditation, yoga, or deep breathing exercises, to manage anxiety and promote a positive mindset. Seek emotional support from family, friends, or a therapist.
Case Studies and Examples
Real-world application is crucial to understanding the nuances of metal removal procedures. Case studies provide invaluable insights into successful and challenging procedures, highlighting the importance of pre-operative planning, surgical technique, and post-operative management. They illustrate how patient-specific factors can impact the procedure, and demonstrate the wide spectrum of possible outcomes.
Illustrative Case Studies of Successful Metal Removal
Many successful procedures involve the removal of plates and screws from fractures, particularly in the long bones. A typical case might involve a patient who underwent a tibia fracture repair with a plate and screws 18 months prior. Pre-operative planning, including meticulous radiographic analysis and discussion of potential complications with the patient, is paramount. The surgical technique involves careful dissection of the soft tissues surrounding the hardware, followed by precise removal of the plate and screws.
Post-operative care focuses on monitoring for infection and ensuring proper bone healing. A successful outcome is characterized by minimal complications, restoration of function, and radiographic evidence of sound bone healing. The patient’s pain levels decrease significantly, and their mobility improves.
Challenging Cases and Resolution Approaches
Certain cases present unique challenges. For example, a patient with a history of infection at the surgical site presents a heightened risk of wound complications during the metal removal procedure. The surgical team may need to employ more aggressive wound debridement techniques and consider antibiotic prophylaxis. Another challenge might arise from a complex fracture configuration, which necessitates careful planning and precise surgical technique to avoid further damage to the surrounding tissues.
In these instances, the surgical team might consider alternative approaches, like using specialized instruments or modifying the surgical plan to address the unique challenges.
Impact of Patient Characteristics on Metal Removal
Patient characteristics can significantly affect the procedure. A patient with osteoporosis, for example, may have a lower bone density, making the removal of hardware more delicate. Similarly, a patient with impaired mobility or a compromised immune system may present unique challenges regarding post-operative care and recovery. The surgeon must consider these factors during pre-operative planning and tailor the surgical approach accordingly.
This approach ensures the best possible outcome while minimizing the risks associated with the patient’s specific conditions.
Detailed Descriptions of Successful Outcomes
Successful outcomes are characterized by several key indicators. A reduction in pain, improved mobility, and the absence of complications are crucial factors. Radiographic evidence of appropriate bone healing is essential, showing that the bone has adequately integrated after hardware removal. A reduction in inflammation and swelling, along with the absence of infection, are further indicators of a successful outcome.
In most cases, patients report a marked improvement in their quality of life after the procedure. The surgeon’s assessment of the patient’s progress, combined with objective findings from imaging studies, confirms the successful removal of the hardware.
Examples of Pre- and Post-Operative X-rays
Pre-operative X-ray: (Illustrative description – a radiograph would show a fracture of the femur with a metal plate and screws in place. The plate and screws are clearly visible, along with the surrounding bone structure.)
Post-operative X-ray: (Illustrative description – a radiograph would show the metal plate and screws have been removed. The fracture site is healed and the bone appears intact, without any visible signs of complications.)
Final Conclusion
In conclusion, removing metal plates, screws, and rods after surgery is a specialized procedure requiring meticulous planning and execution. The careful consideration of pre-operative factors, surgical techniques, and post-operative care are all essential to ensure a smooth recovery. Understanding the potential complications and risks is equally crucial, allowing for informed decision-making and proactive management. This detailed look at the process empowers patients and medical professionals alike to approach this critical aspect of surgical care with confidence and preparedness.