Medications to treat bipolar disorder are a crucial part of managing this complex condition. This in-depth exploration delves into the various types of medications, their mechanisms of action, potential side effects, and considerations for individual treatment plans. We’ll cover everything from mood stabilizers and antipsychotics to combination therapies and the importance of patient factors in medication selection. Understanding these aspects is essential for those navigating bipolar disorder and their healthcare providers.
This guide provides a concise overview of bipolar disorder medications, including a description of the condition, common symptoms, and general principles of medication treatment. We’ll explore different classes of medications and present key information in a structured format. The focus is on practical application and patient understanding, highlighting important factors like side effects, interactions, and long-term management.
Overview of Bipolar Disorder Medications
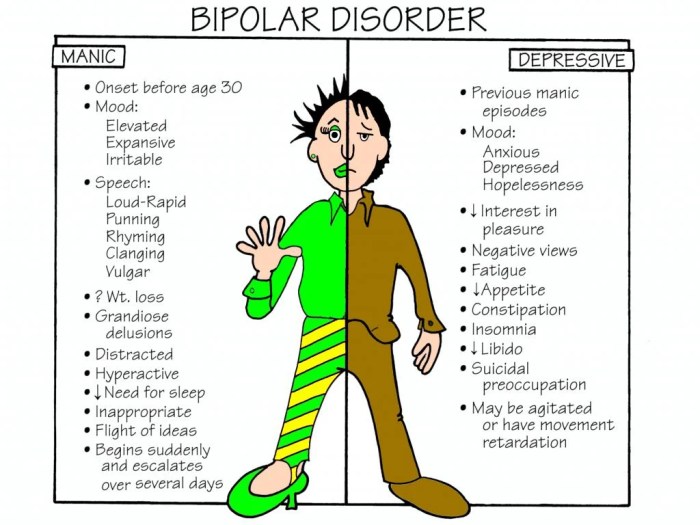
Bipolar disorder is a chronic mental illness characterized by significant mood swings, ranging from extreme highs (mania or hypomania) to deep lows (depression). These fluctuations can significantly impact a person’s daily life, affecting their relationships, work, and overall well-being. Understanding the medications used to manage these mood shifts is crucial for effective treatment.Medication plays a vital role in stabilizing mood swings and preventing future episodes in bipolar disorder.
Finding the right medication for bipolar disorder can be a real journey, with lots of trial and error. It’s crucial to understand the nuances of each option, and sometimes, a seemingly unrelated issue like skin conditions can actually mask underlying health concerns. For example, if you’re experiencing unexplained skin problems, consulting a specialist to rule out any misdiagnosis is key, like at ask an expert avoid misdiagnosis for skin conditions.
Ultimately, a thorough understanding of your body and its various signals is vital for successfully managing bipolar disorder.
The general principles behind medication treatment aim to reduce the severity and frequency of manic and depressive episodes, while also promoting overall well-being. This often involves a combination of medications, tailored to the individual’s specific needs and responses. The selection and dosage of medications are typically determined through careful monitoring and adjustments by a psychiatrist or other qualified medical professional.
Types of Medications Used
Bipolar disorder medications are generally categorized into mood stabilizers, antipsychotics, and antidepressants. These classes work through different mechanisms to target various aspects of the disorder. Mood stabilizers, as the name suggests, are primarily focused on regulating mood fluctuations, while antipsychotics can help manage the intense symptoms of mania or psychosis. Antidepressants are often used cautiously, in conjunction with other medications, to address depressive episodes.
Medication Classes and Their Actions
| Medication Name | Class | Primary Mechanism of Action | Common Side Effects |
|---|---|---|---|
| Lithium | Mood Stabilizer | Alters sodium transport in nerve cells, influencing neurotransmitter release and receptor sensitivity. | Tremor, weight gain, thirst, increased urination, kidney problems (with long-term use). |
| Valproate (Depakote) | Mood Stabilizer | Inhibits GABA activity and influences other neurotransmitters, affecting mood and preventing seizures. | Nausea, vomiting, weight gain, hair loss, liver problems (requires monitoring). |
| Lamotrigine (Lamictal) | Mood Stabilizer | Modulates glutamate and other neurotransmitter activity, stabilizing mood and reducing seizures. | Skin rash (Stevens-Johnson syndrome), nausea, dizziness, headache. |
| Aripiprazole (Abilify) | Antipsychotic | Dopamine system stabilizer; modulates dopamine and serotonin activity. | Nausea, dizziness, anxiety, insomnia, akathisia (restlessness). |
| Quetiapine (Seroquel) | Antipsychotic | Works on multiple neurotransmitter systems, particularly serotonin and dopamine. | Sedation, weight gain, constipation, dry mouth, blurred vision. |
| Olanzapine (Zyprexa) | Antipsychotic | Works on multiple neurotransmitter systems, affecting dopamine and serotonin. | Significant weight gain, increased cholesterol, elevated blood sugar, sedation. |
| Fluoxetine (Prozac) | Antidepressant | Inhibits serotonin reuptake, increasing serotonin levels in the brain. | Nausea, insomnia, sexual dysfunction, anxiety. |
Important Considerations
The selection of medications for bipolar disorder requires careful consideration of individual patient needs and responses. Dosage and combinations may need adjustments over time, and close monitoring by healthcare providers is essential. This approach helps to ensure the safety and efficacy of treatment. Patients should be informed about potential side effects and encouraged to report any concerns promptly.
Managing bipolar disorder often involves a cocktail of medications, each with potential side effects. Sometimes, these medications can lead to issues like hand weakness, which can stem from various factors, including the medication itself or other underlying health conditions. For a deeper understanding of the potential causes of hand weakness, check out this helpful resource on causes of hand weakness.
Ultimately, it’s crucial to discuss any unusual symptoms with your doctor, especially when considering medications for bipolar disorder, to ensure the best possible treatment plan.
Specific Medications for Bipolar Disorder
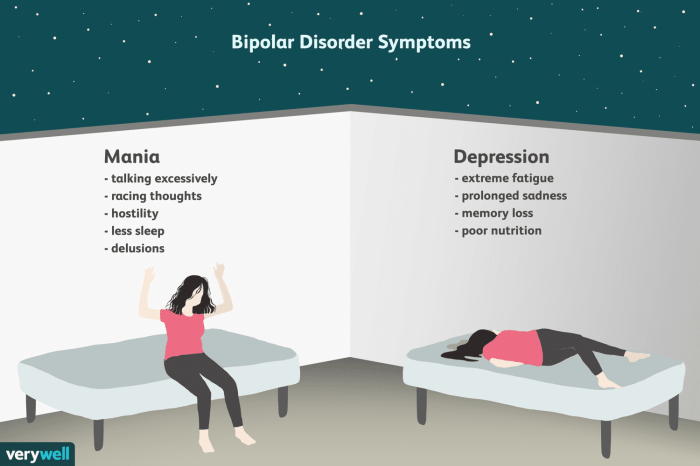
Understanding the specific medications used in treating bipolar disorder is crucial for managing the condition effectively. Different medications target various aspects of the disorder, aiming to stabilize mood swings and prevent episodes of mania or depression. This section delves into commonly prescribed mood stabilizers, examining their mechanisms of action, dosages, administration, and potential side effects.The selection of a medication for bipolar disorder is a complex process.
A healthcare professional, considering individual patient needs and responses, plays a vital role in prescribing and monitoring treatment. Individual responses to medications vary, and close monitoring of patients is essential to adjust the treatment plan as needed.
Mood Stabilizers: Lithium
Lithium is a widely used mood stabilizer for bipolar disorder. Its mechanism of action is not fully understood, but it is believed to affect neurotransmitter systems and ion transport. Lithium is known for its effectiveness in preventing both manic and depressive episodes.Typical dosages for lithium vary, but generally range from 300 to 1200 mg daily, divided into multiple doses.
The administration route is typically oral. Blood levels of lithium are crucial to monitor, as they need to be carefully maintained within a therapeutic range to prevent toxicity. Frequent blood tests are essential to ensure the lithium level remains optimal and safe. Monitoring parameters include checking lithium levels, renal function, and thyroid function, all of which are affected by lithium treatment.
Mood Stabilizers: Valproate
Valproate, also known as divalproex sodium, is another frequently prescribed mood stabilizer. Valproate is effective in treating manic episodes and preventing both manic and depressive episodes. It’s known for its rapid onset of action.The typical dosage for valproate varies based on the patient’s needs. Administration is usually oral. Like lithium, close monitoring of blood levels is necessary to prevent potential side effects and toxicity.
Monitoring parameters include valproate levels, liver function tests, and complete blood counts (CBCs). Regular blood tests are crucial to maintain the drug within the therapeutic range.
Mood Stabilizers: Lamotrigine
Lamotrigine is a mood stabilizer that is primarily used to prevent depressive episodes in bipolar disorder. It is less effective in managing manic episodes. Lamotrigine has a different mechanism of action compared to lithium or valproate, which makes it a valuable addition to treatment strategies.The typical dosage for lamotrigine is usually initiated at a low dose and gradually increased over several weeks.
Finding the right medication for bipolar disorder can be a real journey, and it’s important to remember that everyone responds differently. While exploring treatment options, it’s also fascinating to consider the nuances of health conditions like prostate cancer. For instance, did you know that women can’t get prostate cancer? can women get prostate cancer Understanding the differences between various medical conditions can help us better grasp the complexities of treatments like those for bipolar disorder.
The administration route is typically oral. A gradual increase in dosage is crucial to avoid a serious side effect known as Stevens-Johnson syndrome. Monitoring parameters include complete blood counts (CBCs), renal function tests, and liver function tests. Close monitoring of the skin is crucial during the initial stages of treatment.
Comparison of Mood Stabilizers
| Characteristic | Lithium | Valproate | Lamotrigine |
|---|---|---|---|
| Efficacy | Effective in preventing both mania and depression | Effective in managing mania and preventing both mania and depression | Primarily effective in preventing depression |
| Side Effect Profile | Potential for tremor, weight gain, gastrointestinal upset, kidney problems | Potential for nausea, vomiting, hair loss, weight gain, and liver problems | Potential for rash (Stevens-Johnson syndrome), dizziness, nausea, and headache |
| Drug Interactions | Numerous drug interactions, particularly with diuretics and NSAIDs | Drug interactions with certain medications, including warfarin | Fewer drug interactions compared to lithium and valproate |
| Monitoring Parameters | Lithium levels, renal function, thyroid function | Valproate levels, liver function tests, CBCs | Complete blood counts (CBCs), renal function, liver function |
The table above highlights key differences between these mood stabilizers, including their effectiveness, side effect profiles, and potential drug interactions. This information is intended to provide a general overview and should not be considered medical advice. Consult a healthcare professional for personalized treatment recommendations.
Antipsychotics in Bipolar Disorder Treatment
Antipsychotic medications play a crucial role in managing bipolar disorder, particularly during acute manic or mixed episodes. They are often used in combination with mood stabilizers to help control the intense mood swings and associated symptoms. Their efficacy in preventing relapse and reducing the severity of future episodes is also significant. Understanding the different types of antipsychotics and their potential effects is vital for effective treatment planning.Antipsychotics work by targeting neurotransmitters in the brain, particularly dopamine and serotonin, which are implicated in the pathophysiology of bipolar disorder.
They aim to reduce the intensity of manic symptoms and promote a more stable mood. The choice of antipsychotic, its dosage, and its combination with other medications are tailored to the individual patient’s needs and response.
Types of Antipsychotics
Antipsychotics are broadly categorized into typical and atypical antipsychotics. Each category has distinct mechanisms of action and potential side effect profiles.
Typical Antipsychotics
These medications, often used in the past for their effectiveness in reducing positive symptoms of psychosis, are now less commonly used for bipolar disorder due to their potential for more severe side effects. They primarily target dopamine receptors.
- Chlorpromazine (Thorazine): A first-generation antipsychotic known for its broad range of actions. It can be effective in reducing manic symptoms but is associated with a higher risk of extrapyramidal side effects, such as parkinsonism and tardive dyskinesia.
- Haloperidol (Haldol): A potent antipsychotic often used for its rapid action. It can effectively manage severe manic episodes, but also carries a significant risk of extrapyramidal side effects.
Atypical Antipsychotics
Atypical antipsychotics have emerged as a more preferred option for treating bipolar disorder due to their broader efficacy and generally lower risk of extrapyramidal side effects. They tend to have a more balanced effect on dopamine and serotonin systems.
- Risperidone (Risperdal): This atypical antipsychotic is frequently used in bipolar disorder to manage manic episodes and prevent relapse. It is generally well-tolerated, with a lower risk of extrapyramidal side effects compared to typical antipsychotics.
- Quetiapine (Seroquel): Often prescribed for bipolar disorder, particularly in managing acute mania and mixed episodes. It is generally considered well-tolerated and has a lower risk of weight gain compared to some other atypical antipsychotics.
- Olanzapine (Zyprexa): This medication is often used for managing manic episodes, and has shown some effectiveness in preventing future episodes. However, it is associated with a higher risk of weight gain and metabolic syndrome.
- Aripiprazole (Abilify): This medication is considered a dopamine system stabilizer, potentially offering a more balanced effect on mood and reducing the risk of extrapyramidal side effects. It can be used in both acute and maintenance phases of bipolar disorder.
Potential Benefits and Risks
Antipsychotics can be highly effective in controlling acute manic or mixed episodes, preventing relapse, and improving overall functioning. However, they carry potential risks, including side effects and the need for careful monitoring. Individual responses to medications vary, and clinicians must carefully weigh the benefits against the potential risks for each patient.
Antipsychotic Medications Summary
| Medication | Mechanism of Action | Typical Uses | Potential Side Effects |
|---|---|---|---|
| Chlorpromazine | Dopamine receptor antagonism | Acute mania, psychosis | Extrapyramidal symptoms, sedation, orthostatic hypotension |
| Haloperidol | Dopamine receptor antagonism | Severe mania, psychosis | Extrapyramidal symptoms, tardive dyskinesia, neuroleptic malignant syndrome |
| Risperidone | Dopamine and serotonin receptor antagonism | Mania, mixed episodes, prevention of relapse | Extrapyramidal symptoms (less common), weight gain, sedation |
| Quetiapine | Dopamine and serotonin receptor antagonism | Mania, mixed episodes, prevention of relapse | Sedation, weight gain, orthostatic hypotension |
| Olanzapine | Dopamine and serotonin receptor antagonism | Mania, mixed episodes, prevention of relapse | Weight gain, metabolic syndrome, sedation |
| Aripiprazole | Dopamine system stabilizer | Mania, mixed episodes, prevention of relapse | Akathisia, nausea, anxiety |
Combination Therapies
Bipolar disorder is a complex illness, and often requires a multifaceted approach to treatment. While monotherapy (using a single medication) can be effective for some individuals, combining different medications can offer significant advantages in managing the varied symptoms and preventing relapses. This approach allows for a more personalized strategy tailored to the specific needs of each patient.Combining medications for bipolar disorder is not merely an arbitrary decision.
It’s a calculated strategy aimed at optimizing symptom control, reducing the risk of relapse, and improving overall quality of life. By carefully selecting and monitoring the combination, clinicians strive to achieve a balance between effectiveness and potential side effects. Understanding the rationale behind these combinations is crucial for both patients and healthcare providers.
Rationale for Combination Therapies
Combining medications in bipolar disorder treatment often arises from the need to address multiple facets of the illness. For instance, a patient might experience both mood swings and psychosis, or anxiety alongside depression. Different medications can target specific symptoms more effectively than a single agent. A combination therapy strategy might address different neurotransmitter systems in the brain, leading to improved mood regulation and reduced symptoms.
For example, an antipsychotic might control psychotic features while a mood stabilizer helps manage mood fluctuations.
Potential Benefits of Combination Therapies
Combination therapies can offer several potential benefits. Enhanced symptom control is a key advantage. By addressing multiple aspects of the illness simultaneously, clinicians can often achieve a more stable and improved mood state. Reduced relapse risk is another important consideration. A well-designed combination therapy can help prevent future episodes of mania or depression.
Improved adherence to treatment is possible, as a combination therapy can be more effective in managing specific symptoms, thereby potentially leading to a better patient experience and reducing the likelihood of discontinuation.
Potential Challenges of Combination Therapies
Despite the potential benefits, combination therapies present certain challenges. The increased complexity of medication regimens can lead to more side effects, both in terms of frequency and severity. Close monitoring and careful adjustment of dosages are essential to minimize these side effects. Interactions between different medications can also be a concern. Drug interactions can significantly alter the effectiveness of individual medications or create new side effects.
The potential for increased complexity in patient education and management is another aspect that needs consideration. Healthcare professionals must meticulously explain the rationale and potential risks of the combined therapy.
Examples of Common Medication Combinations
Several common medication combinations are used for specific bipolar disorder presentations. These combinations are often tailored to the individual’s symptoms and response to treatment.
Medication Combinations Table
| Medication Combination | Rationale | Specific Bipolar Presentation |
|---|---|---|
| Mood stabilizer (e.g., Lithium) + Antipsychotic (e.g., Quetiapine) | Addresses mood swings and psychosis simultaneously. Quetiapine can help reduce agitation and psychotic symptoms while lithium stabilizes mood. | Bipolar disorder with prominent mood swings and psychotic features. |
| Antidepressant (e.g., Bupropion) + Mood stabilizer (e.g., Lamotrigine) | Combines mood stabilization with potential antidepressant effects. Bupropion can be effective for depression and anxiety while lamotrigine stabilizes mood. | Bipolar disorder with depressive episodes. |
| Mood stabilizer (e.g., Valproate) + Antipsychotic (e.g., Risperidone) | Addresses mood instability and potential psychotic symptoms. Valproate helps stabilize mood while Risperidone addresses psychotic features. | Bipolar disorder with rapid cycling and/or psychotic symptoms. |
Medication Selection and Patient Factors: Medications To Treat Bipolar Disorder
Choosing the right medication for bipolar disorder is crucial, as each patient’s experience is unique. A personalized approach, considering individual characteristics and potential interactions, is essential for effective treatment. This section delves into the critical factors influencing medication selection and the vital role of patient education in successful management.Effective bipolar disorder management requires a deep understanding of how individual factors influence medication response and adherence.
Tailoring treatment plans to the specific needs of each patient maximizes the chances of achieving remission and maintaining stability.
Individualized Medication Selection
Individualized medication selection is paramount for optimal treatment outcomes. This approach recognizes that the same medication might not produce the same results for all patients, and factors like age, comorbidities, and family history play significant roles. Careful consideration of these elements is crucial for tailoring the most appropriate treatment strategy.
Factors Influencing Medication Selection
Several factors significantly influence the choice of medication and its potential effectiveness. Age, for example, can impact metabolism and the body’s response to different medications. Co-occurring conditions, such as anxiety or substance use disorders, can further complicate the selection process, necessitating careful consideration of potential interactions and the need for a multifaceted approach. Pre-existing medical conditions and family history of medication responses provide valuable insights into potential risks and benefits.
Finally, the patient’s current medications and lifestyle choices must be factored into the selection process to prevent adverse interactions.
Patient Education and Adherence
Patient education plays a critical role in successful bipolar disorder management. Patients need to understand their condition, the purpose of their medications, potential side effects, and the importance of adherence to the prescribed regimen. This understanding empowers them to actively participate in their treatment and promotes better outcomes. Clear communication between the healthcare provider and patient is essential to address concerns and build trust, fostering better adherence.
Table: Patient Factors Influencing Medication Selection and Response
| Patient Factor | Potential Impact on Medication Selection | Example |
|---|---|---|
| Age | Metabolism and response to medications may differ across age groups. | Older adults may require lower doses of certain medications due to slower metabolism. |
| Comorbidities (e.g., anxiety, substance use disorder) | May influence medication choice due to potential interactions or the need for a multi-pronged approach. | A patient with both bipolar disorder and anxiety may benefit from a medication combination targeting both conditions. |
| Current Medications | Potential drug interactions need careful evaluation. | A patient taking multiple medications, including over-the-counter drugs, might require adjustments to avoid interactions. |
| Family History | Family history of medication response or adverse events can provide valuable insights. | If a family member experienced significant side effects from a particular medication, it’s crucial to consider this factor. |
| Lifestyle Factors | Lifestyle choices, such as diet and exercise, can influence medication effectiveness and overall health. | A patient with poor sleep habits might experience more side effects from certain medications. |
| Patient Preferences and Beliefs | Individual preferences and beliefs about medication can affect adherence and outcomes. | A patient who is skeptical about medication might require more intensive education and support to adhere to the regimen. |
Side Effects and Management
Medication side effects are a common concern for individuals managing bipolar disorder. Understanding the potential side effects and developing strategies for management is crucial for maintaining adherence to treatment and achieving optimal well-being. This section delves into common side effects, strategies for minimizing them, and how to report serious reactions to healthcare providers.Managing side effects effectively empowers individuals to continue their medication regimen and maintain a healthy lifestyle.
This proactive approach is essential for symptom control and overall well-being.
Common Side Effects
Recognizing the range of potential side effects is essential for both patients and healthcare providers. Common side effects can vary depending on the specific medication and individual factors. These effects often improve over time as the body adjusts to the medication.
- Gastrointestinal Issues: Nausea, vomiting, diarrhea, and constipation are frequent gastrointestinal side effects. These symptoms can often be managed with dietary adjustments and over-the-counter medications, but it’s important to consult a healthcare professional for severe or persistent issues.
- Sleep Disturbances: Some medications can affect sleep patterns, causing insomnia or excessive sleepiness. Maintaining a consistent sleep schedule and avoiding caffeine or alcohol before bed can help manage these sleep-related side effects.
- Weight Changes: Changes in appetite and metabolism can lead to weight gain or loss. Dietary modifications and regular exercise can help manage weight fluctuations associated with medication.
- Neurological Effects: Drowsiness, dizziness, and headaches are common neurological side effects. These symptoms usually subside as the body adjusts to the medication. It’s important to communicate any persistent or severe neurological symptoms to your doctor.
Strategies for Minimizing Side Effects
Taking proactive steps to mitigate side effects can significantly improve a patient’s experience and adherence to treatment.
- Medication Timing: Taking medications with food can help reduce gastrointestinal distress. Adjusting the timing of medication intake may also help manage sleep disturbances.
- Lifestyle Modifications: Maintaining a balanced diet, regular exercise, and sufficient sleep can help minimize some side effects. For example, a healthy diet can mitigate weight changes and support overall well-being.
- Communication with Healthcare Providers: Open communication with healthcare providers is essential. Report any side effects, no matter how minor they seem, to allow for adjustments to the treatment plan. This includes both common and less common symptoms.
Recognizing and Reporting Serious Side Effects
Recognizing and promptly reporting serious side effects is critical for patient safety. These reactions require immediate medical attention.
- Mental Health Changes: Sudden or significant changes in mood, behavior, or thoughts are serious concerns. Symptoms such as severe anxiety, depression, agitation, or psychosis require immediate medical evaluation.
- Cardiovascular Issues: Symptoms like chest pain, palpitations, or shortness of breath may indicate potential cardiovascular problems. These require immediate medical attention.
- Skin Reactions: Rashes, hives, or other skin reactions can be serious and should be reported immediately. Severe skin reactions can indicate an allergic reaction.
- Neurological Issues: Seizures, tremors, or difficulty with coordination are serious neurological side effects that warrant immediate medical attention.
Summary of Common Side Effects
| Side Effect | Potential Severity | Management Strategies |
|---|---|---|
| Nausea | Mild to Moderate | Taking medication with food, using anti-nausea medications as prescribed. |
| Insomnia | Mild to Moderate | Establishing a regular sleep schedule, avoiding caffeine before bed. |
| Weight Gain | Mild to Moderate | Balanced diet, regular exercise, and medical consultation if necessary. |
| Headache | Mild to Moderate | Over-the-counter pain relievers, hydration, and medical consultation if severe. |
| Suicidal Thoughts | High | Immediate medical attention, hospitalization, and follow-up with a mental health professional. |
Medication Interactions
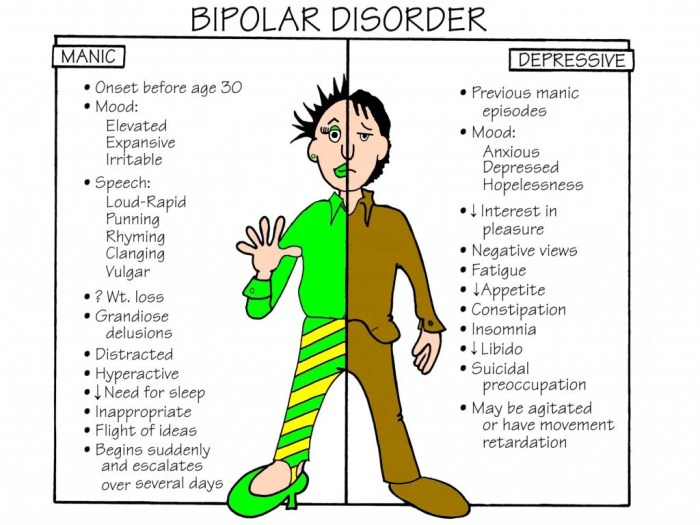
Navigating the complexities of bipolar disorder treatment often involves a delicate dance with multiple medications. While each medication plays a crucial role in stabilizing mood and managing symptoms, the potential for interactions between these drugs can significantly impact treatment efficacy and safety. Understanding these interactions is paramount for both patients and healthcare providers to optimize treatment outcomes and minimize adverse effects.Medication interactions occur when one medication alters the way another medication is absorbed, metabolized, or eliminated from the body.
This can lead to increased or decreased effects of one or both medications, potentially causing side effects or even serious complications. Therefore, a thorough understanding of potential interactions is essential for effective bipolar disorder management.
Potential Drug Interactions
A comprehensive medication history is vital to identify potential drug interactions. This includes not only prescribed medications but also over-the-counter drugs, herbal supplements, and even recreational substances. Failing to consider these factors can lead to unpredictable and potentially dangerous consequences. A complete medication history should be taken at every visit to monitor for any new or changing medications that might affect the treatment plan.
Importance of Thorough Medication History Taking
A detailed medication history is crucial for several reasons. Firstly, it allows healthcare providers to identify potential interactions between prescribed medications and other substances, both prescribed and over-the-counter. Secondly, it helps monitor for any changes in medication use that could impact treatment effectiveness or safety. Thirdly, it provides a baseline for future assessments and helps track the evolution of the patient’s overall health status.
Impact of Drug Interactions on Treatment Outcomes
Drug interactions can significantly impact treatment outcomes for bipolar disorder. For example, an interaction could lead to an inadequate response to mood stabilizers, necessitating adjustments in dosage or switching medications. Conversely, interactions can exacerbate side effects, making treatment less tolerable and potentially leading to non-adherence. In some cases, severe interactions can even lead to life-threatening complications.
Table of Potential Drug Interactions, Medications to treat bipolar disorder
| Drug Interaction | Severity | Preventative Measures |
|---|---|---|
| Lithium and NSAIDs (e.g., ibuprofen, naproxen) | Moderate to High | Use of alternative pain relievers (e.g., acetaminophen), careful monitoring of lithium levels, and close communication with the prescribing physician. |
| Antipsychotics and certain antidepressants | Moderate | Careful monitoring of symptoms, adjusting medication dosages as needed, and close communication with the prescribing physician. |
| Mood stabilizers and certain herbal supplements (e.g., St. John’s Wort) | Variable | Avoid concurrent use of herbal supplements without consultation with a healthcare provider. Providing a complete list of all supplements, vitamins, and herbal remedies to the healthcare provider. |
| Anticonvulsants and other medications that affect liver enzymes | Moderate to High | Regular monitoring of liver function tests, adjusting dosages as needed, and close communication with the prescribing physician. Carefully consider potential risks and benefits of concurrent medications. |
Long-Term Management and Considerations
Bipolar disorder is a chronic condition requiring ongoing management. Successful long-term treatment goes beyond just managing acute episodes. It encompasses a holistic approach that integrates medication, lifestyle adjustments, and consistent support. This phase focuses on preventing future relapses, improving overall well-being, and enabling individuals to lead fulfilling lives.Long-term management of bipolar disorder necessitates a dynamic approach. Medication adjustments, lifestyle modifications, and robust support systems are crucial components of this ongoing process.
The goal is not just to suppress symptoms but to empower individuals to effectively navigate the challenges of bipolar disorder and live their best possible lives.
Ongoing Monitoring and Medication Adjustments
Effective long-term management involves consistent monitoring of treatment response and symptom progression. Regular check-ups with a psychiatrist are essential to assess medication effectiveness and adjust dosages as needed. Blood tests and other assessments may be conducted to monitor for potential side effects and ensure the medication is not causing any adverse health impacts. This dynamic approach is vital for optimizing treatment outcomes and preventing potential complications.
Symptoms can fluctuate over time, requiring adjustments to medication regimens.
Lifestyle Factors in Bipolar Disorder Management
Lifestyle plays a significant role in managing bipolar disorder. A balanced diet, regular exercise, and sufficient sleep contribute significantly to mood stabilization. Maintaining a consistent sleep schedule, prioritizing stress reduction techniques such as meditation or yoga, and engaging in enjoyable activities can significantly impact mood regulation. Furthermore, establishing healthy coping mechanisms for stress is key. These factors work synergistically with medication to enhance overall well-being.
Importance of Patient Support and Mental Health Resources
Patient support and access to mental health resources are critical for long-term success in managing bipolar disorder. Support groups, therapy sessions, and access to mental health professionals provide individuals with valuable coping strategies, emotional support, and education about the condition. The availability of these resources can help reduce feelings of isolation and provide a network of understanding individuals.
The support of family and friends is equally crucial in fostering a supportive environment.
Key Factors for Long-Term Management
| Factor | Description |
|---|---|
| Medication Adherence | Taking medications as prescribed is crucial for maintaining stability. Missing doses can disrupt the therapeutic effect and increase the risk of relapse. |
| Regular Monitoring | Regular check-ups with a psychiatrist are essential to evaluate medication effectiveness and adjust dosages as needed. |
| Lifestyle Modifications | Adopting a healthy lifestyle including a balanced diet, regular exercise, and sufficient sleep can significantly improve mood regulation. |
| Stress Management Techniques | Practicing stress reduction techniques like meditation or yoga can help manage stress, which is a significant trigger for bipolar episodes. |
| Mental Health Resources | Accessing support groups, therapy, and mental health professionals provides crucial support, coping strategies, and education about the condition. |
| Family and Social Support | A supportive network of family and friends plays a vital role in providing encouragement and understanding. |
Illustrative Cases and Scenarios
Understanding bipolar disorder requires recognizing its diverse presentations. Medication strategies must be tailored to individual needs, considering the specific type and severity of the illness, as well as the patient’s unique response to treatment. Illustrative cases below highlight these complexities and the dynamic nature of bipolar disorder management.
Case 1: Rapid Cycling Bipolar Disorder
This patient, a 28-year-old woman, experiences rapid mood swings, often cycling between mania and depression within a week or even a few days. Initial treatment with a mood stabilizer, like lithium, is insufficient to control the rapid cycling. The healthcare team then adds an atypical antipsychotic, such as quetiapine, to stabilize mood and reduce the frequency and severity of manic episodes.
Close monitoring of her symptoms and medication adjustments are crucial to finding the optimal combination and dosage.
Case 2: Bipolar Disorder with Mixed Features
A 35-year-old man presents with symptoms of both mania and depression simultaneously. He experiences racing thoughts, agitation, and sleeplessness, alongside feelings of hopelessness and worthlessness. This mixed episode requires a combination therapy approach. The treatment plan might include a mood stabilizer, like valproate, alongside an antipsychotic, like olanzapine, to manage the mixed state and prevent escalation. The patient’s response to this combination therapy is closely monitored to fine-tune the medication regimen.
Case 3: Bipolar Disorder and Comorbid Anxiety
A 40-year-old female patient with bipolar disorder also suffers from generalized anxiety disorder. Her anxiety significantly impacts her ability to adhere to her medication schedule and experience relief from depressive episodes. The treatment team considers both the bipolar disorder and the anxiety when developing a personalized plan. An anti-anxiety medication, such as a selective serotonin reuptake inhibitor (SSRI), might be added to the existing mood stabilizer and antipsychotic regimen.
Evaluating Treatment Response
Monitoring a patient’s response to medication is essential. This involves regular assessments of mood, energy levels, sleep patterns, and overall functioning. Clinicians track symptoms using standardized rating scales and conduct regular follow-up appointments. Adjustments to the medication regimen are made based on these evaluations. This may involve increasing or decreasing doses, switching medications, or adding supplementary therapies.
For example, if a patient experiences significant side effects with a particular medication, the dosage might be lowered or the medication replaced with an alternative. Regular monitoring is critical to prevent adverse effects and ensure the patient’s well-being.
Ending Remarks
In conclusion, navigating the world of bipolar disorder medications requires a comprehensive understanding of various factors. This guide provides a structured overview, but remember, personalized treatment is paramount. Open communication with your healthcare provider is essential for developing a tailored strategy that addresses individual needs and potential challenges. The goal is to achieve optimal management of symptoms, improve quality of life, and foster a deeper understanding of the condition.