What is nociceptive pain? It’s pain originating from actual or potential tissue damage. This isn’t just a fleeting discomfort; it’s a complex physiological response triggered by various stimuli. From a simple burn to a persistent muscle strain, understanding the mechanisms behind nociceptive pain is crucial for effective pain management. This exploration delves into the science behind this common experience, examining everything from its causes and symptoms to diagnosis, treatment, and potential complications.
Nociceptive pain signals are transmitted via specialized nerve endings called nociceptors. These receptors are activated by noxious stimuli, ranging from extreme temperatures to pressure and chemical irritants. The process involves a cascade of events, starting with the initial stimulation and culminating in the perception of pain in the brain. Understanding these steps is key to appreciating the complexity of this fundamental human experience.
Definition and Overview

Nociceptive pain is a crucial part of our sensory system, acting as a warning signal of potential tissue damage. It’s a vital mechanism for protecting us from harm. Understanding its intricacies helps in developing effective pain management strategies.Nociceptive pain arises when specialized nerve endings, called nociceptors, detect noxious stimuli. These stimuli can range from heat and pressure to chemicals released from damaged tissue.
This signal transduction is critical in our survival.
Nociceptors and Pain Perception
Nociceptors are sensory nerve fibers that respond to potentially harmful stimuli. They are found throughout the body, encompassing skin, muscles, joints, and internal organs. Their activation initiates a cascade of events that lead to the perception of pain. Nociceptors are not static; they are dynamic and adapt to the intensity and duration of the stimulus.
Types of Nociceptive Pain
Nociceptive pain is categorized into somatic and visceral pain, based on the location of the stimulated nociceptors. Somatic pain originates from the skin, muscles, bones, and joints, while visceral pain arises from internal organs. These differences in location significantly influence the characteristics of the pain.
Nociceptive pain, basically, is your body’s way of telling you something’s wrong. It’s the signal that alerts you to potential tissue damage, like a burn or a cut. Understanding this is crucial because it’s linked to your rights, including your right to leave the hospital if you feel you’re recovering well enough. Ultimately, knowing what nociceptive pain is can empower you to make informed decisions about your health and well-being.
Physiological Mechanisms of Nociceptive Pain Transmission, What is nociceptive pain
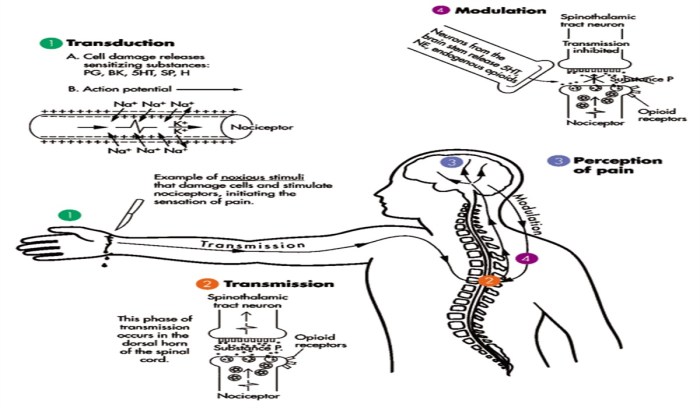
Nociceptive pain transmission involves a complex series of events. The noxious stimulus triggers the activation of nociceptors, leading to the generation of action potentials. These electrical signals travel along sensory neurons to the spinal cord. Neurotransmitters, such as substance P, are released, facilitating the transmission of the pain signal to the brain. The process is meticulously orchestrated to provide a comprehensive pain response.
Stages of Nociceptive Pain Processing
The following flowchart Artikels the stages involved in nociceptive pain processing:
Nociceptive Pain Processing Flowchart [Stimulus] --> [Nociceptor Activation] --> [Action Potential Generation] --> [Signal Transmission to Spinal Cord] --> [Synaptic Transmission] --> [Ascending Pathways to Brain] --> [Pain Perception in Brain]
Comparison of Somatic and Visceral Pain
| Characteristic | Somatic Pain | Visceral Pain |
|---|---|---|
| Location | Skin, muscles, bones, joints | Internal organs |
| Quality | Sharp, localized | Dull, aching, poorly localized |
| Referral | Usually localized to the site of injury | Often referred to a different area of the body |
| Examples | Cut, bruise, muscle strain | Appendicitis, pancreatitis, organ ischemia |
Note: Pain referral is a phenomenon where pain originating from an internal organ is perceived as coming from a different area of the body.
This is due to the convergence of visceral and somatic afferent pathways in the spinal cord. Understanding referral patterns is crucial for accurate diagnosis and treatment.
Causes and Triggers
Nociceptive pain, a vital protective mechanism, arises from the activation of specialized nerve endings called nociceptors. Understanding the triggers and underlying causes is crucial for effective pain management. This process often involves tissue damage, but not always. This section delves into the common causes, stimuli, and factors influencing the intensity and duration of this type of pain.
Nociceptive pain is a response to harmful stimuli, and the intensity of the pain often correlates with the severity of the stimulus. The pathway involves the transduction of the stimulus into a neural signal, transmission along sensory nerves, and interpretation in the brain. Different types of stimuli can activate nociceptors, leading to a spectrum of pain experiences.
Common Causes of Nociceptive Pain
Various factors can initiate nociceptive pain signals. Direct physical injury, such as cuts, burns, or fractures, frequently leads to the activation of nociceptors. However, even non-traumatic conditions like inflammation and infection can trigger this pain response.
Stimuli Activating Nociceptors
Nociceptors are activated by a variety of stimuli. These include mechanical stimuli, such as pressure or stretching beyond normal limits. Thermal stimuli, like extreme heat or cold, can also trigger nociceptor activation. Chemical stimuli, including substances released during inflammation or tissue damage, are another important category. Examples include histamine, prostaglandins, and potassium ions.
Tissue Damage and Nociceptive Pain
A strong correlation exists between tissue damage and the experience of nociceptive pain. Damaged tissues release chemicals that stimulate nociceptors, initiating the pain signal. The extent of tissue damage directly influences the intensity and duration of the pain. For example, a minor cut will likely result in acute pain that subsides quickly, while a severe burn might lead to chronic pain lasting for weeks or months.
Factors Influencing Pain Intensity and Duration
Several factors modulate the intensity and duration of nociceptive pain. These include the individual’s pain threshold, their perception of the pain, and their overall health condition. For instance, individuals with a lower pain threshold may experience more intense pain than those with a higher one for the same level of stimulus. Psychological factors, such as stress and anxiety, can also influence the perception of pain.
Acute vs. Chronic Nociceptive Pain
Acute nociceptive pain is a short-term response to a specific injury or stimulus. Chronic nociceptive pain, on the other hand, persists for an extended period, often exceeding the expected healing time. The underlying causes and contributing factors can vary considerably. For instance, acute pain may result from a sprained ankle, while chronic pain could stem from osteoarthritis.
Types of Tissue Damage Triggering Nociceptive Pain
| Type of Tissue Damage | Description |
|---|---|
| Cuts and lacerations | Breaks in the skin and underlying tissues. |
| Burns | Damage to tissues caused by heat, chemicals, or electricity. |
| Fractures | Broken bones. |
| Muscle strains and sprains | Overstretching or tearing of muscles or ligaments. |
| Inflammation | Body’s response to injury or infection, characterized by swelling, redness, and pain. |
| Infections | Invasion of harmful microorganisms, resulting in local tissue damage. |
Symptoms and Manifestations: What Is Nociceptive Pain
Nociceptive pain, a vital protective mechanism, presents itself in a wide array of ways, depending on the source and location of the injury or stimulus. Understanding these manifestations is crucial for accurate diagnosis and effective treatment. Recognizing the specific symptoms and how they vary among individuals can greatly assist healthcare professionals in pinpointing the cause of the pain.
Nociceptive pain, essentially, is your body’s way of telling you something’s wrong. It’s a signal that a tissue is being damaged, like a burn or a cut. Understanding this is crucial, especially when considering diagnostic tools like capsule endoscopy for celiac disease diagnosis. This procedure helps pinpoint issues within the small intestine, which can be a source of pain in certain conditions.
So, while nociceptive pain is a vital feedback mechanism, it’s also important to find the root cause for effective treatment.
Different individuals experience nociceptive pain with varying intensities and qualities. Factors such as the underlying cause, the individual’s pain threshold, and even psychological factors play significant roles in shaping the experience. This complex interplay emphasizes the importance of a holistic approach to pain management.
Common Symptoms
Nociceptive pain is often characterized by a range of sensations, from dull aches to sharp, throbbing pains. These sensations can be localized to a specific area or spread throughout a larger region. The severity of the symptoms can fluctuate, influenced by factors such as activity levels, stress, and sleep quality. For example, a sprained ankle might cause sharp, localized pain that intensifies with movement, whereas a muscle strain could manifest as a dull ache in a broader area.
Examples of Manifestations
Nociceptive pain can manifest in various ways depending on the source and individual. A patient experiencing pain from a toothache might describe a sharp, throbbing pain localized to the affected tooth, while someone with a pulled hamstring might report a dull ache and stiffness in the back of their thigh. These examples illustrate the diverse ways in which nociceptive pain can be expressed.
Pain Intensity and Location
The intensity of nociceptive pain can vary considerably. It can range from mild discomfort to severe agony, influencing daily activities and quality of life. The location of the pain is crucial for diagnosis. For example, pain in the chest might be a sign of a heart condition or muscle strain, while pain in the abdomen could indicate a variety of digestive issues.
Precise localization assists healthcare professionals in identifying the potential cause. A patient experiencing pain in their left lower quadrant of the abdomen, for instance, might be more prone to having an appendicitis than if the pain was localized to the upper right quadrant.
Psychological Factors
Psychological factors can significantly influence the perception and experience of nociceptive pain. Stress, anxiety, and depression can exacerbate pain signals, leading to a more intense and prolonged experience. Conversely, a positive outlook and coping mechanisms can help manage pain more effectively. For instance, a person with a history of anxiety might perceive a minor injury as more painful than someone who is more resilient to stress.
Individual Reporting of Pain
Individuals report nociceptive pain in diverse ways. Some might use precise descriptors, like “sharp,” “stabbing,” or “throbbing,” while others might use more general terms, like “ache” or “discomfort.” The use of visual analog scales (VAS) or numerical rating scales (NRS) can help quantify the pain intensity, providing a more objective measure for clinicians. This variety highlights the importance of open communication between patients and healthcare professionals to ensure accurate pain assessment.
Categorization of Nociceptive Pain Symptoms by Body Region
| Body Region | Potential Symptoms |
|---|---|
| Head | Headaches, migraines, toothaches, facial pain |
| Neck | Stiffness, pain, muscle spasms, radiating pain |
| Back | Lower back pain, upper back pain, sciatica |
| Shoulders | Shoulder pain, impingement, rotator cuff injuries |
| Arms | Elbow pain, wrist pain, hand pain, carpal tunnel syndrome |
| Legs | Knee pain, ankle pain, foot pain, muscle strains |
| Abdomen | Cramps, bloating, sharp pain, dull ache |
| Chest | Chest pain, pressure, tightness, radiating pain |
| Pelvis | Pelvic pain, hip pain, groin pain |
This table provides a general overview of potential symptoms associated with nociceptive pain in various body regions. It is not exhaustive, and specific symptoms may vary greatly depending on the underlying cause. Consulting with a healthcare professional is crucial for accurate diagnosis and treatment.
Diagnosis and Assessment
Understanding nociceptive pain requires a meticulous diagnostic approach that goes beyond simply identifying the pain location. Accurate diagnosis hinges on a comprehensive evaluation of the patient’s history, physical examination findings, and potentially, imaging studies. This process aims to pinpoint the source of the pain and guide appropriate treatment strategies.
Patient History
A detailed patient history is crucial in diagnosing nociceptive pain. This involves gathering information about the onset, duration, location, and character of the pain. Understanding the patient’s medical history, including past injuries, surgeries, and chronic conditions, is also essential. Factors such as recent activities, lifestyle, and environmental exposures can provide valuable clues.
Questions to Ask a Patient
The following questions can help in eliciting crucial information about the pain:
- When did the pain start?
- Where is the pain located?
- What does the pain feel like (e.g., sharp, dull, aching)?
- How intense is the pain on a scale of 0 to 10?
- What makes the pain better or worse?
- What treatments have been tried already, and what was the outcome?
- Does the pain radiate to any other areas?
- Have there been any recent injuries or trauma?
- Are there any associated symptoms, such as swelling, redness, or fever?
- What is the patient’s overall health and lifestyle?
Physical Examination
A thorough physical examination is vital for assessing the source and extent of nociceptive pain. This may involve inspection, palpation, range of motion assessments, and neurological testing. Specific areas of focus might include the affected joint, muscle, or tissue. For example, a patient with suspected back pain would undergo a detailed assessment of the spine, including palpation of the vertebrae, assessment of spinal mobility, and neurological checks for signs of nerve impingement.
The examination helps in identifying potential physical abnormalities or limitations that contribute to the pain.
Imaging Techniques
Imaging techniques, such as X-rays, CT scans, and MRIs, play a significant role in diagnosing nociceptive pain. X-rays are useful for visualizing bone structures and detecting fractures or dislocations. CT scans provide detailed cross-sectional views of the body, aiding in identifying soft tissue abnormalities or internal injuries. MRIs offer excellent soft tissue contrast, enabling the visualization of nerves, muscles, ligaments, and tendons.
These techniques help identify the underlying cause of pain, such as a herniated disc or a bone spur. For example, an MRI might reveal a meniscal tear in the knee, explaining a patient’s knee pain.
Diagnostic Criteria for Nociceptive Pain
The diagnostic criteria for nociceptive pain vary based on the specific anatomical location and potential causes. A comprehensive approach considers the clinical presentation, imaging findings, and patient history to reach an accurate diagnosis. The following table provides a summary of diagnostic criteria for some common types of nociceptive pain:
| Type of Nociceptive Pain | Diagnostic Criteria |
|---|---|
| Musculoskeletal Pain (e.g., back pain, joint pain) | History of trauma or overuse; localized tenderness; limited range of motion; imaging findings of joint or bone abnormalities. |
| Neuropathic Pain | Pain originating from damaged or diseased nerves; often described as burning, shooting, or tingling; neurological examination may reveal sensory deficits or abnormalities. |
| Visceral Pain | Pain originating from internal organs; often described as deep, aching, or cramping; associated with organ-specific symptoms (e.g., nausea, vomiting, fever). |
| Somatic Pain | Pain originating from skin, muscles, bones, or joints; characterized by localized tenderness and pain; often associated with physical injury. |
Treatment and Management
Managing nociceptive pain effectively involves a multifaceted approach tailored to the individual patient. Successful treatment hinges on understanding the underlying cause, the patient’s response to different interventions, and a commitment to ongoing care. This approach emphasizes both pharmacological and non-pharmacological strategies, with a strong focus on patient education and self-management.
Effective pain management requires a collaborative effort between the patient, healthcare provider, and other support personnel. This collaborative effort promotes a comprehensive understanding of the pain experience, enabling the development of a personalized treatment plan that considers individual needs and preferences.
Pharmacological Interventions
Pharmacological interventions are often the cornerstone of nociceptive pain management. Analgesics, in various forms and strengths, aim to reduce the sensation of pain by acting on the nervous system. Different types of analgesics target different pain pathways, allowing for personalized treatment strategies.
- Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen and naproxen are frequently used for mild to moderate pain, offering anti-inflammatory effects alongside analgesic properties. They are generally well-tolerated but may cause gastrointestinal upset in some individuals.
- Acetaminophen (paracetamol) is another commonly prescribed analgesic, known for its relatively low risk of side effects compared to NSAIDs. However, its effectiveness for severe pain may be limited.
- Opioids, such as codeine and morphine, are reserved for moderate to severe pain that does not respond to other treatments. Their use requires careful monitoring due to the potential for addiction and respiratory depression.
- Adjuvant analgesics, such as antidepressants or anticonvulsants, can be used in conjunction with other medications to enhance pain relief, particularly when neuropathic pain components are present.
Non-Pharmacological Approaches
Non-pharmacological interventions play a vital role in comprehensive pain management. These approaches often address the underlying cause or contributing factors and aim to improve function and quality of life.
- Physical therapy (PT) is a valuable tool in managing nociceptive pain. PT interventions focus on restoring mobility, improving strength, and reducing inflammation through exercises, manual therapy, and other modalities. For example, a patient experiencing back pain might undergo exercises to strengthen core muscles and improve posture.
- Heat and cold therapy can provide temporary relief from pain and inflammation. Heat promotes blood flow, while cold reduces inflammation and muscle spasms.
- Relaxation techniques, such as deep breathing and meditation, can help manage pain by reducing stress and promoting relaxation. Mindfulness-based stress reduction (MBSR) programs have demonstrated effectiveness in chronic pain management.
- Lifestyle modifications, including maintaining a healthy weight, getting regular exercise (within pain tolerance), and adopting a balanced diet, are important for overall health and can contribute to managing nociceptive pain.
Supportive Care
Supportive care involves addressing the emotional and social needs of patients experiencing nociceptive pain. This is crucial for overall well-being and treatment adherence.
- Patient education is paramount. Educating patients about their condition, treatment options, and potential side effects empowers them to actively participate in their care. This includes understanding the rationale behind the prescribed medications and the importance of adherence to the treatment plan.
- Counseling and support groups can provide emotional support and coping strategies for patients dealing with chronic pain. Sharing experiences with others facing similar challenges can foster a sense of community and resilience.
- Addressing any underlying psychological factors, such as anxiety or depression, that may exacerbate the pain experience is critical. Therapy can help patients develop coping mechanisms and improve overall well-being.
Patient Education and Self-Management
Empowering patients with knowledge about their condition and the tools for self-management is crucial. This fosters a proactive role in their recovery and long-term well-being.
- Providing clear and concise information about the nature of nociceptive pain, its causes, and its potential treatment options helps patients understand their condition better.
- Teaching patients self-management strategies, including pain monitoring, activity pacing, and relaxation techniques, can improve their ability to cope with and manage their pain effectively.
- Encouraging patient participation in developing and implementing their treatment plan promotes a sense of ownership and responsibility for their well-being.
Treatment Modalities Comparison
| Treatment Modality | Pros | Cons |
|---|---|---|
| NSAIDs | Effective for mild to moderate pain; often well-tolerated; relatively inexpensive. | Potential for gastrointestinal side effects; may not be suitable for individuals with certain medical conditions. |
| Acetaminophen | Generally well-tolerated; lower risk of side effects than NSAIDs; effective for mild to moderate pain. | May not be as effective for severe pain as other options. |
| Opioids | Effective for severe pain that doesn’t respond to other treatments. | Potential for addiction, respiratory depression, and other side effects; requires careful monitoring. |
| Physical Therapy | Addresses the underlying cause of pain; improves function and mobility; often improves quality of life. | May require time commitment; may not be suitable for all individuals or types of pain. |
| Heat/Cold Therapy | Provides temporary relief from pain and inflammation. | Limited duration of relief; may not be effective for all types of pain. |
Illustrative Case Studies
Understanding nociceptive pain requires exploring real-world examples. Case studies provide valuable insights into the diverse presentations, progressions, and management strategies for this type of pain. These examples illuminate the complexities of pain and highlight the importance of personalized care.
Acute Nociceptive Pain Case Study
A 28-year-old construction worker experienced sudden, sharp pain in his right ankle after a fall on a construction site. The pain was localized to the ankle and intensified with movement. The pain was described as a throbbing, burning sensation, rated as 8/10 on a numerical pain scale. Physical examination revealed swelling, bruising, and tenderness around the ankle joint.
Diagnostic imaging (X-ray) confirmed a fracture of the lateral malleolus. The pain was successfully managed with rest, ice, compression, elevation (RICE), pain medication, and eventually surgical intervention to repair the fracture.
Chronic Nociceptive Pain Progression
A 55-year-old woman with a history of osteoarthritis experienced gradual worsening of knee pain over several years. Initially, the pain was mild and intermittent, occurring primarily after prolonged periods of activity. Over time, the pain became more severe, persistent, and interfered with daily activities. She developed stiffness, limited range of motion, and a decreased quality of life. The pain was frequently associated with sleep disturbances and emotional distress.
Management strategies included physical therapy, medication adjustments, and assistive devices. Regular follow-up with specialists to manage pain, and address potential complications like joint deformities, were essential to maintain quality of life.
Nociceptive pain is basically your body’s way of telling you something’s wrong, like a burn or a bruise. It’s often sharp and localized, a signal that tissue damage is happening. Understanding this can be helpful in exploring conditions like insulin resistance, which can sometimes lead to chronic pain, and even progress to diabetes, affecting how the body manages glucose and leading to issues with nerve function.
For a deeper dive into the nuances of insulin resistance versus diabetes, check out this helpful resource: insulin resistance vs diabetes. Ultimately, though, nociceptive pain is a crucial part of our body’s defense mechanisms, highlighting the need for rest and healing.
Impact of Treatment on Pain Management
A 62-year-old man with chronic back pain from a herniated disc experienced significant relief after undergoing a multidisciplinary pain management program. The program integrated physical therapy, cognitive behavioral therapy (CBT), and medication adjustments. CBT helped him manage stress and develop coping mechanisms for pain. Physical therapy focused on strengthening core muscles and improving posture. Medication was used to manage pain and inflammation.
As a result, the patient reported a substantial reduction in pain intensity, improved sleep quality, and a significant increase in functional ability. He was able to return to many of his hobbies.
Importance of Interdisciplinary Care
Managing nociceptive pain effectively often necessitates a collaborative approach. A patient with complex pain conditions, for example, might require input from various healthcare professionals, including physicians, physical therapists, psychologists, and pain specialists. This collaborative approach allows for a comprehensive assessment of the patient’s needs and the development of a tailored treatment plan. It facilitates effective communication and coordination among healthcare providers, resulting in more holistic and personalized care.
Patient Journey and Treatment Outcomes
A 30-year-old woman experiencing chronic pain after a car accident underwent a comprehensive treatment program. The program involved a phased approach that included medication, physical therapy, psychological support, and lifestyle modifications. The initial phase focused on pain reduction and functional restoration. The subsequent phase focused on managing pain flares and improving overall well-being. The patient’s progress was monitored regularly, and the treatment plan was adjusted as needed.
Ultimately, the patient achieved a significant reduction in pain, improved mobility, and a return to a more fulfilling lifestyle.
Summary Table of Case Studies
| Case Study | Pain Type | Duration | Treatment Approach | Outcome |
|---|---|---|---|---|
| Acute Ankle Fracture | Acute nociceptive | Short-term | RICE, medication, surgery | Pain relief, fracture repair |
| Chronic Knee Osteoarthritis | Chronic nociceptive | Long-term | Physical therapy, medication, assistive devices | Improved function, maintained quality of life |
| Herniated Disc Back Pain | Chronic nociceptive | Long-term | Multidisciplinary pain management | Significant pain reduction, improved function |
| Post-Accident Chronic Pain | Chronic nociceptive | Long-term | Comprehensive, phased treatment program | Pain reduction, improved mobility, improved lifestyle |
Potential Complications and Prevention
Nociceptive pain, while often a response to injury or tissue damage, can sometimes lead to secondary complications if not managed effectively. Understanding these potential problems and implementing proactive strategies for prevention is crucial for optimal patient outcomes. Early intervention and treatment play a vital role in mitigating these issues, and preventative care is key to minimizing the long-term impact of pain.
Potential Complications of Nociceptive Pain
Nociceptive pain, while a natural response to harm, can unfortunately lead to various complications if left unaddressed. These complications can range from physical limitations to psychological distress. Chronic pain, for instance, can significantly impact daily activities, social interactions, and overall well-being.
Strategies for Preventing Complications
Proactive measures are essential to prevent the development and progression of complications associated with nociceptive pain. Early and effective pain management strategies, including medication, physical therapy, and lifestyle modifications, are vital.
- Early Intervention: Prompt diagnosis and treatment are paramount in preventing complications. Delaying treatment can exacerbate pain, leading to a cascade of problems, such as muscle weakness, stiffness, and reduced mobility.
- Multidisciplinary Approach: A collaborative approach involving physicians, physical therapists, psychologists, and other healthcare professionals can provide comprehensive care. This holistic approach addresses the physical, emotional, and social aspects of pain management, thereby improving overall outcomes.
- Patient Education: Empowering patients with knowledge about their condition and treatment options can foster active participation in their care. This includes understanding the importance of adherence to medication schedules, physical therapy exercises, and lifestyle adjustments.
- Stress Management Techniques: Chronic pain can significantly impact mental health. Incorporating stress-reduction techniques, such as mindfulness, yoga, or meditation, can help manage emotional distress and improve coping mechanisms.
Importance of Early Intervention and Treatment
Early intervention and treatment are critical in preventing long-term complications. Early diagnosis and treatment can limit the severity of pain and reduce the risk of secondary issues. For example, timely intervention for a back injury can prevent the development of chronic pain and disability.
Mitigating Complications Through Proactive Measures
Proactive measures can significantly reduce the risk of complications associated with nociceptive pain. These measures encompass early diagnosis, effective pain management strategies, and comprehensive care. Implementing preventative care strategies is key to minimizing pain-related issues. Physical therapy, occupational therapy, and counseling are all examples of proactive measures.
Role of Preventative Care in Reducing Pain-Related Issues
Preventative care plays a crucial role in minimizing the risk of pain-related complications. This includes regular check-ups, maintaining a healthy lifestyle, and adopting injury-prevention strategies. For example, proper lifting techniques can prevent back injuries.
Table: Link Between Complications and Nociceptive Pain Severity
| Nociceptive Pain Severity | Potential Complications |
|---|---|
| Mild | Limited joint mobility, occasional muscle stiffness, temporary sleep disturbance |
| Moderate | Chronic pain, reduced physical activity, decreased quality of life, increased risk of depression or anxiety |
| Severe | Significant disability, chronic pain syndrome, substantial limitations in daily activities, potentially life-altering health issues, dependence on others for basic needs |
Future Directions and Research
Unraveling the complexities of nociceptive pain requires a multifaceted approach, incorporating advancements in neuroscience, pharmacology, and technology. This section explores emerging research avenues, highlighting knowledge gaps and potential solutions for improved pain management. Future research will likely focus on refining diagnostic tools, developing targeted therapies, and leveraging technological innovations to enhance patient outcomes.
Latest Research Advancements
Significant progress has been made in understanding the intricate neural pathways involved in nociceptive pain transmission. Studies utilizing advanced neuroimaging techniques, such as functional magnetic resonance imaging (fMRI), have provided valuable insights into the brain regions activated during pain perception. These advancements are paving the way for more precise diagnostic criteria and personalized treatment strategies. For example, researchers are now able to identify specific neural patterns associated with different types of nociceptive pain, allowing for more accurate classification and targeted interventions.
Current Gaps in Knowledge
Despite the progress, significant knowledge gaps remain concerning the mechanisms underlying chronic nociceptive pain. The transition from acute to chronic pain, a crucial aspect of many pain conditions, is not fully understood. Further research is needed to delineate the specific molecular and cellular changes that contribute to the chronification of pain signals. Moreover, the individual variability in pain perception and response to treatment remains a considerable challenge.
Understanding these factors is essential for developing personalized pain management strategies.
Potential Future Directions for Research
Future research should focus on identifying novel therapeutic targets. This includes exploring the role of specific neurotransmitters, neuromodulators, and inflammatory pathways in chronic pain conditions. Furthermore, research into the interplay between the nervous system and the immune system in the development and maintenance of pain is expected to yield significant insights. For instance, investigations into the role of the gut microbiome in modulating pain responses may offer novel therapeutic avenues.
Promising Areas of Investigation
One promising area is the development of novel analgesic drugs targeting specific pain pathways. The use of gene therapy and stem cell technology is also gaining traction as potential therapeutic interventions. Moreover, the study of non-pharmacological interventions, such as mindfulness-based stress reduction and physical therapy, holds significant potential for enhancing pain management strategies.
Impact of New Technologies on Pain Management
Advancements in technology are revolutionizing pain management. Wearable sensors and biofeedback devices allow for real-time monitoring of pain intensity and physiological responses. These technologies can provide valuable data for personalized pain management plans and facilitate early detection of pain flares. Furthermore, virtual reality (VR) and augmented reality (AR) technologies are being explored as potential tools for pain distraction and rehabilitation.
Table of Current Research Initiatives
| Research Initiative | Focus Area | Potential Impact |
|---|---|---|
| Development of novel analgesic drugs targeting specific pain pathways | Pharmacology | Improved efficacy and reduced side effects of pain treatments |
| Investigation of the interplay between the nervous system and the immune system in chronic pain | Neuroscience/Immunology | Identification of novel therapeutic targets and personalized treatment strategies |
| Clinical trials using VR/AR for pain distraction and rehabilitation | Technology-based interventions | Enhanced pain management strategies for patients with chronic pain |
| Research into the role of the gut microbiome in modulating pain responses | Gastroenterology/Neuroscience | Identification of novel therapeutic targets for chronic pain |
Outcome Summary
In conclusion, nociceptive pain, a fundamental aspect of human experience, is a complex interplay of physiological and psychological factors. From its origins in tissue damage to the intricate pathways of pain perception, this overview highlights the multifaceted nature of this experience. Understanding the different types, causes, and management strategies for nociceptive pain is essential for effective patient care and improving overall well-being.

