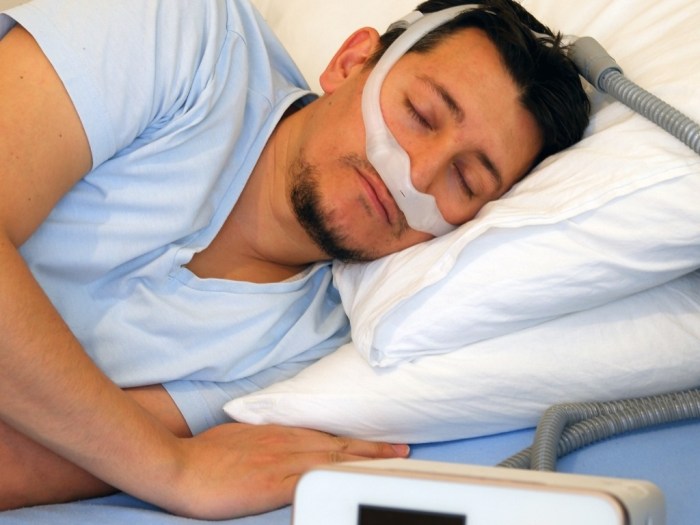
What is the difference between CPAP and BiPAP? Understanding these two therapies is crucial for anyone struggling with sleep apnea. CPAP and BiPAP machines deliver pressurized air to keep your airways open during sleep, preventing interruptions to your breathing. However, they differ in how they achieve this, leading to distinct advantages and disadvantages for different patients.
This guide delves into the specifics of CPAP and BiPAP, comparing their pressure settings, treatment applications, and user experiences. We’ll explore which type of machine might be best suited for you, based on your sleep apnea severity and individual needs. It’s important to remember that the best choice should always be determined by a healthcare professional after a thorough evaluation.
Introduction to CPAP and BiPAP
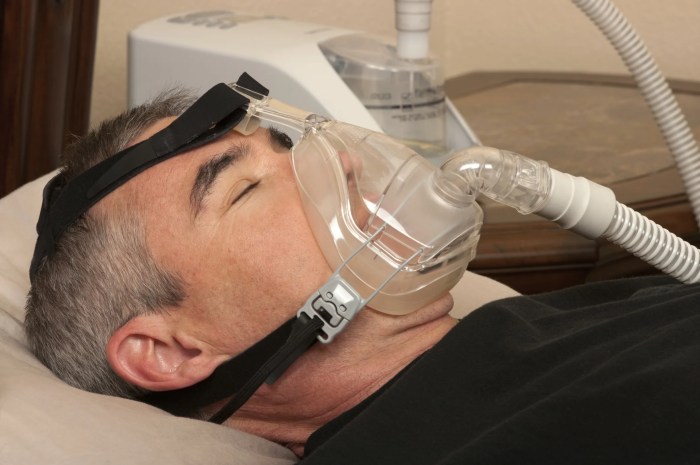
CPAP and BiPAP are two common types of positive airway pressure (PAP) therapy used to treat sleep apnea. Sleep apnea is a sleep disorder characterized by pauses in breathing during sleep. These pauses can significantly reduce the amount of oxygen reaching the body, leading to various health problems. Both CPAP and BiPAP machines deliver pressurized air to keep the airways open during sleep, preventing these breathing interruptions.
Understanding the differences between these therapies is crucial for patients to choose the most effective treatment for their specific needs.These therapies work by applying a gentle, constant or varying pressure to the airway, preventing collapse during sleep. This pressure keeps the airways open, allowing for uninterrupted breathing and the proper exchange of oxygen and carbon dioxide. This ultimately improves sleep quality and overall health.
CPAP and BiPAP machines are both used to help with breathing issues, but they differ in their pressure delivery. Understanding these differences is crucial, but sometimes weight loss when sick can also affect breathing patterns, making it even more important to understand the nuances of these machines. Ultimately, consulting a doctor to determine the right machine for your specific needs is key to managing breathing problems effectively.
CPAP Therapy
CPAP, or Continuous Positive Airway Pressure, delivers a constant stream of pressurized air to the airway throughout the entire breathing cycle. The pressure is set by a doctor based on individual needs. CPAP is generally well-suited for individuals with mild to moderate sleep apnea.
BiPAP Therapy
BiPAP, or Bilevel Positive Airway Pressure, delivers two different pressures during the breathing cycle. One pressure is used during inhalation (Inspiratory Positive Airway Pressure, or IPAP), and a lower pressure is used during exhalation (Expiratory Positive Airway Pressure, or EPAP). This allows for a more natural breathing pattern and can be more comfortable for some patients, particularly those with more severe sleep apnea.
Basic Mechanics of CPAP and BiPAP Machines
CPAP machines generate a continuous flow of air at a pre-set pressure, which is delivered through a mask covering the nose and/or mouth. The pressure forces the airway open, preventing it from collapsing. BiPAP machines, on the other hand, deliver varying pressures during inhalation and exhalation. The higher pressure during inhalation helps to open the airways more effectively, and the lower pressure during exhalation helps to facilitate easier exhalation.
Comparison of CPAP and BiPAP Machines
| Feature | CPAP | BiPAP |
|---|---|---|
| Pressure Setting | Single, constant pressure | Two different pressures (IPAP/EPAP) |
| Airflow | Continuous flow | Variable flow |
| Suitability | Mild to moderate sleep apnea | Moderate to severe sleep apnea |
This table highlights the key differences in pressure and airflow between the two machines, aiding in determining which therapy is best suited for a given patient’s condition.
Ever wondered about the difference between CPAP and BiPAP machines? They both help with breathing issues, but BiPAP offers more support, adjusting pressure for inhaling and exhaling. Knowing this can be helpful, especially if you’re researching treatment options for conditions like the various types of ovarian cancer. For example, if you’re looking for comprehensive information on different ovarian cancer types, check out this resource: types of ovarian cancer.
Ultimately, the best choice between CPAP and BiPAP depends on individual needs and breathing patterns.
Key Differences in Pressure Settings: What Is The Difference Between Cpap And Bipap
CPAP and BiPAP machines both deliver pressurized air to help with breathing during sleep, but their pressure delivery systems differ significantly. This difference in pressure delivery is crucial in managing sleep apnea and achieving optimal treatment results. Understanding the varying pressure settings is essential for both patients and healthcare providers to ensure the therapy is effective and comfortable.
Pressure Settings and Air Delivery
The key difference between CPAP and BiPAP lies in the pressure settings and how they deliver air. CPAP, or Continuous Positive Airway Pressure, maintains a constant pressure throughout the entire breathing cycle. BiPAP, or Bilevel Positive Airway Pressure, delivers two different pressures: an inspiratory pressure (IPAP) during inhalation and an expiratory pressure (EPAP) during exhalation. This dual-pressure approach allows for a more natural breathing pattern, as it mimics the natural pressure fluctuations during respiration.
Pressure Ranges and Sleep Apnea Severity
The pressure settings used in CPAP and BiPAP machines are adjusted based on the severity of sleep apnea. The severity of sleep apnea is typically assessed through a sleep study. This assessment provides vital data to determine the appropriate pressure settings for each individual.
| Sleep Apnea Severity | CPAP Pressure Range (cmH2O) | BiPAP Pressure Range (cmH2O) |
|---|---|---|
| Mild | 5-10 | 8-12 (IPAP/EPAP) |
| Moderate | 10-15 | 10-15 (IPAP/EPAP) |
| Severe | 15+ | 12+ (IPAP/EPAP) |
Different pressure ranges for CPAP and BiPAP machines are tailored to different sleep apnea severities. For instance, a patient with mild sleep apnea might benefit from a CPAP pressure of 7 cmH2O, while a patient with severe sleep apnea might require a CPAP pressure of 18 cmH2O. Similarly, in BiPAP therapy, adjusting IPAP and EPAP pressures based on the severity allows for a more customized approach to respiratory support.
Impact on Therapy Effectiveness
The pressure differences significantly impact the effectiveness of each therapy. In CPAP, a constant pressure helps to keep the airway open throughout the breathing cycle. This constant pressure is effective in preventing airway collapse, particularly during sleep. In BiPAP, the variable pressures allow for a more natural breathing pattern, which can be more comfortable for some patients.
The tailored pressures also offer more support during inhalation and exhalation. For example, a patient with a higher inspiratory pressure requirement might experience better airflow and improved sleep quality using BiPAP compared to CPAP. Furthermore, patients with more complex breathing patterns might benefit more from BiPAP’s variable pressures to adjust to these fluctuations.
Treatment Applications and Patient Needs
Choosing between CPAP and BiPAP depends heavily on the specific needs of the patient. Understanding the types of sleep apnea each therapy addresses, individual patient factors, and the role of physician evaluation is crucial for optimal treatment selection. This section delves into these aspects, providing examples and considerations for diverse patient profiles.
Types of Sleep Apnea Addressed by Each Therapy
CPAP is generally the first-line treatment for mild to moderate obstructive sleep apnea (OSA). BiPAP is often considered for more severe cases or when CPAP isn’t well-tolerated. Central sleep apnea (CSA), a condition where the brain fails to send signals to the muscles controlling breathing, can also be treated with BiPAP, as it can help regulate breathing patterns throughout the night.
Furthermore, patients with complex medical conditions, such as heart failure or chronic obstructive pulmonary disease (COPD), may require BiPAP for improved respiratory support.
Patient Factors Influencing Therapy Choice
Several patient factors play a significant role in determining the most suitable therapy. These include the severity of sleep apnea, the patient’s tolerance to CPAP pressure, and any underlying medical conditions. For instance, a patient with a history of nasal congestion or other anatomical factors affecting airflow may find BiPAP more comfortable. Similarly, patients with respiratory issues beyond sleep apnea, like COPD, might benefit from BiPAP’s adjustable pressure settings.
Additionally, a patient’s overall health status and their willingness to comply with the treatment plan are crucial considerations.
CPAP and BiPAP machines are both used to help with breathing issues, but they differ in their delivery of air pressure. Understanding these subtle differences is key for anyone needing this kind of support. However, sometimes, more serious issues like parasitic infections of the central nervous system parasitic infections of the central nervous system can also impact breathing.
Thankfully, with proper diagnosis and treatment, these conditions can be managed, allowing for a return to a more comfortable breathing pattern, and helping you understand the finer points of CPAP and BiPAP. Ultimately, consulting a healthcare professional is essential for determining the most suitable treatment plan for individual needs.
Role of Physician Evaluation in Selecting the Appropriate Therapy
A thorough sleep study, often involving overnight monitoring of breathing and brain activity, is essential for accurate diagnosis and personalized treatment recommendations. Physicians evaluate the severity of the sleep apnea, considering factors such as the apnea-hypopnea index (AHI), and the patient’s overall health. This evaluation guides the choice between CPAP and BiPAP, ensuring the most effective and well-tolerated therapy.
Patient Scenarios Where One Therapy Might Be Preferred Over the Other
A patient with mild OSA might find CPAP sufficient and well-tolerated, experiencing significant improvement in sleep quality and daytime alertness. Conversely, a patient with moderate to severe OSA, or a patient who experiences significant mask discomfort or pressure intolerance with CPAP, may benefit more from BiPAP’s ability to deliver varying pressures during inhalation and exhalation. Similarly, a patient with COPD might find BiPAP’s adjustable pressure settings to be more supportive of their respiratory needs.
Considerations for Patients with Specific Medical Conditions or Anatomical Features
Patients with nasal congestion, facial deformities, or other anatomical issues impacting airflow may find BiPAP more comfortable due to its adjustable pressure settings. Furthermore, patients with certain medical conditions, like heart failure or neuromuscular disorders, may need BiPAP’s more tailored pressure support to address their specific respiratory requirements. For instance, a patient with a history of respiratory complications might benefit from the pressure control provided by BiPAP.
Summary of Ideal Patient Profiles
| Feature | CPAP | BiPAP |
|---|---|---|
| Ideal Patient Type | Patients with mild to moderate sleep apnea | Patients with moderate to severe sleep apnea, or patients with difficulty tolerating CPAP |
| Potential Challenges | Mask discomfort, pressure intolerance, nasal dryness | Potential for higher cost, potential for machine complexity |
Machine Functionality and User Experience
CPAP and BiPAP machines, while both serving the crucial purpose of improving sleep apnea, differ significantly in their functionality and user experience. Understanding these differences can greatly influence patient comfort and treatment adherence. This section dives deep into the specifics of each machine’s components, user-friendliness, available masks, and crucial aspects like mask fitting.The choice between CPAP and BiPAP is often a personalized one, guided by individual needs and preferences.
A comprehensive understanding of the machines’ characteristics empowers patients and healthcare professionals to make well-informed decisions.
Machine Components and Functions
CPAP machines deliver a constant stream of air pressure to keep the airways open during sleep. BiPAP machines, on the other hand, offer two different pressure levels – one for inhalation and another for exhalation. This allows for a more natural breathing pattern. CPAP machines typically consist of a compressor, a pressure regulator, a flow meter, and tubing connected to a mask.
BiPAP machines have similar components but also include a separate pressure control mechanism to manage both inspiratory and expiratory pressures. The compressor’s efficiency directly impacts the machine’s overall performance, while the pressure regulator ensures consistent pressure delivery.
Ease of Use and User Experience, What is the difference between cpap and bipap
CPAP machines are generally straightforward to use. Modern machines often feature intuitive controls, clear displays, and automated settings. BiPAP machines, with their dual pressure settings, may require a bit more adjustment. Patient training is crucial for both machines to maximize effectiveness. The user experience greatly impacts adherence to the treatment plan.
Types of Masks and Proper Fitting
A wide array of masks are available for both CPAP and BiPAP therapy. Common types include nasal masks, full face masks, and nasal pillow masks. Proper mask fitting is paramount for successful treatment. A well-fitting mask ensures a consistent seal around the nose and mouth, preventing air leaks and ensuring the prescribed pressure is delivered effectively. Incorrect fitting can lead to discomfort, skin irritation, and reduced treatment efficacy.
Mask Discomfort and Leaks
Mask discomfort and leaks are common challenges for patients using CPAP or BiPAP machines. Factors like mask size, material, and facial structure can contribute to discomfort. Proper mask selection and fitting are essential for minimizing these issues. Addressing mask-related issues through adjustments, different mask types, or specialized fitting techniques can improve user experience.
Machine Noise and Mitigation
Some CPAP and BiPAP machines can produce noticeable noise. The noise level can vary based on the machine model and the compressor’s performance. Several strategies can help reduce noise. Using a quieter machine model or placing the machine away from the bed can significantly reduce noise disturbance. Additionally, ensuring the machine is properly maintained can minimize noise issues.
Comparison of Mask Types
| Mask Type | CPAP | BiPAP |
|---|---|---|
| Nasal Mask | Suitable for most patients | Suitable for most patients |
| Full Face Mask | Suitable for patients with nasal issues or who leak with nasal masks | Suitable for patients with nasal issues or who leak with nasal masks, and potentially those who find full-face more comfortable |
| Nasal Pillow Mask | Suitable for patients with nasal issues | Suitable for patients with nasal issues |
This table summarizes the suitability of different mask types for CPAP and BiPAP, considering factors like facial structure and potential leakage. Individual needs and preferences should be considered alongside these general guidelines.
Long-Term Considerations and Maintenance
Long-term CPAP or BiPAP therapy success hinges on consistent use and proper maintenance. This isn’t a quick fix; it’s a commitment to a healthier, more restful life. Understanding the long-term aspects, from machine upkeep to potential side effects, is crucial for maximizing the benefits and minimizing any drawbacks.Consistent use is paramount to achieving lasting positive results. Adherence to the prescribed treatment plan, coupled with proactive maintenance, significantly improves the long-term effectiveness of these therapies.
Long-Term Effectiveness of Therapy
CPAP and BiPAP therapies, when used consistently, offer long-term improvements in sleep quality and overall health. Patients often experience reduced daytime sleepiness, improved cognitive function, and better cardiovascular health over time. Studies have shown that sustained use leads to a noticeable reduction in sleep apnea-related complications like high blood pressure and heart problems.
Importance of Consistent Use
Adherence to the prescribed treatment plan is critical for long-term effectiveness. Missing treatments or using the devices inconsistently can hinder progress and potentially negate the positive effects of the therapy. Regular use allows the body to adapt to the pressure support, promoting improved breathing patterns and a better night’s sleep. This consistency is often a key factor in patient satisfaction and successful long-term management of sleep apnea.
Factors Influencing Treatment Adherence
Several factors can impact treatment adherence. These include the complexity of the equipment, the perceived effort required for daily use, and the potential for discomfort or side effects. Furthermore, patient education, support systems, and a strong doctor-patient relationship all contribute to successful long-term adherence.
Maintaining CPAP and BiPAP Machines
Regular maintenance of the CPAP or BiPAP machine is vital for optimal performance and prolonged device lifespan. This includes proper cleaning of the machine and its components.
Maintaining CPAP and BiPAP Machines – Step-by-Step Guide
| Task | Description |
|---|---|
| Cleaning the Mask | Thoroughly clean the mask according to the manufacturer’s instructions. This usually involves using mild soap and water, or a specific mask cleaner. Avoid harsh chemicals. |
| Cleaning the Machine | Clean the machine according to the manufacturer’s instructions. This typically involves removing the water reservoir, cleaning it, and reassembling the machine. |
| Filter Replacement | Replace filters as recommended by the manufacturer. Filters prevent dust and other particles from entering the machine, ensuring optimal airflow and extending the machine’s lifespan. |
| Humidifier Care (if applicable) | Follow the manufacturer’s instructions for cleaning and maintaining the humidifier. This usually involves regularly cleaning the humidifier reservoir and replacing water to prevent bacterial growth. |
Potential Long-Term Side Effects and Mitigation
While CPAP and BiPAP therapies are generally safe, some patients may experience temporary side effects such as nasal dryness, mask leaks, or discomfort. Nasal dryness can be mitigated by using a humidifier, while mask leaks can often be resolved with adjustments to the mask fit. Consult your healthcare provider if any side effects persist or worsen.
Final Summary
In conclusion, understanding the nuances of CPAP and BiPAP is vital for navigating sleep apnea treatment effectively. Choosing the right therapy requires a careful consideration of your individual needs and sleep apnea severity, guided by a physician. This comprehensive comparison provides a starting point for making an informed decision, but always consult a medical professional for personalized advice.