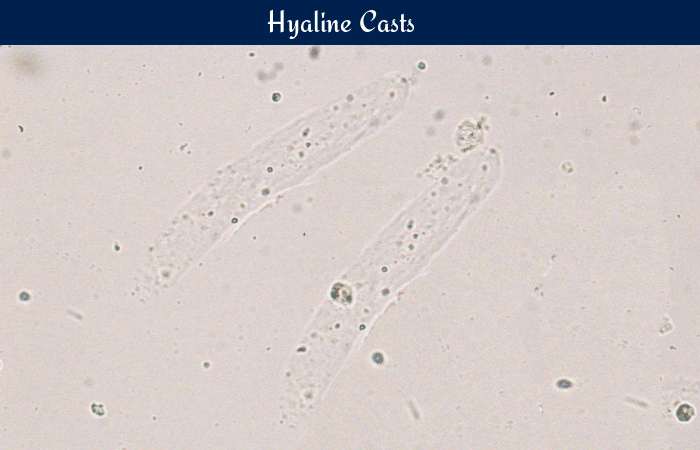
Hyaline casts in urine are a common finding in urinalysis, often prompting further investigation. These microscopic structures, essentially protein-filled tubes, can offer valuable clues about a patient’s overall health. Understanding their appearance, formation, and significance is crucial for accurate diagnosis and effective treatment. This comprehensive guide explores the multifaceted aspects of hyaline casts, from their definition and characteristics to their role in medical diagnosis, formation, differential diagnosis, and illustrative case studies.
The presence of hyaline casts in urine, while sometimes benign, can also signal underlying conditions such as dehydration or kidney stress. This article will explore the diverse scenarios where these casts appear, offering a clear and concise overview. The information presented will empower readers with a deeper understanding of these important indicators in the realm of medical diagnostics.
Hyaline Casts in Urine: Definition and Characteristics
Hyaline casts are a common finding in urine sediment analysis, often appearing in healthy individuals. These casts are essentially protein-based structures that form in the renal tubules. Understanding their characteristics, including their appearance, composition, and potential significance, is crucial for interpreting urine analysis results.
Definition of Hyaline Casts
Hyaline casts are cylindrical structures formed within the renal tubules of the kidney. They are composed primarily of a protein-rich matrix, primarily Tamm-Horsfall protein. This matrix is translucent and colorless. Hyaline casts are a normal constituent of urine in healthy individuals, though their presence can be indicative of other conditions as well.
Microscopic Appearance
Hyaline casts are typically transparent and colorless, appearing as thin, homogeneous, and cylindrical structures under a microscope. Their size and shape can vary, but they are generally straight or slightly curved. They often have a slightly refractile (light-bending) quality.
Composition of Hyaline Casts
The primary component of hyaline casts is Tamm-Horsfall protein, a glycoprotein produced by the tubular epithelial cells in the kidneys. This protein forms a matrix that gives the casts their characteristic shape. Minor amounts of other proteins, like albumin, might also be present.
Size and Shape Variations
Hyaline casts can vary in size, ranging from a few micrometers to several tens of micrometers in length. Their shape is usually straight or slightly curved. The width of the casts also varies and can range from narrow to broader, but the structure remains cylindrical.
Differentiating Hyaline Casts from Other Cast Types
Distinguishing hyaline casts from other types of urinary casts is vital for accurate diagnosis. Hyaline casts are readily distinguishable from granular casts, which exhibit a granular appearance due to cellular debris. Waxy casts, another type, are broader and have a more irregular shape. Epithelial casts are characterized by the presence of epithelial cells within their structure, unlike hyaline casts.
Furthermore, the presence of blood cells or bacteria within the casts can also help differentiate them.
Comparison Table of Urinary Casts
| Cast Type | Description | Appearance | Possible Causes |
|---|---|---|---|
| Hyaline Casts | Cylindrical structures composed primarily of Tamm-Horsfall protein; typically transparent and colorless. | Thin, homogeneous, cylindrical, straight or slightly curved; transparent, colorless. | Normal finding in healthy individuals; dehydration; mild exertion; strenuous exercise; fever; and some medications. |
| Granular Casts | Result from the degeneration of cellular material within the renal tubules. | Appear granular or fragmented, often exhibiting a granular or fragmented appearance; can be various shades of yellow, tan, or brown. | Acute tubular necrosis; glomerulonephritis; pyelonephritis; chronic kidney disease; and nephrotic syndrome. |
| Waxy Casts | Broad, irregular, and often have a “ground-glass” appearance; formed from the aggregation of granular casts. | Broad, irregular, often with a “ground-glass” appearance; usually pale yellow to light brown; more opaque than hyaline casts. | Chronic kidney disease; severe kidney damage; and nephrotic syndrome. |
Significance in Medical Diagnosis
Hyaline casts, though seemingly innocuous, can hold crucial diagnostic value in assessing a patient’s overall health status. Their presence in urine often signals underlying conditions affecting the kidneys or the urinary tract. Understanding the context of these casts, their potential causes, and their correlation with other symptoms is vital for accurate diagnosis and effective treatment.Hyaline casts are primarily composed of protein and cellular debris, forming cylindrical structures that are essentially harmless in small quantities.
However, their presence in high concentrations or alongside other abnormalities can point to various medical issues. Their presence in urine samples is not a disease itself, but a symptom that indicates a potential problem within the urinary system.
Hyaline casts in urine are pretty common, often a sign of something benign like dehydration. However, if you’re experiencing pain on top of your foot, like a sharp stabbing sensation, it could be a completely different issue. For instance, conditions causing pain on top of the foot, such as pain on top of foot , could potentially be unrelated to the presence of hyaline casts, though both could stem from underlying health issues.
It’s important to remember that hyaline casts alone usually aren’t a cause for major concern, but always check with a doctor for proper diagnosis and treatment.
Clinical Significance of Hyaline Casts
Hyaline casts, in themselves, are not inherently pathological. Their presence in trace amounts is often a normal response to temporary conditions such as dehydration or strenuous exercise. However, their persistent or excessive presence warrants further investigation.
Conditions Commonly Associated with Hyaline Casts
Several conditions can lead to the appearance of hyaline casts in urine. These conditions can range from benign to more serious. Factors influencing the appearance of these casts include temporary dehydration, recent strenuous exercise, or underlying health issues.
Potential Causes of Hyaline Casts
Several factors can contribute to the presence of hyaline casts in urine. Temporary conditions like dehydration or strenuous exercise can cause a temporary increase in the number of casts. More significant issues, such as kidney infections or glomerulonephritis, can also result in the presence of hyaline casts.
Correlation between Hyaline Casts and Overall Health
The presence of hyaline casts, while not always indicative of a severe problem, should be considered within the context of a patient’s overall health status and other symptoms. For instance, if a patient experiences frequent episodes of hyaline casts, accompanied by other symptoms like blood in the urine (hematuria), or proteinuria, it may signal a more serious underlying condition requiring further investigation.
Consider the frequency of their appearance and the presence of other symptoms when evaluating the clinical significance.
Examples of Situations Where Hyaline Casts Might Indicate Underlying Conditions
A patient with a history of hypertension and experiencing persistent hyaline casts, along with elevated blood pressure readings, may require further investigation for potential kidney damage. Likewise, a patient with a recent history of urinary tract infection (UTI) exhibiting hyaline casts in urine alongside other symptoms like fever and pain, warrants careful evaluation for potential complications.
Table of Common Conditions Associated with Urinary Casts
| Condition | Cast Type | Description |
|---|---|---|
| Dehydration | Hyaline Casts | Temporary increase in hyaline casts due to reduced urine output. |
| Acute Kidney Injury (AKI) | Granular Casts | Presence of granular casts indicates damaged kidney tubules, often associated with AKI. |
| Glomerulonephritis | Hyaline Casts, RBC Casts, Protein Casts | Inflammation of the glomeruli in the kidneys, potentially leading to the presence of various types of casts. |
| Pyelonephritis | WBC Casts | Presence of white blood cell casts indicates infection within the kidney. |
| Nephrotic Syndrome | Protein Casts | Significant protein loss in urine, often accompanied by protein casts. |
Formation and Pathophysiology
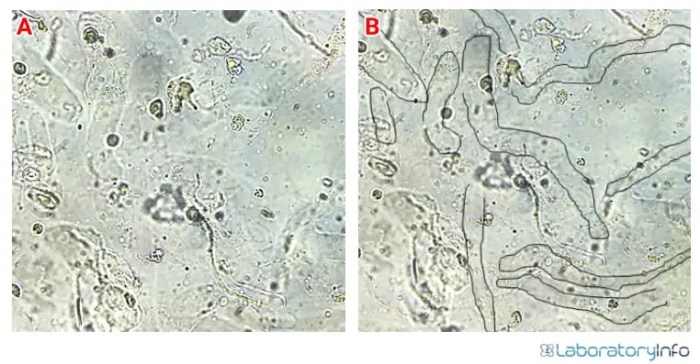
Hyaline casts, those enigmatic translucent cylinders found in urine, are more than just an intriguing microscopic sight. Understanding their formation and the underlying pathophysiology is crucial for accurate medical diagnosis and effective patient management. This section delves into the process of hyaline cast formation, highlighting the role of tubular epithelial cells and the pathophysiological mechanisms that contribute to their presence.
We will also compare hyaline cast formation with other types of casts, providing a comprehensive overview.Tubular epithelial cells play a pivotal role in the delicate balance of kidney function. These cells line the renal tubules and actively participate in the filtration, reabsorption, and secretion processes. Any disruption in their normal functioning can have a cascading effect, influencing the formation of various urinary constituents, including hyaline casts.
Hyaline Cast Formation in the Kidney
Hyaline casts originate in the renal tubules, the intricate filtering units of the kidney. The process typically begins with the accumulation of protein within the tubular lumen. This accumulation can stem from a variety of factors, such as dehydration, inflammation, or proteinuria. The protein, often a combination of serum proteins and Tamm-Horsfall protein (secreted by the tubular epithelial cells), forms a matrix within the tubules.
Hyaline casts in urine are a common finding, often nothing to worry about. They’re essentially protein-filled tubes, sometimes appearing when your body is a bit dehydrated, which can happen if you’re not careful when running outside in extreme cold. Checking out resources on when is it too cold to run outside might help you understand the importance of staying hydrated when exercising.
However, if these casts appear frequently or with other symptoms, it’s always a good idea to see a doctor.
This protein-rich matrix then undergoes a process of dehydration and aggregation, leading to the formation of the characteristic hyaline casts.
Role of Tubular Epithelial Cells
Tubular epithelial cells are integral to hyaline cast development. These cells not only contribute to the protein content within the tubules but also influence the environment within the tubules. Changes in their activity, such as those triggered by inflammation or ischemia, can lead to increased protein leakage into the tubular lumen. Moreover, altered cell shedding and desquamation can further contribute to the protein accumulation, thus creating an ideal environment for cast formation.
Pathophysiological Mechanisms
Several pathophysiological mechanisms can contribute to the presence of hyaline casts. Dehydration, a common condition, reduces urine volume, leading to increased protein concentration within the tubules. Proteinuria, the presence of excessive protein in the urine, directly increases the amount of protein available for cast formation. Inflammation of the renal tubules, a common response to infection or injury, can damage tubular epithelial cells, increasing protein leakage and cast formation.
Comparison with Other Cast Types, Hyaline casts in urine
While hyaline casts are composed primarily of protein, other casts have distinct compositions and origins. Granular casts, for example, are characterized by the presence of granular material, reflecting cellular breakdown within the tubules. Waxy casts, on the other hand, indicate a more advanced stage of renal damage, often characterized by a more homogenous and brittle structure. Fatty casts are composed of lipids and are indicative of fat or lipid abnormalities.
Understanding these differences is critical for accurately interpreting the presence of casts in urine samples.
Diagram of Hyaline Cast Formation
[Imagine a diagram here showing the renal tubule. The diagram would show the normal lining of epithelial cells. Then, under conditions of stress (e.g., dehydration or inflammation), proteins leak into the lumen. The proteins aggregate, dehydrate, and form a homogenous, transparent cast. The cast would be depicted as a cylinder-shaped structure within the tubule.]
Factors Influencing Hyaline Cast Formation
The formation of hyaline casts is influenced by a complex interplay of factors. These factors can be categorized as:
| Factor | Mechanism | Impact |
|---|---|---|
| Dehydration | Reduced urine volume, increased protein concentration in the tubules. | Increased risk of hyaline cast formation. |
| Proteinuria | Increased protein in the urine, leading to higher protein content within the tubules. | Directly contributes to cast formation. |
| Inflammation | Damage to tubular epithelial cells, increased protein leakage into the tubules. | Promotes cast formation. |
| Ischemia | Reduced blood flow to the kidneys, affecting tubular cell function. | Can increase protein leakage and cast formation. |
Differential Diagnosis and Treatment
Hyaline casts, while often benign, can sometimes signal underlying kidney issues. Distinguishing between harmless and significant causes is crucial for effective management. A comprehensive diagnostic approach, coupled with appropriate treatment strategies, is essential for patient well-being.
Conditions Mimicking Hyaline Casts
Hyaline casts aren’t always indicative of a specific disease. Several conditions can produce similar findings, making differential diagnosis vital. These include strenuous exercise, dehydration, and recent fever. Understanding these non-pathological factors is essential for accurate interpretation. For example, a healthy individual experiencing dehydration might exhibit hyaline casts in their urine, but this isn’t necessarily a cause for concern.
Diagnostic Approach
A systematic diagnostic approach is necessary to determine the underlying cause. This involves a thorough patient history, physical examination, and relevant laboratory tests beyond the urine analysis. Blood tests, including kidney function tests (creatinine, BUN), are crucial for evaluating kidney health. Imaging studies, such as ultrasound or CT scans, might be required to assess the kidneys and urinary tract for structural abnormalities.
Hyaline casts in urine can be a fascinating, albeit slightly unsettling, sign that something’s going on. While they often aren’t cause for immediate alarm, they can sometimes indicate a kidney issue. Learning more about the potential causes, like kidney disease, can be quite helpful. Of course, a more serious condition like metastatic breast cancer might also sometimes show up in these casts, which makes the question of is chemotherapy used to treat metastatic breast cancer crucial.
Ultimately, a doctor’s diagnosis is key, and further investigation will likely be needed to understand the complete picture. So, if you notice hyaline casts, don’t panic, but do schedule a check-up.
A detailed medical history can often provide valuable clues, identifying any pre-existing conditions or recent illnesses that could contribute to the presence of hyaline casts.
Treatment Strategies
Treatment strategies depend entirely on the underlying cause. For instance, if dehydration is the culprit, rehydration therapy is sufficient. If the cause is a more serious condition like diabetes or hypertension, the treatment focuses on managing these underlying medical problems. The treatment strategy will vary considerably depending on the root cause, ranging from simple lifestyle adjustments to complex medical interventions.
Medical Interventions
Medical interventions are tailored to the specific condition. For hypertension, antihypertensive medications are prescribed. For diabetes, insulin therapy or oral hypoglycemic agents are employed. Addressing underlying conditions through appropriate medical interventions is crucial. If the hyaline casts are a symptom of a urinary tract infection, antibiotics are necessary.
This example highlights the importance of targeted treatment based on the underlying cause.
Alternative Treatment Options
In some cases, alternative or complementary therapies might be considered, but these should always be discussed with the physician. Dietary modifications and herbal remedies, for example, could be part of a comprehensive approach to managing the underlying condition. The decision to incorporate alternative therapies should be made cautiously, in consultation with the physician.
Comparison of Treatment Effectiveness
The effectiveness of different treatment strategies depends on the cause. For example, rehydration is highly effective for treating dehydration-induced hyaline casts. For more complex conditions, a multi-faceted approach involving medication, lifestyle modifications, and possibly surgery is often necessary. Monitoring the patient’s response to treatment is essential for evaluating its effectiveness.
Diagnostic Flowchart
The following flowchart provides a simplified illustration of the diagnostic process:
| Step | Action | Possible Outcomes |
|---|---|---|
| 1 | Obtain comprehensive patient history and physical examination | Suspected underlying condition, or no suspected condition |
| 2 | Perform urinalysis and blood tests (including kidney function tests) | Hyaline casts present, normal results |
| 3 | Evaluate results, identify potential causes | Dehydration, underlying medical condition, no significant findings |
| 4 | If underlying condition suspected, perform further tests (e.g., imaging) | Confirmation or exclusion of underlying condition |
| 5 | Develop a personalized treatment plan based on the underlying cause | Rehydration, medication, lifestyle modifications, or further investigation |
Illustrative Cases and Examples
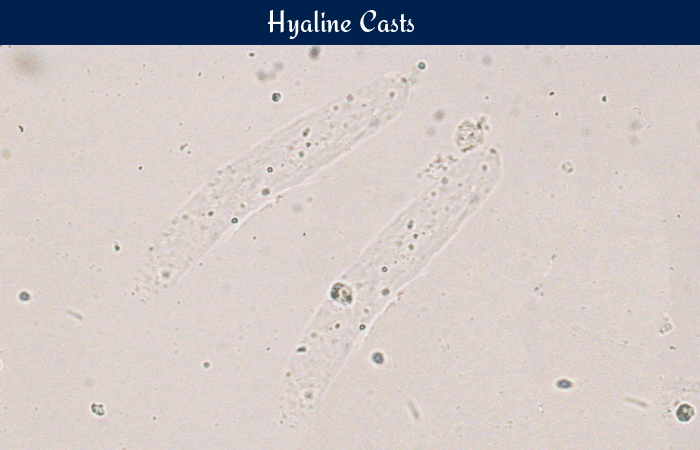
Hyaline casts, while often considered a benign finding in urine analysis, can be a significant indicator of underlying conditions. Understanding their presence in various clinical scenarios is crucial for accurate diagnosis and effective patient management. These cases highlight the importance of considering the complete clinical picture when evaluating hyaline casts.Hyaline casts are frequently observed in individuals experiencing mild dehydration, strenuous exercise, or even stress.
However, their presence, especially in combination with other symptoms or a specific medical history, may point towards more serious pathologies. The following cases illustrate diverse scenarios where hyaline casts play a diagnostic role.
Case 1: The Athlete
A 25-year-old male athlete presented with mild flank pain and fatigue following a marathon. His urine analysis revealed numerous hyaline casts, alongside a slightly elevated creatinine level. The athlete reported no history of kidney disease or other significant medical issues. The hyaline casts in this case likely resulted from the strenuous physical activity and subsequent dehydration. Treatment involved increased fluid intake, and the casts resolved within a few days as the athlete’s hydration improved.
This case demonstrates how hyaline casts can be a normal response to strenuous exercise and dehydration.
Case 2: The Elderly Patient with Hypertension
A 72-year-old female with a history of hypertension and diabetes presented with edema and frequent urination. Her urine analysis showed the presence of hyaline casts, proteinuria, and microscopic hematuria. The patient’s symptoms, combined with her medical history, strongly suggested kidney damage related to her long-standing hypertension and diabetes. Further diagnostic tests, including renal ultrasound and blood tests, confirmed chronic kidney disease.
Treatment focused on managing blood pressure and blood sugar levels, along with supportive care to alleviate symptoms. This case highlights the potential link between hyaline casts and chronic kidney disease, particularly in patients with a pre-existing history of hypertension or diabetes.
Case 3: The Patient with Urinary Tract Infection
A 30-year-old female presented with symptoms of a urinary tract infection (UTI), including dysuria, frequency, and urgency. Her urine analysis revealed hyaline casts, leucocytes, and bacteria. The hyaline casts in this case were likely a non-specific finding associated with the inflammatory response triggered by the UTI. Treatment involved antibiotic therapy targeting the identified bacteria, and the hyaline casts resolved as the infection subsided.
This case illustrates how hyaline casts can be a nonspecific finding in the context of a urinary tract infection.
Case 4: The Patient with Systemic Lupus Erythematosus
A 45-year-old female with a history of systemic lupus erythematosus (SLE) presented with progressive renal dysfunction. Her urine analysis showed hyaline casts, proteinuria, and hematuria. The presence of hyaline casts, combined with the patient’s SLE diagnosis and renal symptoms, indicated a potential lupus nephritis. Further testing confirmed the diagnosis. Treatment involved immunosuppressant medications and close monitoring of renal function.
This case emphasizes the importance of considering underlying autoimmune conditions in the presence of hyaline casts, especially in patients with a known history of autoimmune diseases.
Different Scenarios with Hyaline Casts
Hyaline casts can be observed in various scenarios, and their significance varies based on the clinical context. Dehydration, strenuous exercise, and stress can cause transient hyaline casts, while persistent or recurrent hyaline casts with other abnormalities in urine analysis often suggest underlying renal conditions. The following table summarizes these scenarios:
| Scenario | Possible Causes | Significance |
|---|---|---|
| Dehydration | Reduced urine volume | Transient finding; resolves with hydration |
| Strenuous exercise | Increased urine flow and concentration | Transient finding; resolves with rest and hydration |
| Stress | Physiological response | Transient finding; resolves with stress reduction |
| Underlying Renal Conditions | Chronic kidney disease, glomerulonephritis, lupus nephritis | Possible indicator of renal damage |
Final Review
In conclusion, hyaline casts in urine, while often a non-alarming finding, can be a critical indicator of potential health issues. This discussion has highlighted their various characteristics, medical significance, and underlying causes. From their microscopic appearance to their diagnostic implications, this exploration provides a holistic view of these urinary constituents. Remember, if you or someone you know experiences symptoms that might be related to hyaline casts, it’s essential to consult with a healthcare professional for proper evaluation and treatment.