What is discogenic pain? This deep dive explores the complexities of this often-misunderstood back pain, examining its causes, symptoms, diagnosis, and treatment options. We’ll uncover the anatomical structures involved, the differences between types of discogenic pain, and the various approaches to managing this condition. Discogenic pain, originating from the spinal discs, can manifest in a…
Category: Health and Wellness
How Long Live Without Food Survival Limits
How long live without food? This question delves into the fascinating, and often grim, realities of human survival in the face of starvation. Our bodies are remarkably resilient, but how long can they withstand the absence of essential nutrients? This exploration examines the complex interplay of physiology, factors influencing survival, consequences of prolonged fasting, and…
Lower Back and Hip Pain Understanding the Causes and Relief
Lower back and hip pain can significantly impact daily life, causing discomfort and hindering movement. This comprehensive guide explores the various causes, symptoms, and treatment options available for managing this prevalent issue. We’ll delve into the musculoskeletal factors, inflammation, injuries, and lifestyle choices that contribute to this pain. We’ll also cover diagnostic methods, non-invasive treatments,…
Can You Live Without Your Pancreas? A Comprehensive Guide
Can you live without your pancreas? This comprehensive guide delves into the fascinating world of pancreatic function, the medical considerations for removal, lifestyle adjustments, long-term effects, and ethical considerations. We’ll explore the vital role the pancreas plays in digestion and hormone regulation, examining the necessary dietary changes and medical procedures involved in managing life without…
Rectal Ulcer Overview and More A Deep Dive
Rectal ulcer overview and more: Understanding rectal ulcers involves exploring their diverse types, common causes, and a range of potential symptoms. This comprehensive guide will delve into the complexities of these conditions, providing a detailed overview of diagnosis, treatment options, and preventative measures. From ischemic to inflammatory and infectious ulcers, we’ll uncover the factors contributing…
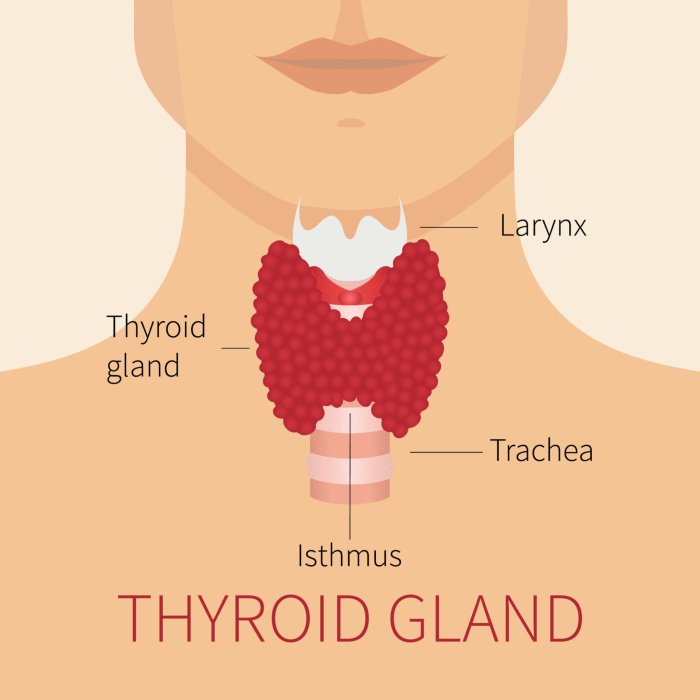
Thyroid Hormones Metabolism and Weight A Deep Dive
Thyroid hormones metabolism and weight are intricately linked. This exploration delves into the complex relationship between thyroid hormones, metabolism, and body weight, examining the biochemical pathways involved, the impact of imbalances, and various factors that influence thyroid function. Understanding this connection is crucial for managing weight and overall well-being. We’ll cover everything from the role…
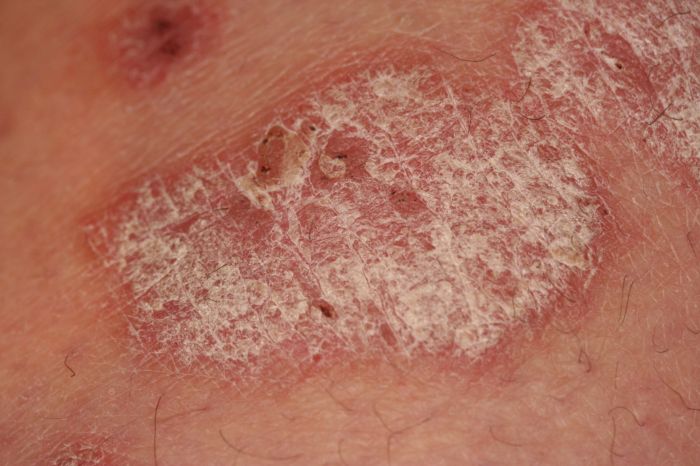
Psoriasis and Your Life A Deep Dive
Psoriasis and your life intertwine in profound ways, impacting everything from daily routines to emotional well-being. This exploration delves into the multifaceted nature of living with psoriasis, offering insights into its effects, treatment options, and the importance of coping strategies. We’ll navigate the challenges and triumphs of managing this condition, emphasizing the journey of adaptation…
When Should I Worry About Passing Too Much Gas?
When should I worry about passing too much gas? This common digestive issue can be frustrating, but understanding what’s normal and when to seek help is key. We’ll explore the science behind gas production, the signs that something might be amiss, potential underlying medical conditions, and lifestyle changes that can help manage it. From understanding…
Menopause Facts and Statistics A Deep Dive
Menopause facts and statistics paint a compelling picture of this significant life transition. From global prevalence rates and demographic breakdowns to the intricate interplay of symptoms, health impacts, and management strategies, this exploration provides a comprehensive overview. Understanding the realities of menopause empowers women and healthcare professionals alike. This deep dive examines the prevalence of…
High Blood Pressure Facts Your Guide
High blood pressure facts are crucial for understanding a silent health threat. This comprehensive guide dives deep into the causes, symptoms, and treatment options, offering practical strategies for prevention and management. Learn about different types, risk factors, and how lifestyle choices impact blood pressure readings. We’ll also explore the potential complications and preventative measures you…